Squamous cell carcinomas, keratinocytes derived tumours, are the second most common cancer of the skin. Unlike BCC, they care capable not just of invasion, but of metastasis. They are harder to diagnose than BCCs. The clinical stakes are raised…..
This chapter in one minute
Squamous cell carcinomas (SCC) are keratinocyte tumours that often appear on histological grounds to be more differentiated than basal cells. Remember the discussion about BCC and basal cells? Do not think from this first sentence that SCC are derived from terminally differentiated keratinocytes — if they were, they would be incapable of division.
Unlike basal cell carcinomas, SCCs are capable of metastasis, and they therefore have a higher mortality rate than BCCs.
Clinical vignette
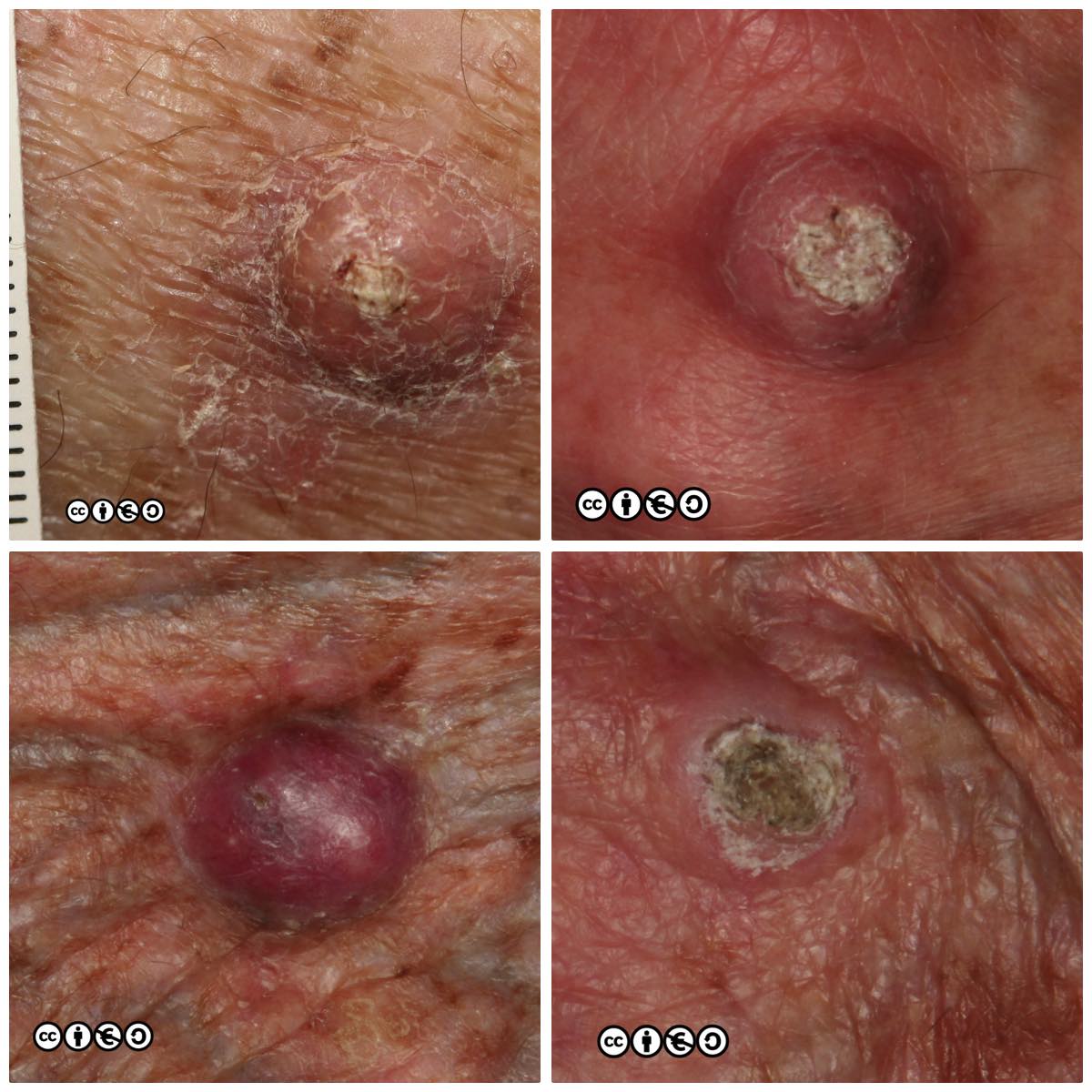
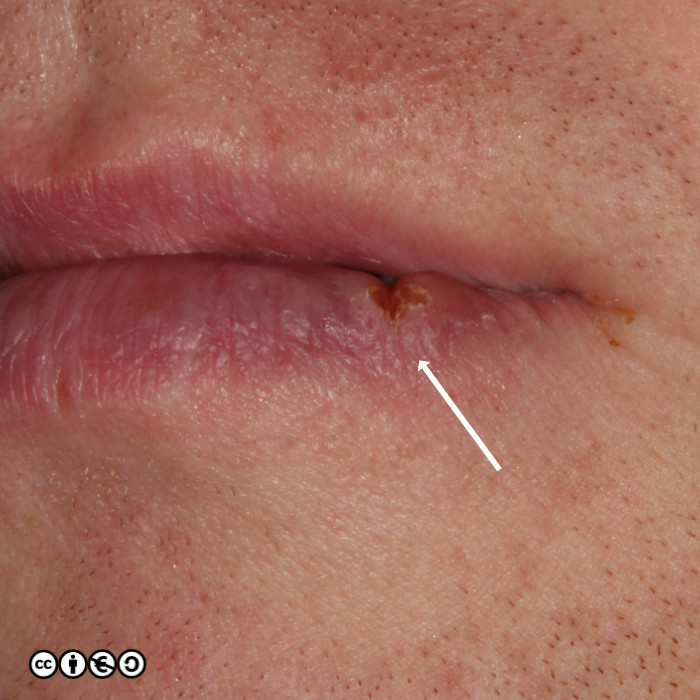
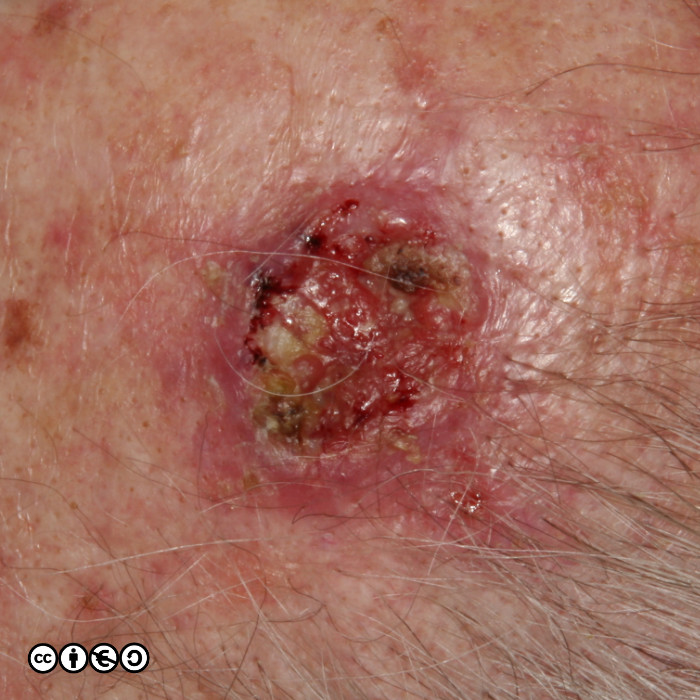
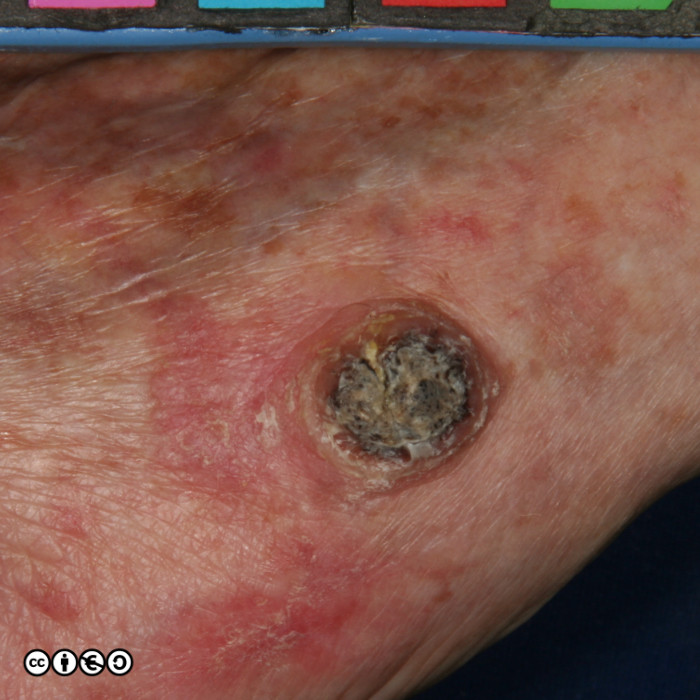
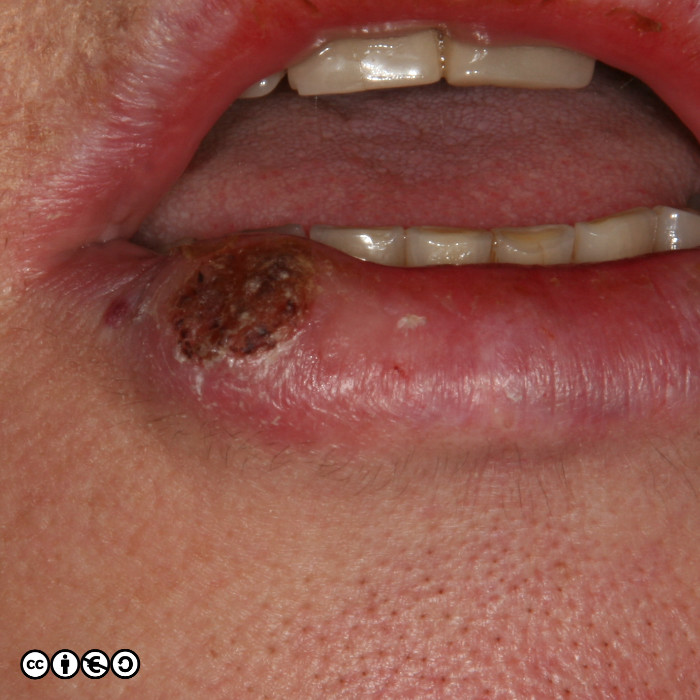
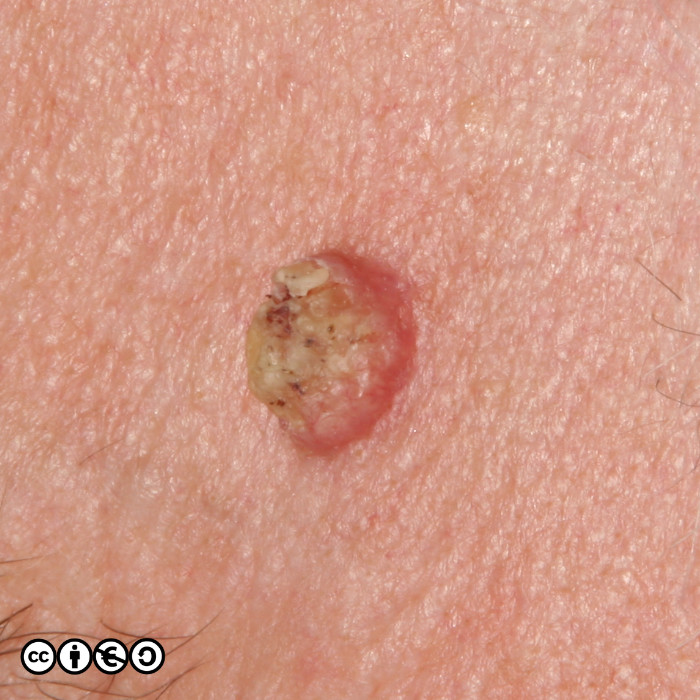
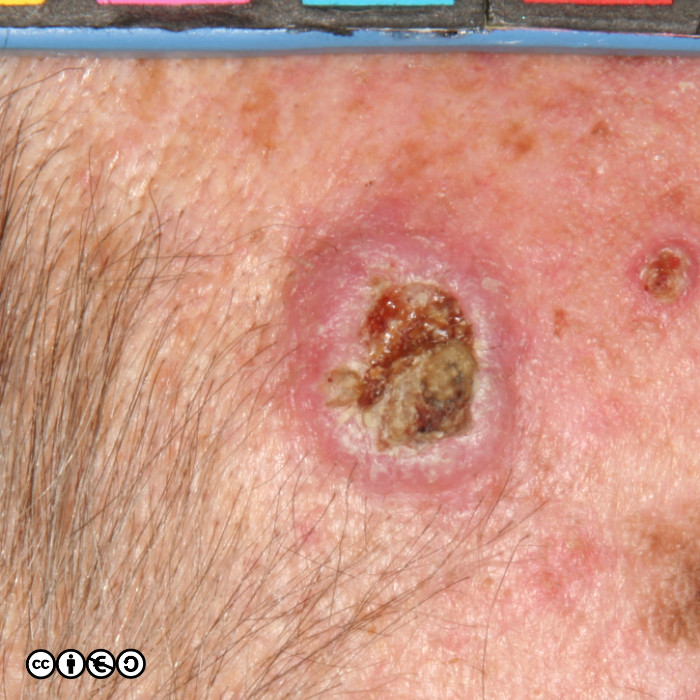
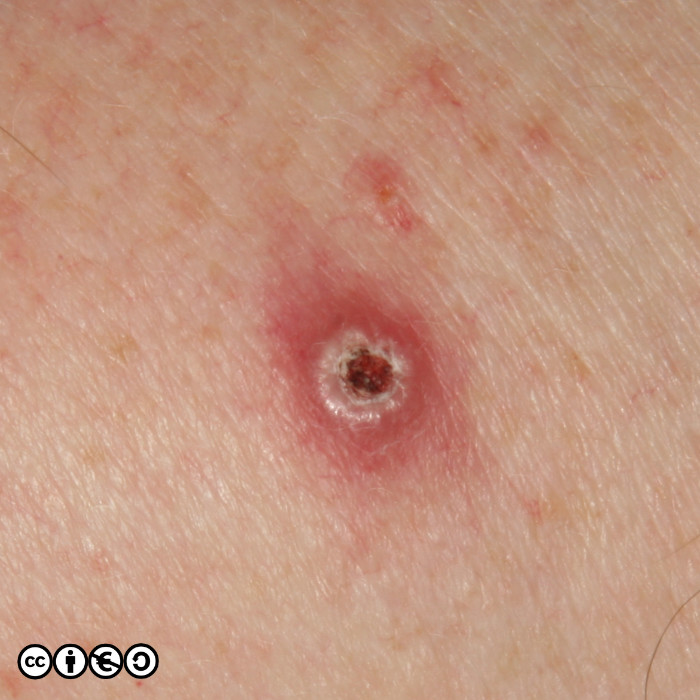
The typical SCC is a keratinising nodule that may be ulcerated or show excess ‘keratin’ formation. They are often referred to as “ugly” and “untidy” looking — often with a ‘yuck’ factor. Given their relation with high levels of cumulative UVR exposure, the surrounding skin may show many features of photodamage including dermal atrophy, and increased variation in pigmentation and of the skin vasculature. Their distribution strictly mirrors cumulative UVR exposure: rates are highest on bald headed men, the tops of the ears, faces and backs of the hands.
They are usually nodules, and vary in size from ~5mm up to 3 or 4cm or greater. Some poorly differentiated SCCs appear to have lost their ‘keratinising’ appearance and resemble a piece of raw steak or jam on the skin’s surface.
Some examples of squamous cell carcinomas are shown below.
Notice that in that many of the SCC images (above and below), the tumour seems to centre around a keratin plug, to form a volcano like structure. Whilst some SCCs are ‘smooth’, most show areas of hyperkeratotic material (‘keratin’). They can also be ulcerated.
Epidemiology
SCC are ~five times less common than BCC with an incidence of around 55:100,000 in the English population, with a median age of 80. They are more common in men than women (2:1).
SCC are most common on the sites that receive the largest amount of cumulative UVR such as the tops of the ears, face and back of hands. Their body site distribution therefore is identical to that of actinic keratoses — SCC precursor lesions we will deal with in the next chapter.
SCC are more strongly related to cumulative UVR than any other skin cancer.
UVR and sun sensitive skin account for the vast majority of SCC. There are however a number of other rarer causes further discussed below.
Clinical behaviour
SCC are both invasive and capable of metastasising and therefore of causing death. The mortality rate is ~0.5/100,000.
Perhaps 3-5% of SCC spread to local lymph nodes or beyond.
As a general rule, SCC of sun exposed skin are less aggressive than SCC of other keratinocyte derived tumours such as SCC of the cervix, mouth or oesophagus. The reason for this is unclear.
Treatment of SCC
SCC should be excised with a margin of normal tissue of 4-6 mm. This might mean that flaps or grafts are required (discussed in the earlier skin surgery chapter).
The only alternative to excision is — in some instances — radiotherapy. Some tumours (e.g. large ones, which are thick) are more likely to spread to local lymph nodes or metastasise, and are deemed ‘high risk’. You do not need to know the details, but such high risk tumours might be treated with local excision and local radiotherapy. We will return to therapy in a later chapter.
Some other things about SCC I should have mentioned
Precursor lesions: Whilst there are no clinically recognised precursors of BCCs, there are precursor lesions of SCCs: actinic keratoses and intraepithelial carcinoma. We are going to discuss these conditions more in the next chapter.
Immunosuppression: SCC are dramatically more common in those patients with organ transplants who are receiving immunosuppressives. Because immunosuppression itself may allow a tumour to behave more aggressively and SCC (unlike BCC) metastasise, SCC represent a significant mortality risk in this patient group. Management of such patients requires regular expert surveillance of the skin, advice on minimising UVR exposure and prompt surgical excision of any SCC that develop. In such patients both the clinical features and histopathological appearance of the tumours is more complex (than in immunocompetent individuals), and more caution in management is warranted (i.e. waver on the side of over, rather than undertreatment).
The increase in incidence in immunosuppressed persons is far greater for SCC than for BCC (or melanoma).
Inherited syndromes: There are no SCC specific inherited tumour suppressor syndromes as there are for malignant melanoma and basal cell carcinoma. SCC are however a feature of xeroderma pigmentosum (all UVR related skin cancers are increased in xeroderma pigmentosum).
For completion, but not for learning about, I would add that there is a very rare syndrome, the Ferguson Smith syndrome, with tumours that resemble SCC, but which behave very differently. Students do not need to know more. Some more details are here.
Carcinogens other than UVR: In areas with high levels of arsenic ingestion, cutaneous SCC (as well as SCC of other internal organs) are more common.
Patients who have received large amounts of PUVA (Psoralen +UVA) therapy are much more prone to SCC. The main group of patients affected is a cohort of patients from the 1980s and early 1990s when PUVA was — with hindsight — perhaps overused for the treatment of plaque psoriasis.
Carousel of 15 SCC images
Below are 15 images of SCCs. Click the (faint) arrows / chevrons half way down on the right or left sides of the image, or press on the grey blue buttons, to navigate. On an iPad ‘swipe’ sideways.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.