I introduced surgical therapies and briefly described some other therapeutic modalities in the earlier chapter on skin surgery. If you do not feel confident distinguishing excision from incision, or how shaves can be excisional or incisional, go back and check that chapter out again.
In this chapter I am going to delve a little more deeply into how we treat skin cancer and premalignant lesions. From a medical student’s perspective the key issue is to understand the principles rather than the details. This means understanding how treatment decisions are matched to the behaviour of any tumour type. In other words, not just the how, but the why.
I am going to start with melanoma, because it has the most in common with the management of other non-cutaneous cancers, some of which you should be familiar with. I will then move on to SCC, BCC and the dysplastic lesions.
Management of suspicious pigmented lesions and melanoma
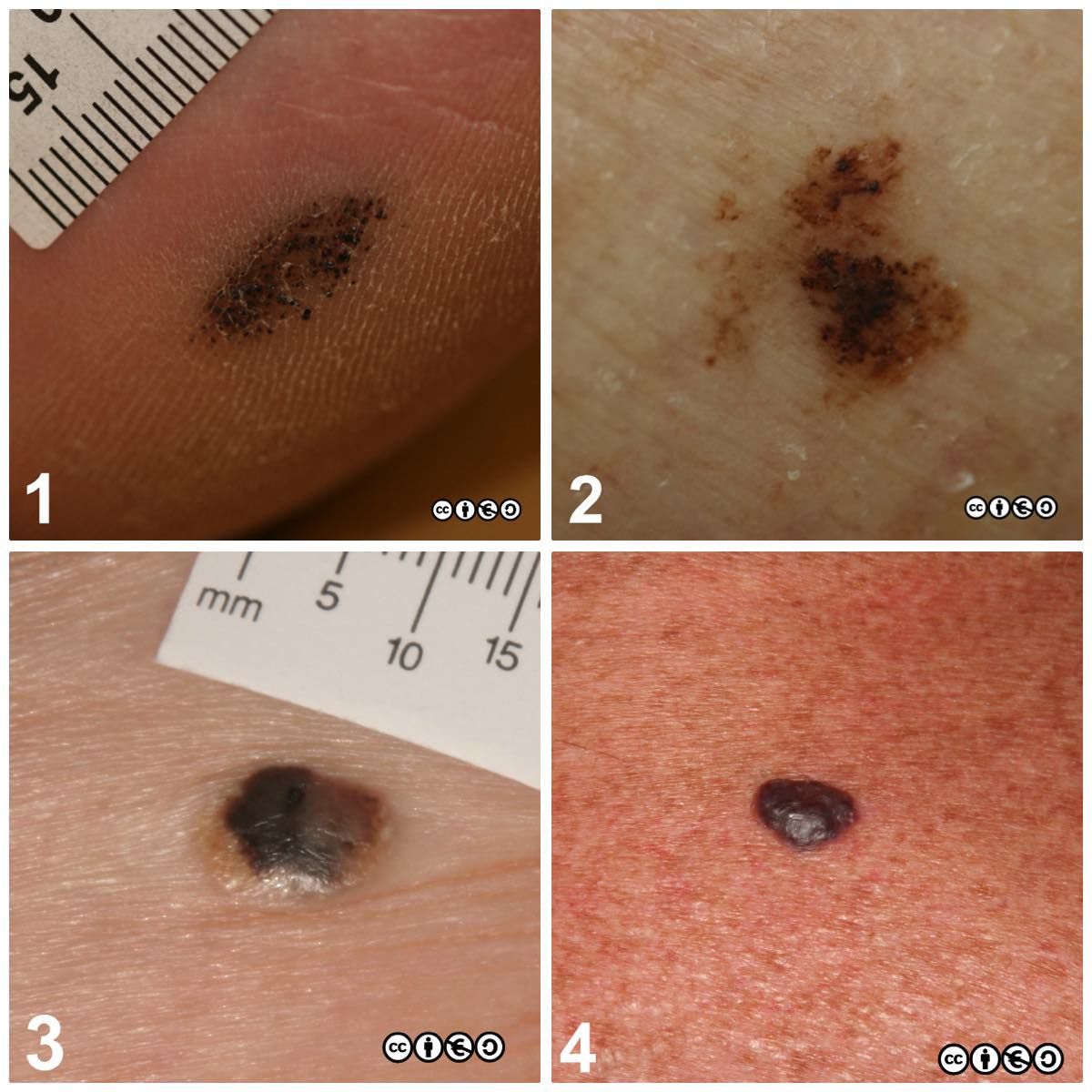
The first decision is to decide if the lesion is melanocytic or not. Many keratinocyte tumours are pigmented (with melanin), but they are not primary proliferations of melanocytes (note: this distinction is important). Shown below are four pigmented lesions. Only one is melanocytic.
It is usually — but not always — possible to make this distinction. How did you do?
- Lesion 1 is talon noir (“black heel”). Small collections of extravascular blood trapped within the thickened skin, usually seen in squash players over the achilles tendon. It is due to shearing forces. (non-melanocytic).
- Lesion 2 is an early melanoma — so a true melanocytic lesion.
- Lesion 3 is the greater mimic: a seborrhoeic keratosis (non-melanocytic).
- Lesion 4 is an angioma. The pigment is haemoglobin within the vessels (non-melanocytic).
But once you consider that a lesion could be a melanoma — and we all get it wrong sometimes — act as follows:
- If you are surgically competent in this domain of clinical practice, mark out the lesion margins and the lesion margins + 2mm, with a surgical marker pen. Now excise the lesion with a 2mm margin, and send for histopathological examination, marking the specimen urgent.
- You are asking the Dermatopathologist two key questions. First, is this a melanoma? Second, if it is a melanoma, what is the Breslow depth.
The dermatopathologist will provide other details, but for the non-expert these are the key points (is it a melanoma, and if it is, what is the Breslow thickness).
If the lesion is not a melanoma, either being benign or some other type of non-melanoma skin cancer, manage as described elsewhere.
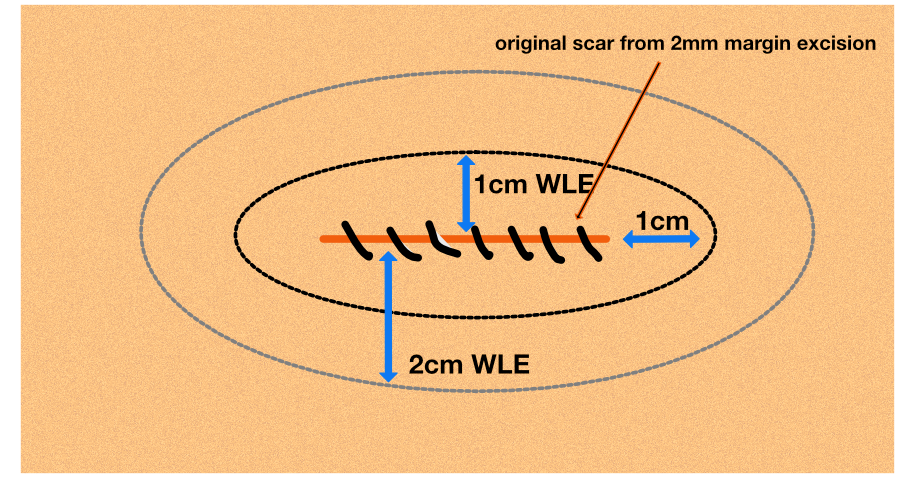
If the lesion is a melanoma, what you do next depends on the Breslow thickness, but will involve what is termed a wide local excision (WL). The wide local excision means the original scar is excised and a margin of normal skin taken. Usually the further surgery (WLE) will be down to the level of the superficial fascia.
- If the Breslow thickness is under 1mm, then a wide local excision with a 1cm margin is needed. Note, this 1cm margin is on all sides of the scar, so in effect the new defect has a diameter of 2cm.
- If the Breslow thickness is greater than 1mm, then usually a 2cm margin WLE (on all sides) will be required (defect diameter of 4cm).
Students do not need to memorise these margins, nor do they need to delve into the debate about whether sampling of lymph nodes is required or advisable, but you must understand the principles of initial biopsy with a 2mm excision, followed by a wide local excision if the diagnosis of melanoma is confirmed.
Avoid taking incisional biopsies of presumed melanomas
Incisional biopsies in melanoma are frowned upon for two reasons
- Histopathological diagnosis of melanocytic lesions is hard. There are often variations in the appearance in different parts of a melanoma. Incisional biopsies run the risk of being false negatives — a disastrous outcome.
- Further management, as I discussed above, is predicated on the exact Breslow thickness. If you only sample some of the lesion, you may underestimate the correct figure.
Having said this, sometimes incisional biopsies are unavoidable if the primary lesion is very large and on the face, because you do not want to mistakenly carry out major surgery only to find out that your diagnosis was incorrect (e.g. the lesion was benign).
Management: beyond surgery
For a primary lesion, with no clinical evidence of spread, surgery as described above is all that is required. Adjuvant therapy is not indicated. Although there are several new drugs, including those that target the BRAF signalling pathway (e.g. Vemurafenib) or Immune Checkpoint inhibitors (e.g. Ipilimumab), they are presently reserved for metastatic disease.
You do not need to know more, except for me to highlight that the oncological management of melanoma is in a state of flux. This is chiefly because the Immune Checkpoint Inhibitors — drugs that inhibit the natural inhibiting pathways of the immune system— have a dramatic effect in a minority of patients with metastatic disease. By ‘dramatic’ I mean that they seem to induce long-term remissions of tumours in some cases. For some patients these drugs are life-changing and time will tell whether permanent cures occur.
How much imaging and ‘searching’ for distant disease you do varies enormously between countries. Ignore such debates, but know that an initial presentation with detectable distal disease is unusual (<1%).
Patients with melanoma are at an increased risk of subsequent melanomas, so most centres follow patients up regularly for several years to search for new primaries and detect recurrences.
Prognosis
Prognosis is tightly tied to Breslow thickness — that is, the Breslow thickness is a proxy for whether a primary tumour has already spread, even if this spread is not detectable clinically or with imaging.
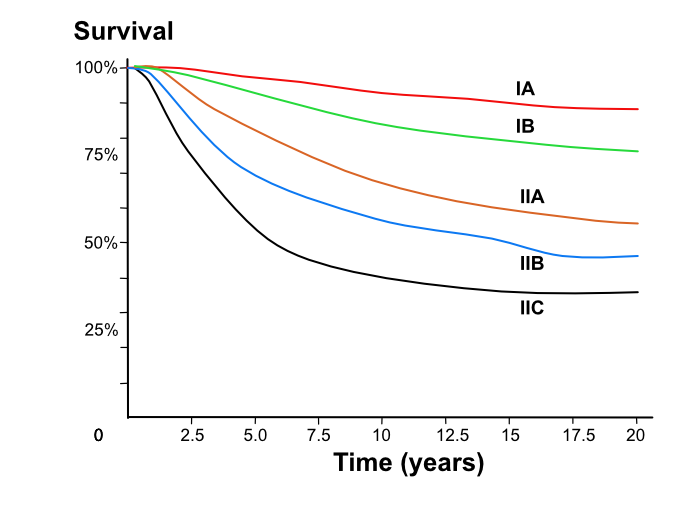
A schematic of survival is shown below. Do not memorise the figure, but note most patients with thin tumours do well, and that recurrence is often late (see the difference between 5 and 10 years).
5 year survival for melanoma is not sufficient (late recurrences occur).
Survival by stage. Stage IA is less than 1mm Breslow thickness, with no ulceration. Stage IIC, is Breslow >4mm with ulceraton. Other stages are intermediate. Redrawn from the 2009 AJCC Melanoma and Staging Classification.
Squamous cell carcinoma
Remember the biology: SCC can spread to local lymph nodes and metastasise distantly.
The treatment of choice for most SCC is excision, usually with a margin of around 5mm (you do not need to remember this figure). It is possible to identify tumours that are more likely to spread (‘high risk’). They tend to be larger than 2cm, they tend to have a depth greater than 4mm, and to be poorly differentiated, or occurring on the background of immunosuppression (you do not need to learn this list). In such high risk tumours, post operative radiotherapy may occasionally be considered, but surgery remain key. Adjuvant therapy is not indicated.
Basal cell carcinoma
Remember the biology: BCC ‘never’ metastasize but are destructive locally
Surgery has the highest success rate with cures in 98% of cases in expert hands. Again, clearance is best achieved by taking a margin of normal skin (usually 4mm — you do not need to learn the figure). Radiotherapy is also occasionally used — and perhaps underused.
Because most BCC occur on the middle third of the face, a good aesthetic outcome assumes some importance. Flaps or grafts may be required, but a particular type of surgery called Mohs’ micrographic surgery is often employed. This is a technique aimed at tissue conservation and ensuring adequacy of margins.
Although we do not expect you to know the details of Mohs, understanding why it is used will teach you some key facts about non-Mohs surgery. Watch the following video to learn more.
Dysplastic lesions (actinic keratoses, intraepithelial carcinoma)
Remember the biology: low risk lesions
Earlier, I highlighted that although people may dispute the exact figure, the chance of progression of an actinic keratosis to a squamous cell carcinoma is very low. The figure for intraepithelial carcinoma is slightly higher, but the risk is small.
Surgical options for these lesions include curettage and cautery. Although this technique does not allow examination of margins (see video above), the cure rate is so high and the risk so low that it is often an appropriate management. Excision for some dysplastic lesions is still appropriate, and lesions misdiagnosed as squamous cell carcinomas, may still end up being excised, too.
Other management options for dysplastic lesions are described below. You should be aware of these options, but do not delve any deeper.
Beyond the knife
The above sections can largely be paraphrased as saying: skin cancer is treated by excision — usually. Indeed, I often tell students, that saying “surgery” as the answer to a question about the management of any malignant or dysplastic skin lesion is seldom far from the truth.
There are however some non-surgical modalities that are used for BCC and some of the premalignant lesions. As ever, note how therapy is being matched to biological behaviour.
Cryotherapy
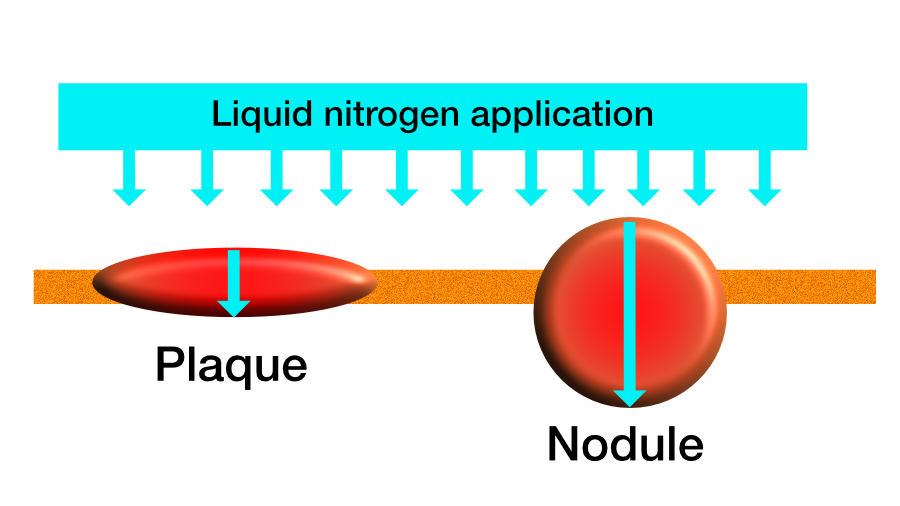
Cryotherapy has been mentioned in an earlier chapter. As the figure below highlights, superficial plaque like lesions often do better with cryotherapy than the thicker nodular lesions. The reason is simple: since the liquid nitrogen is being applied from one direction only, it is hard for the cold to penetrate to the bottom of deeper lesions. (see figure below).
So, some superficial BCCs and premalignant lesions such as actinic keratoses or intraepithelial carcinomas can be readily managed with cryotherapy. It is not suitable for squamous cell carcinomas, nor melanomas(!). Cryotherapy is destructive and will alter the physical signs if it does not clear the lesion, therefore:
do not use cryotherapy unless you are certain of the diagnosis.
Topical chemotherapeutic agents
There are a range of topical chemotherapeutic agents now available. You do not need to know the precise indication, not details of prescribing — but you should be familiar with their names and their existence.
Imiquimod is a topical agent that stimulates the innate and adaptive immune system. It has potent anti-tumour and antiviral actions. It was originally introduced as a treatment for anogenital warts, but is now used to treat actinic keratoses, IEC, and some superficial basal cell carcinomas. There are various treatment options but all involve multiple applications per week for over one month. It provokes pronounced local inflammation and a flu like malaise in some patients (enough to warrant stopping the treatment, on occasions).
5-Fluorouracil (5FU) is a pyrimidine base analogue that inhibits DNA and RNA synthesis. It is used as a systemic agent in oncology but as a topical agent is effective against AKs, superficial BCCs and some cases of IEC. It needs to be used over extended periods (i.e. a month) and it provokes a prominent inflammatory response which limits its acceptability. It can play a valuable role in treating large areas of skin in which the development of NMSC is occurring at multiple places (so called ‘field change’).
Ingenol mebutate is an inducer of cell death and can be used to treat actinic keratoses. Like many other topical agents it provokes a prominent inflammatory reaction.
Topical non-steroidals Drugs such as diclofenac have antitumour effects in many animal model systems. Applied topically to human skin, they have very modest therapeutic actions agains actinic keratoses.
Photodynamic therapy. In this modality topical porphyrins are applied to the skin and then visible light shone on the tumour. Because porphyrins are selectively absorbed by the tumour the treatment is relatively selective. Side effects include pain, and again, the treatment is only suitable for superficial lesions.
As a general rule, all the above topical agents have only a marginal role in the treatment of most NMSC, but are more useful for dysplastic lesions.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.