At this stage you might be feeling that you have this skin cancer thing all sorted. There are a few different cancers (melanoma, BCC and SCC), and many of these different tumour types look different from each other. Black things are usually melanomas and, in any case, since I have said surgery is usually the definitive treatment, if there is any diagnostic confusion, just cut all of them out and let the pathologist sweat the hard work……. Besides these cancers don’t look like anything on your own skin, so what is the big deal?
Sadly, I have news for you: life is not so simple.
This chapter in one minute
What's in a name?
The clinician’s problem is not so much that she has to distinguish between different types of skin cancer (although this is sometimes hard) but that the clinician has to distinguish between normality (i.e. non-cancer) and any type of cancer. This latter task is usually much harder, largely due to the myriad of marks and lesions that are part of normal skin. This chapter and the next one is going to introduce you to these non-cancer ‘normal’ lesions, so that in a later chapter (‘The clinician’s approach) we can put it all together ready to do some (virtual) clinics together.
Much as though it might offend some, the chief purpose of the next two chapters is not to delve deeply into the biology of all these myriad marks and lesions that adorn human skin, but to enable you to attach a label to the common ones. The purpose of the name — when correctly applied — is simply to allow those of us in the clinic to identify the lesion as non-cancer, and to cease any further diagnostic search. In this particular context, attaching the correct name allows you and the patient to stop worrying that a lesion might be cancer and literally, to move on. Let me suggest an example of what we are about.
Domestic cats and lions have important biological differences, but if my partner told me that one of these two species was in our back garden, I would feel happier knowing I could trust her to be able to name the two species accurately. I would also argue that this was not the time for an exploration of the wonders of human biology and what genetic ancestry the two species have in common have in common, but rather a time for a binary decision about the need to barricade ourselves in the house. Or not.
In this chapter I deal mainly with lesions that are pigmented due to the presence of melanin. As you shall learn, this is not the same as saying that these lesions are melanocytic. The next chapter, Mimics (ii), deals with some other common lesions.
Freckles (ephilides)
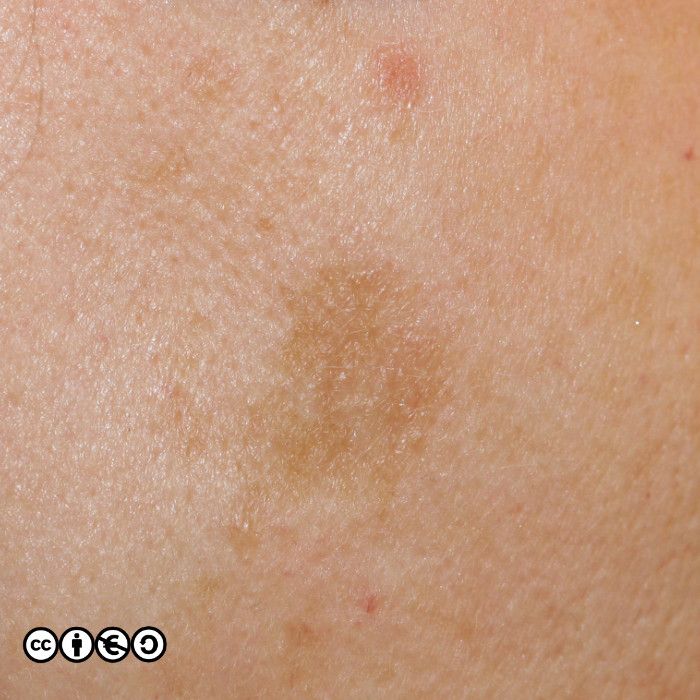
Freckles are flat (macular) focal areas of overproduction of melanin. The number of melanocytes is not increased (contrast with melanocytic nevi — see below — in which there are increased melanocyte numbers). Freckles are the result of sun exposure in those with sensitive skin.
Therefore you can expect to see freckles most commonly in red-haired or pale skinned persons who live in areas with high ambient sun exposure and have a history of sunburn. The extent of freckling therefore reflects both genetics and the environment.
It is therefore obvious that freckles are markers of — or a proxy for — skin cancer risk.
Freckles are most common on the face, shoulders and arms, but in some persons extend down the legs. Freckles darken in response to sunshine. They rarely enter into the differential diagnosis of skin cancer. (Image below copyright of Reto Caduff)
Seborrhoeic keratoses
Seborrhoeic keratoses (synonyms: basal cell papillomas, seborrhoeic warts) are benign keratinocyte tumours some of which are known to harbour somatic mutations.
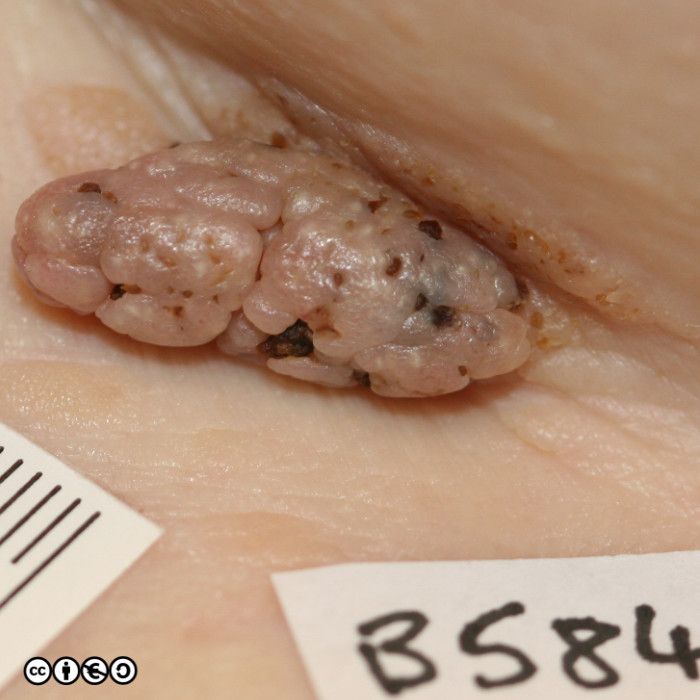
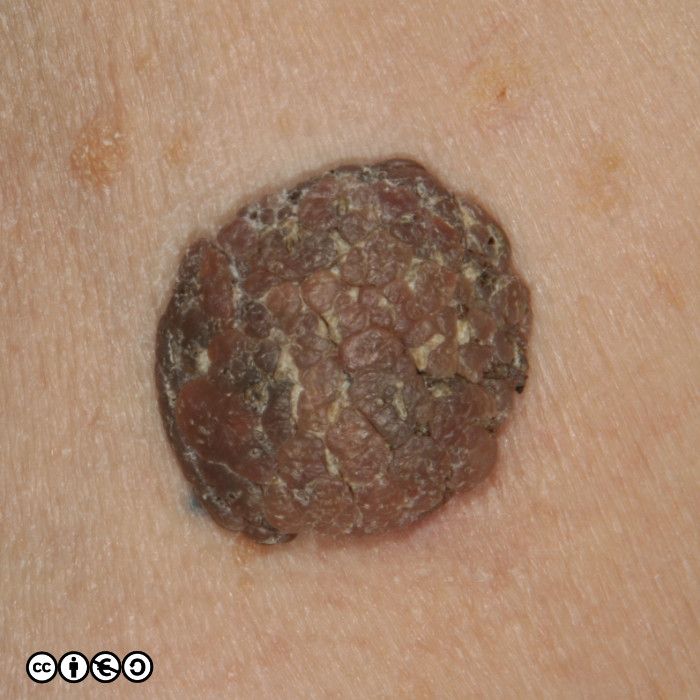
Clinically they vary from being almost flat to being raised by up to a centimetre. They have a stuck on appearance, and a warty (highly irregular) surface, and often appear ‘greasy’ (hence the name seborrhoeic, even though they have nothing to do with sebaceous glands). They are most common on the trunk but can occur on the face and limbs, but not on the palms or soles. They start to appear in the third and forth decades, and increase as the years go by. They are more common in Caucasians than in Asians or Africans
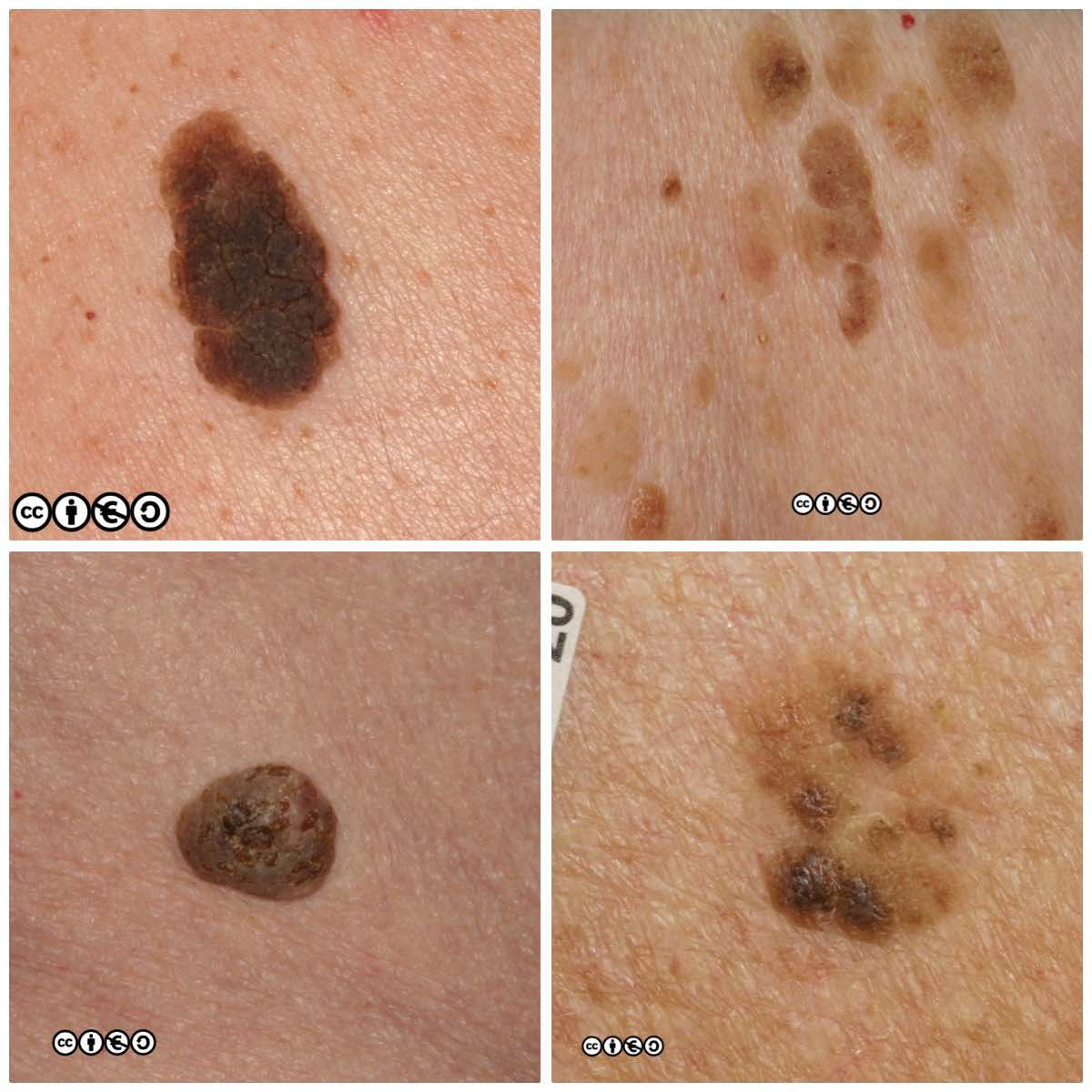
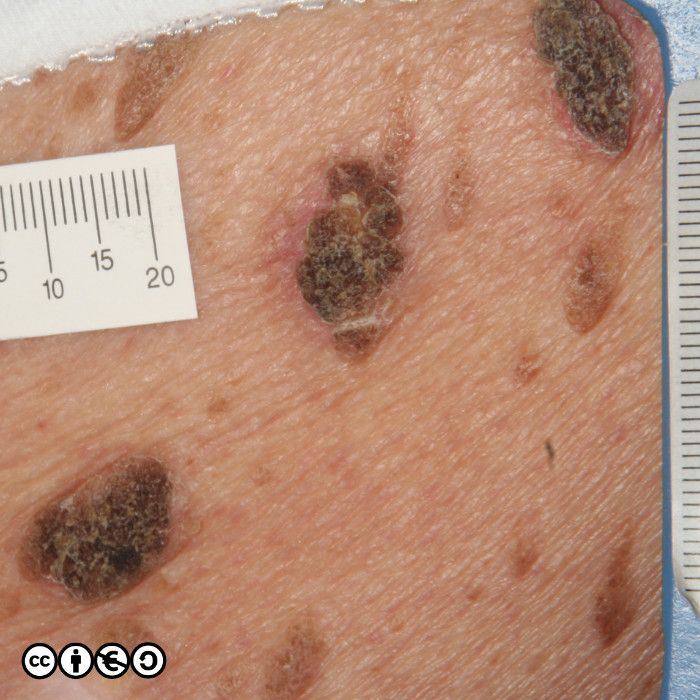
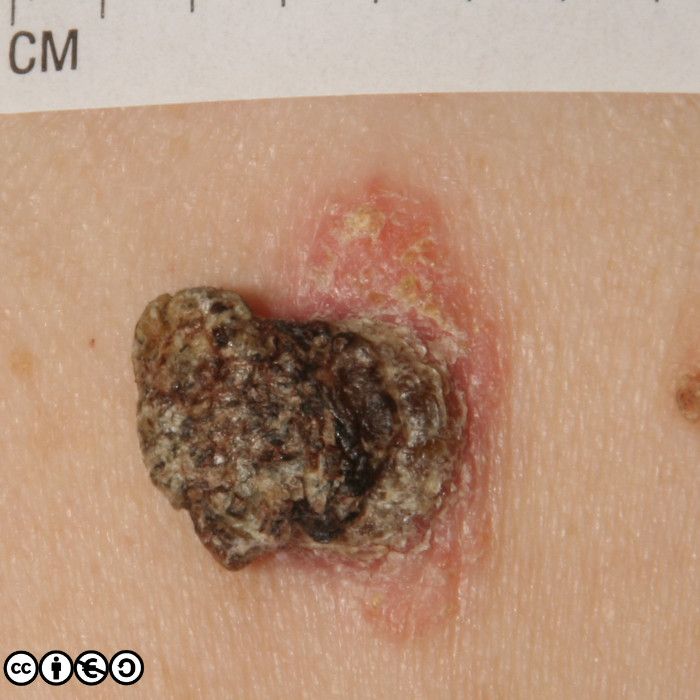
Some patients may have hundreds of seborrhoeic keratoses. They can virtually mimic any skin cancer including BCC and SCC, but they are frequently confused with melanoma. They may itch or bleed, are usually irregular in shape, with an irregular edge, and show variable pigmentation. Most putative melanomas referred from primary care to secondary care will turn out to be seborrhoeic keratoses.
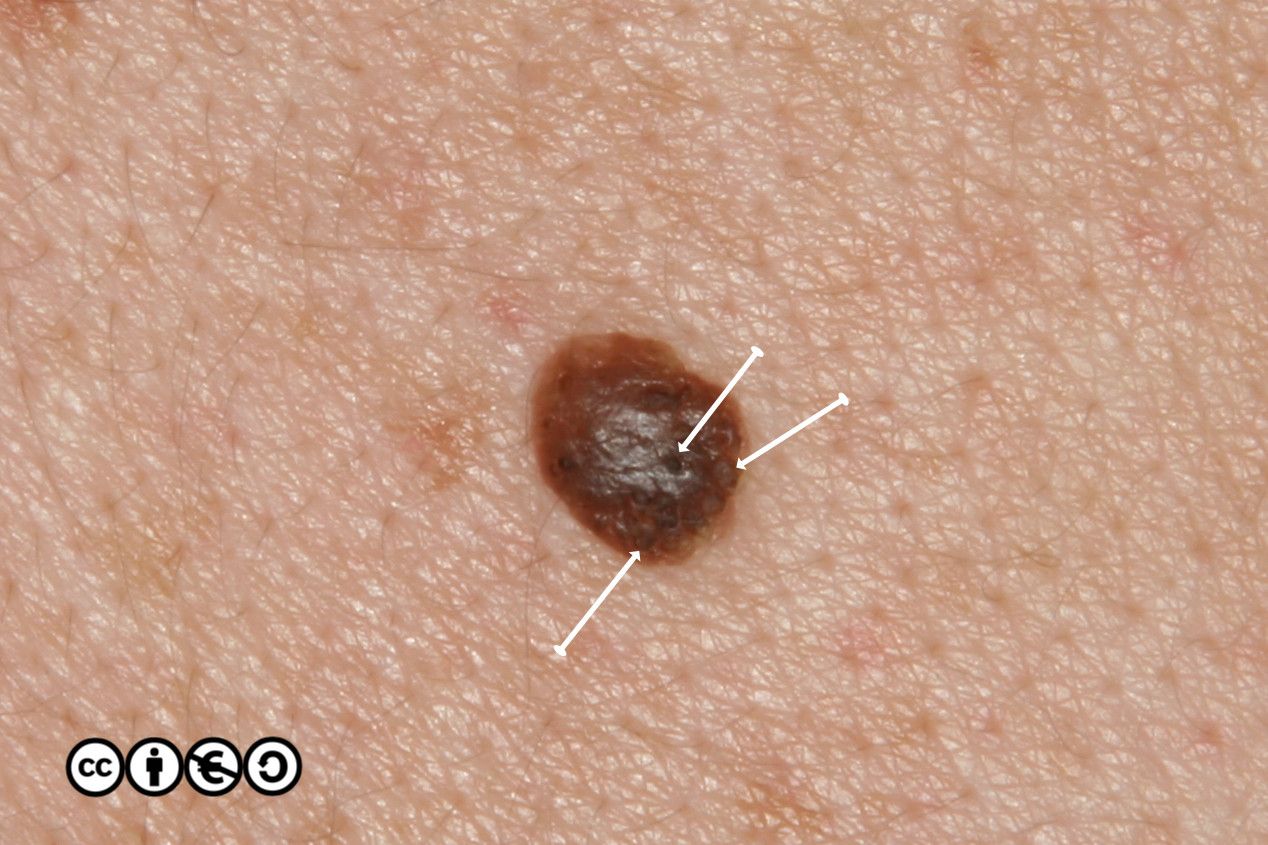
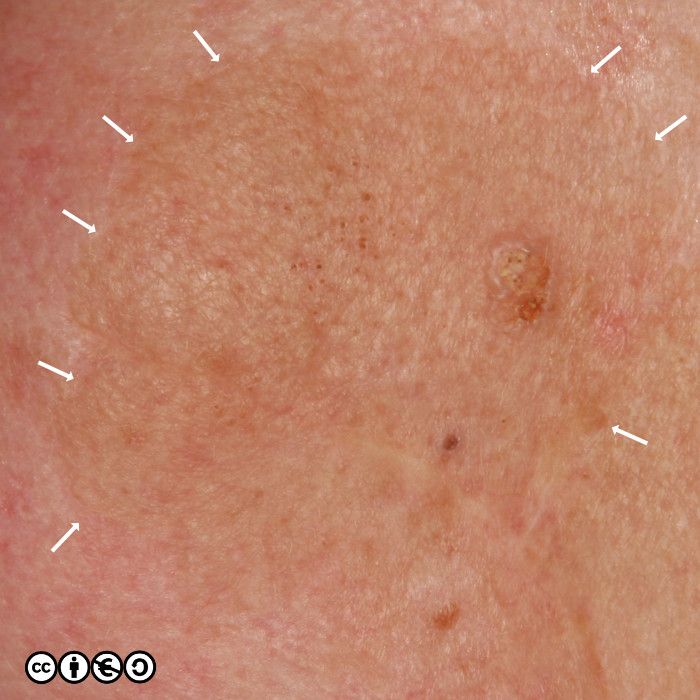
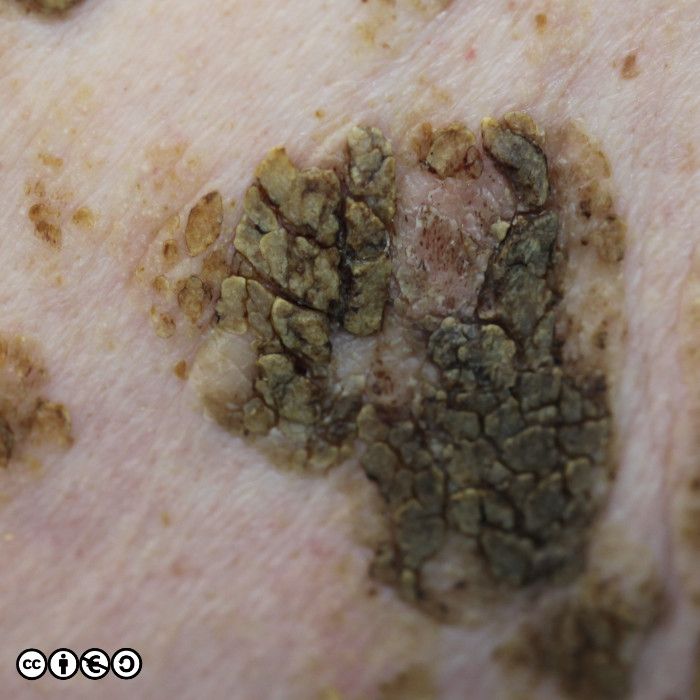
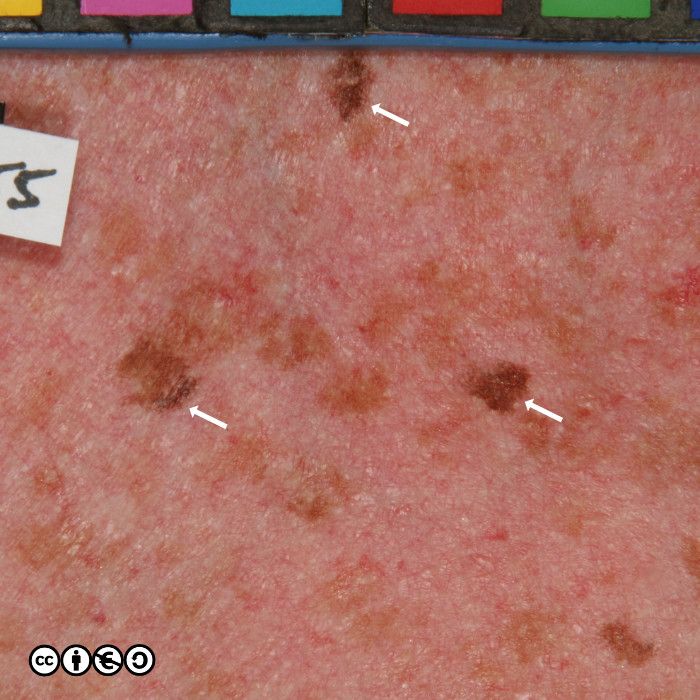
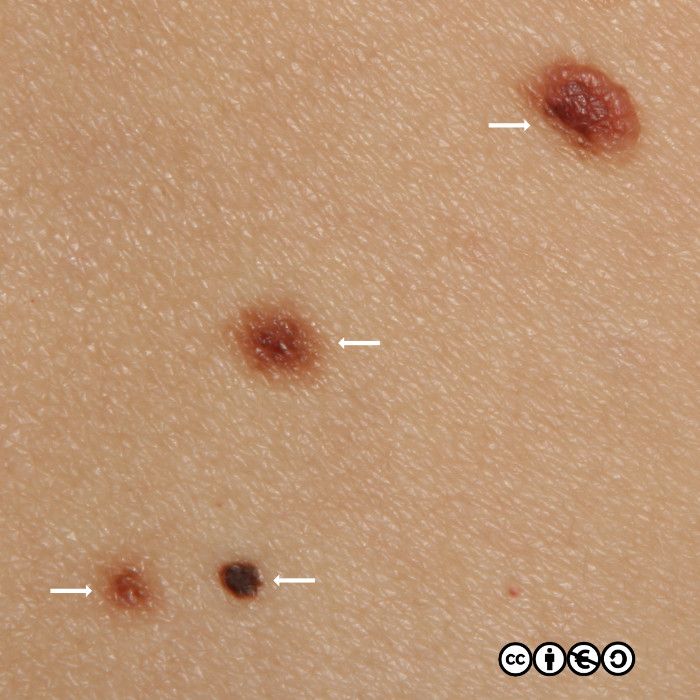
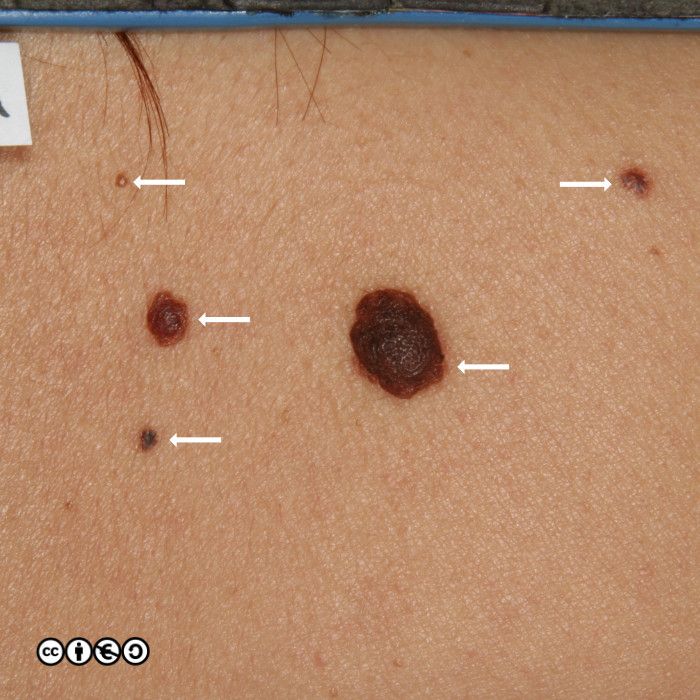
Some seborrhoeic keratoses contain many ‘comedo like‘ openings. If there are many of these — as are shown with white arrows in the image below — they suggest seborrhoeic keratosis as the diagnosis. (I have only pointed to some of the comedo like openings.)
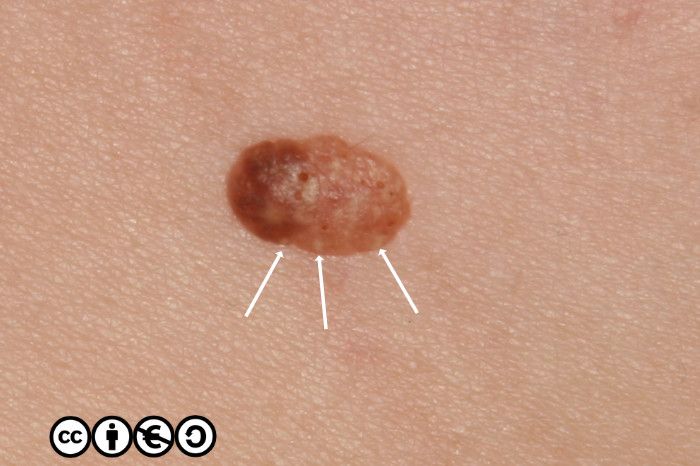
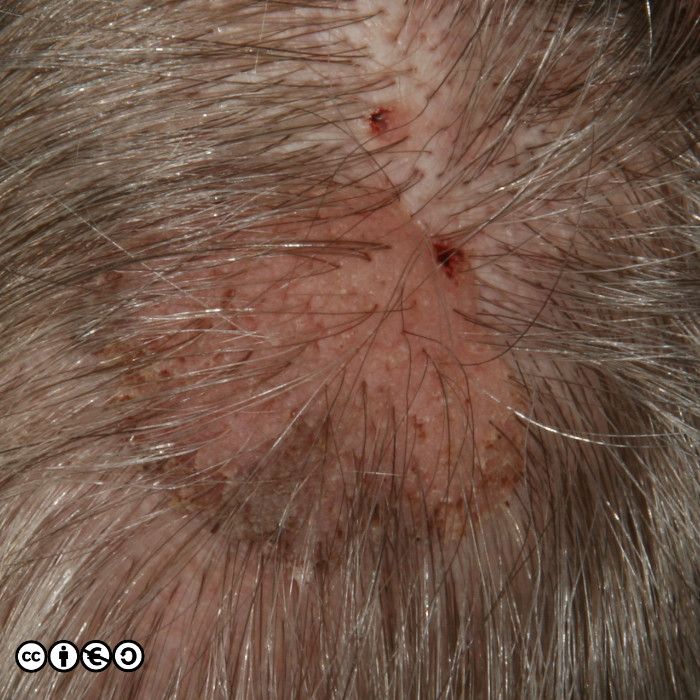
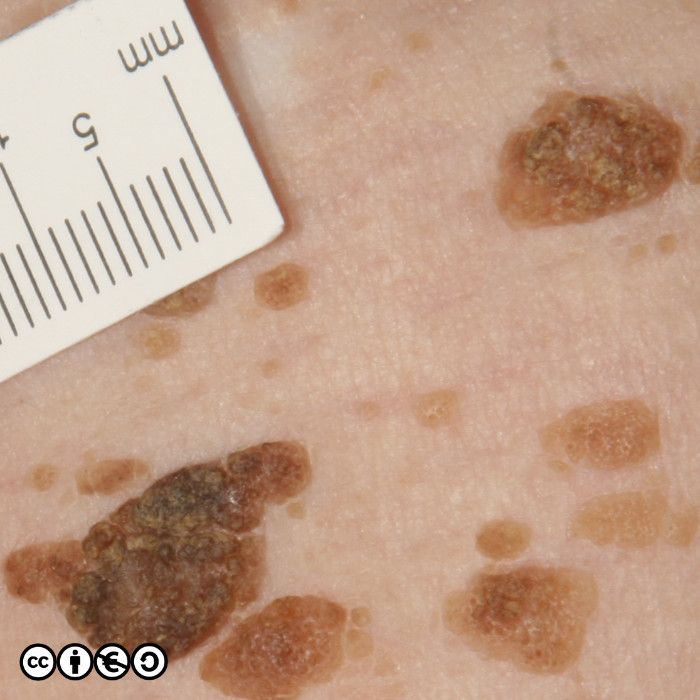
As well as the these comedo like openings, you may see white milia like (pseudocyst) structures. In the image below, some of these are arrowed — there are more. In this image you can also see some comedo like openings, too.
The milia like and comedo like structures are not present in all seborrhoeic keratoses, but they can be useful in distinguishing some seborrhoeic keratoses from melanomas (they are very uncommon in melanomas).
Carousel of 11 Seborrhoeic Keratose images
Below are 11 images of seborrhoeic keratoses. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
Solar Lentigines (single: lentigo, plural: lentigines)
A true lentigo means a linear proliferation of melanocytes along the basement membrane. Unfortunately the term lentigo is used for lots of lesions that are not true lentigines. Do not get hung up on when a lesion is a true lentigo or not.
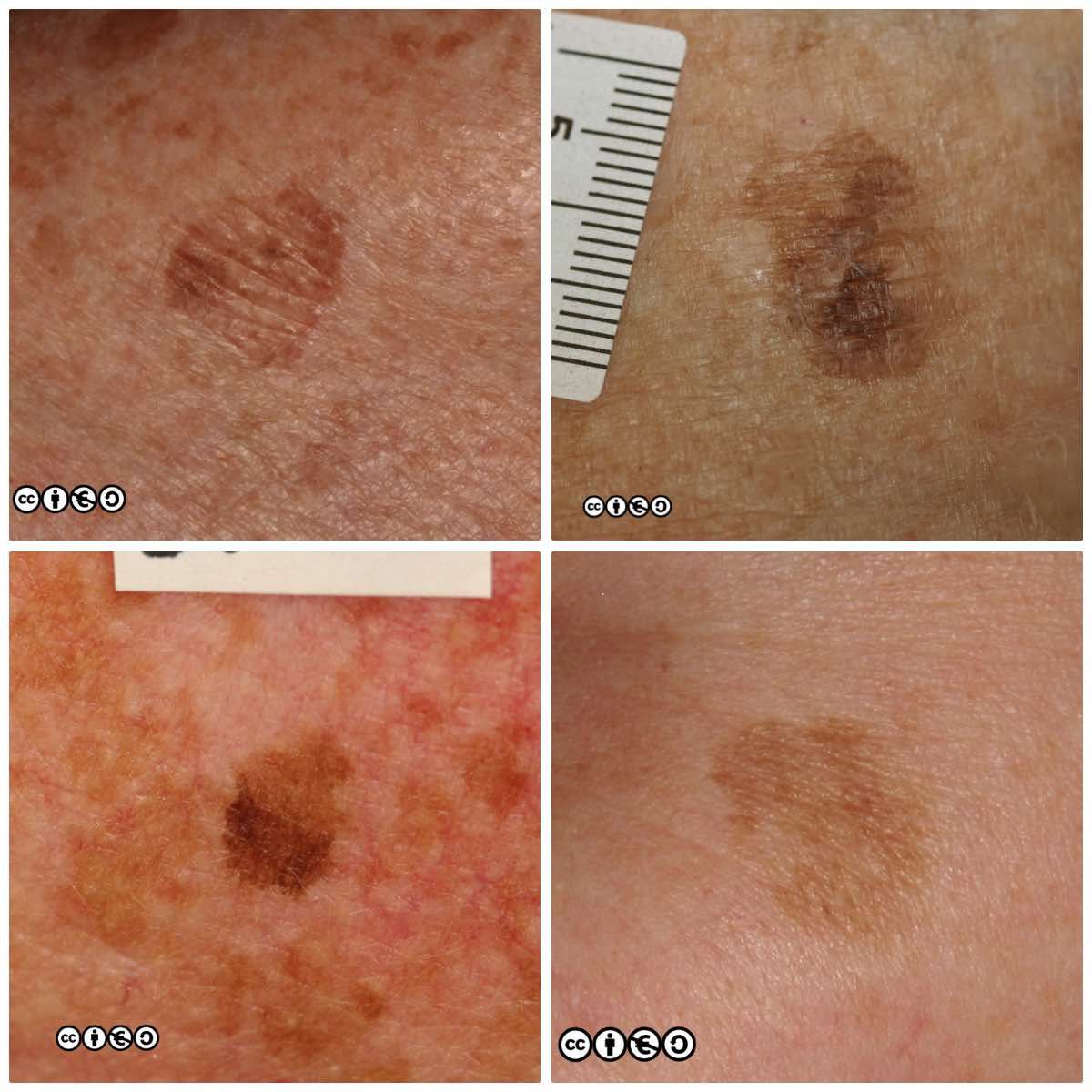
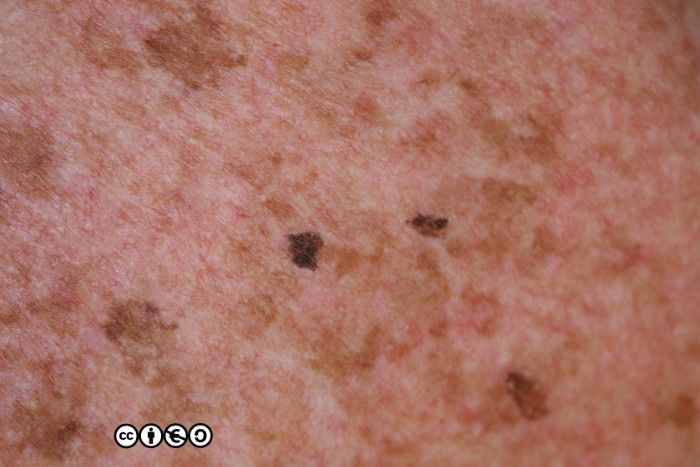
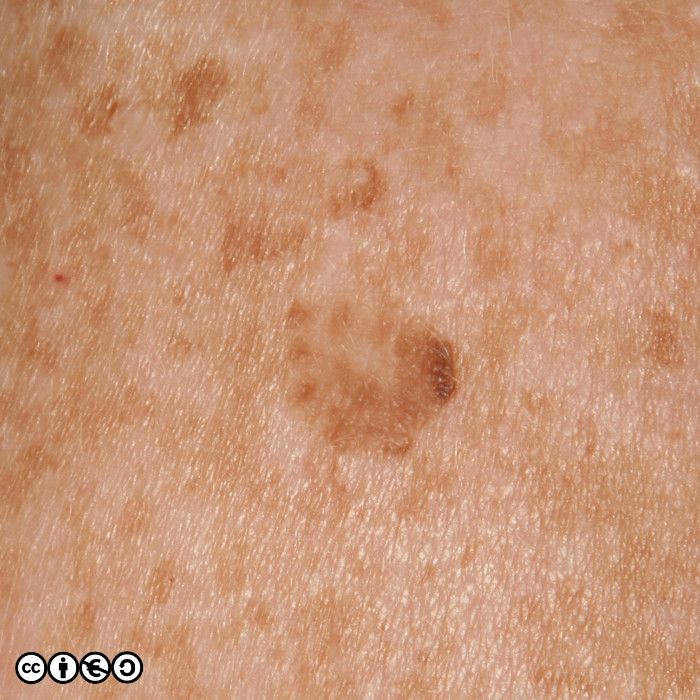
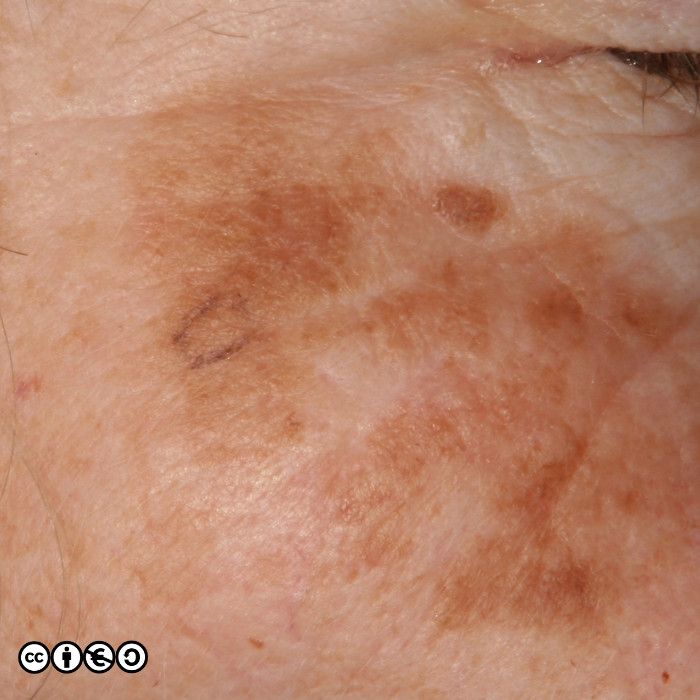
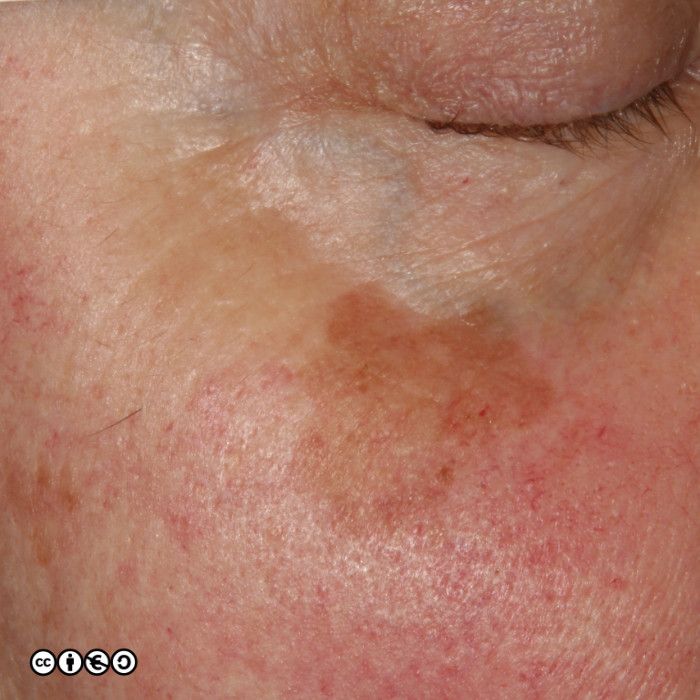
Solar lentigines (‘liver spots’, to many patients) are flat or almost flat brown marks most common on the backs of the hands, forearms and the face. They reflect previous sun exposure and the surrounding skin may show other features of sun damage. Solar lentigines are essentially flattish seborrhoeic keratoses on histopathological examination. The number of melanocytes is not increased, and the pigment is melanin. So, although we can say they are pigmented lesions, they are not primarily melanocytic lesions (i.e. there is no proliferation of melanocytes).
Their medical significance is that if they are flat and without any warty appearance they can be easily confused with lentigo maligna or lentigo maligna melanoma, or other benign melanocyte proliferations that are common on sun exposed skin. They are almost ubiquitous after middle age in sun sensitive patients. If an index lesion looks like lots of others on the patient’s own skin it is very unlikely to be a melanoma. If there is doubt, do not biopsy, but refer to a dermatologist.
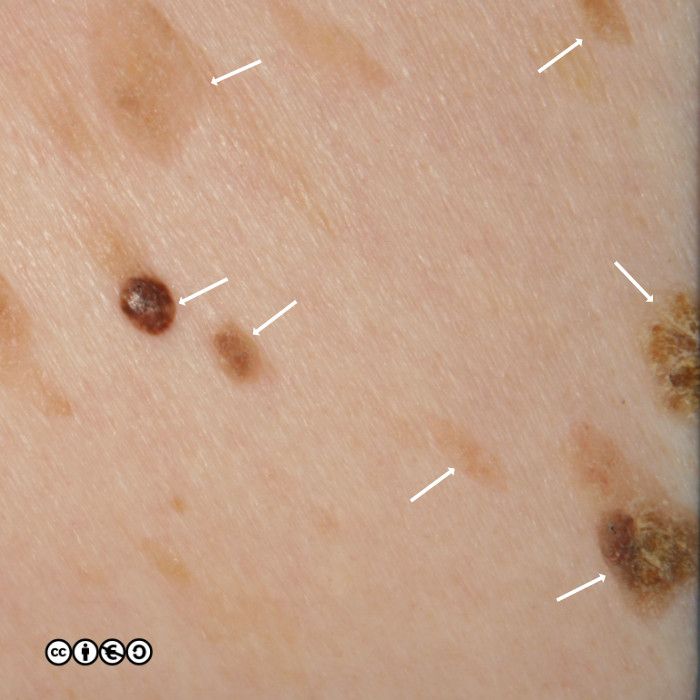
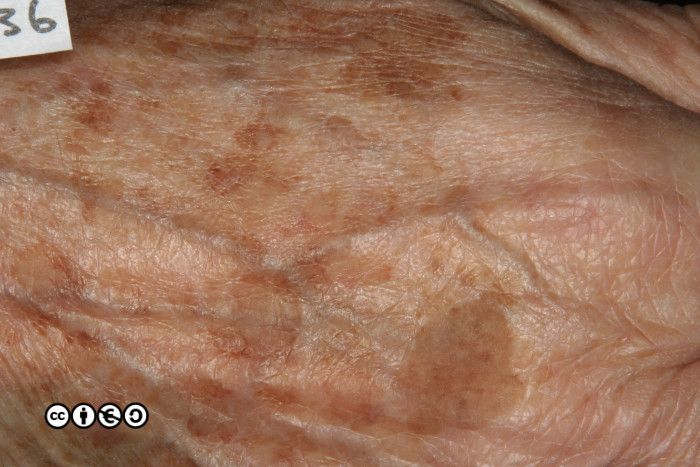
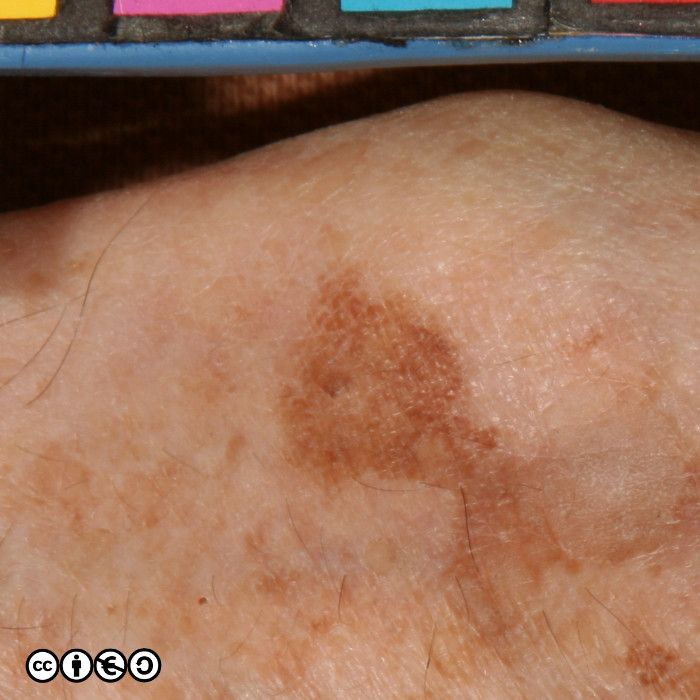
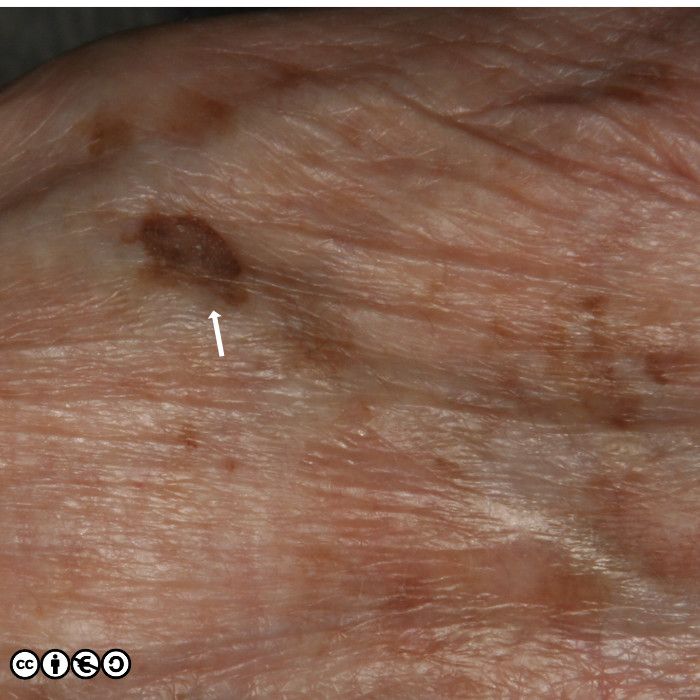
The relation with seborrhoeic keratoses is clear in the image of multiple lesions on the back of this person’s hand. Many are clinically macular, but some are raised and we could debate whether these are solar lentigines or early seborrhoeic keratoses.
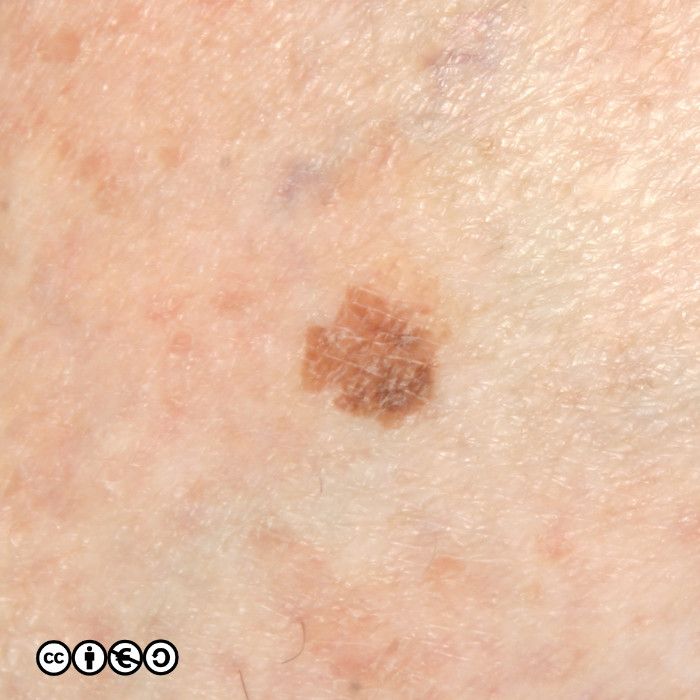
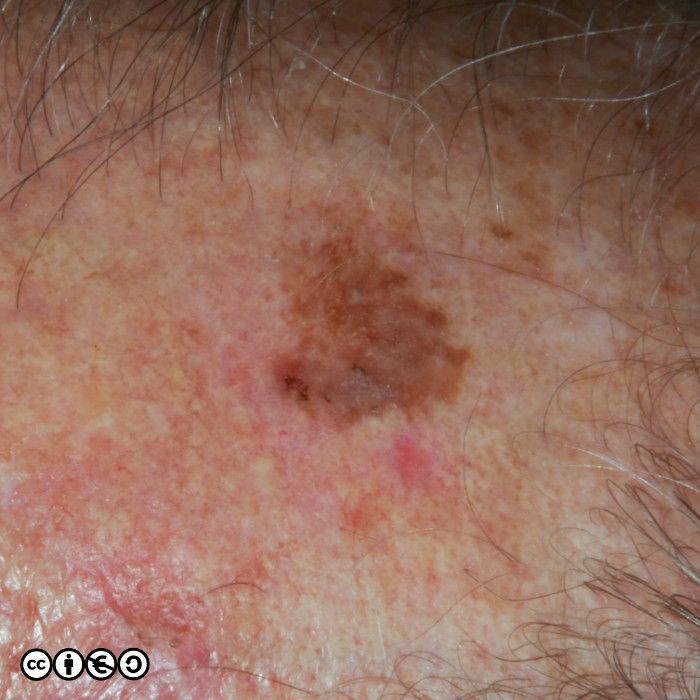
The image below shows how some solar lentigines can be very dark (the two lesions stand out against the almost complete coverage of tan coloured solar lentigines in this image). The clinical differential is versus a melanoma.
Carousel of 10 Solar lentigines
Below are 10 images of solar lentigines. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
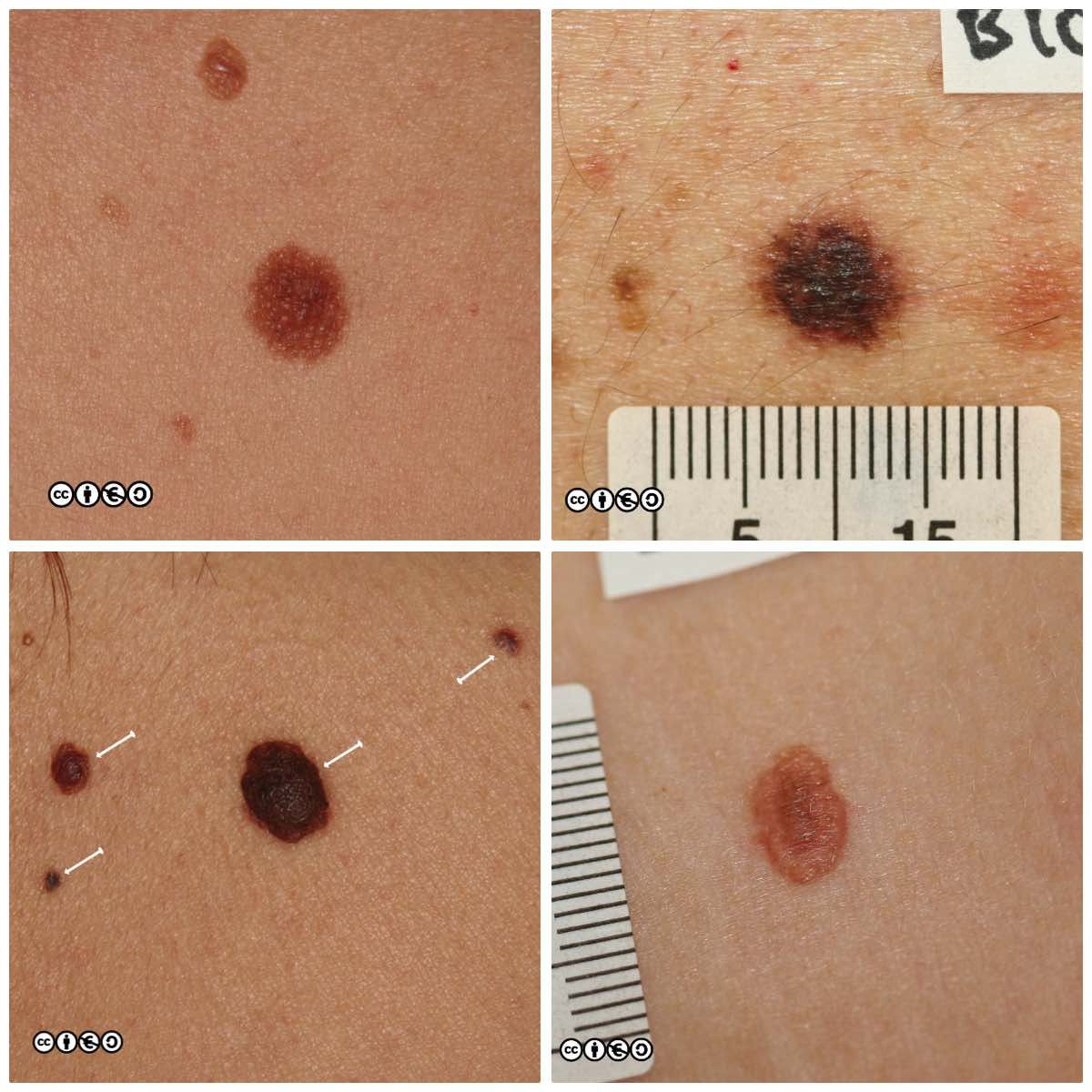
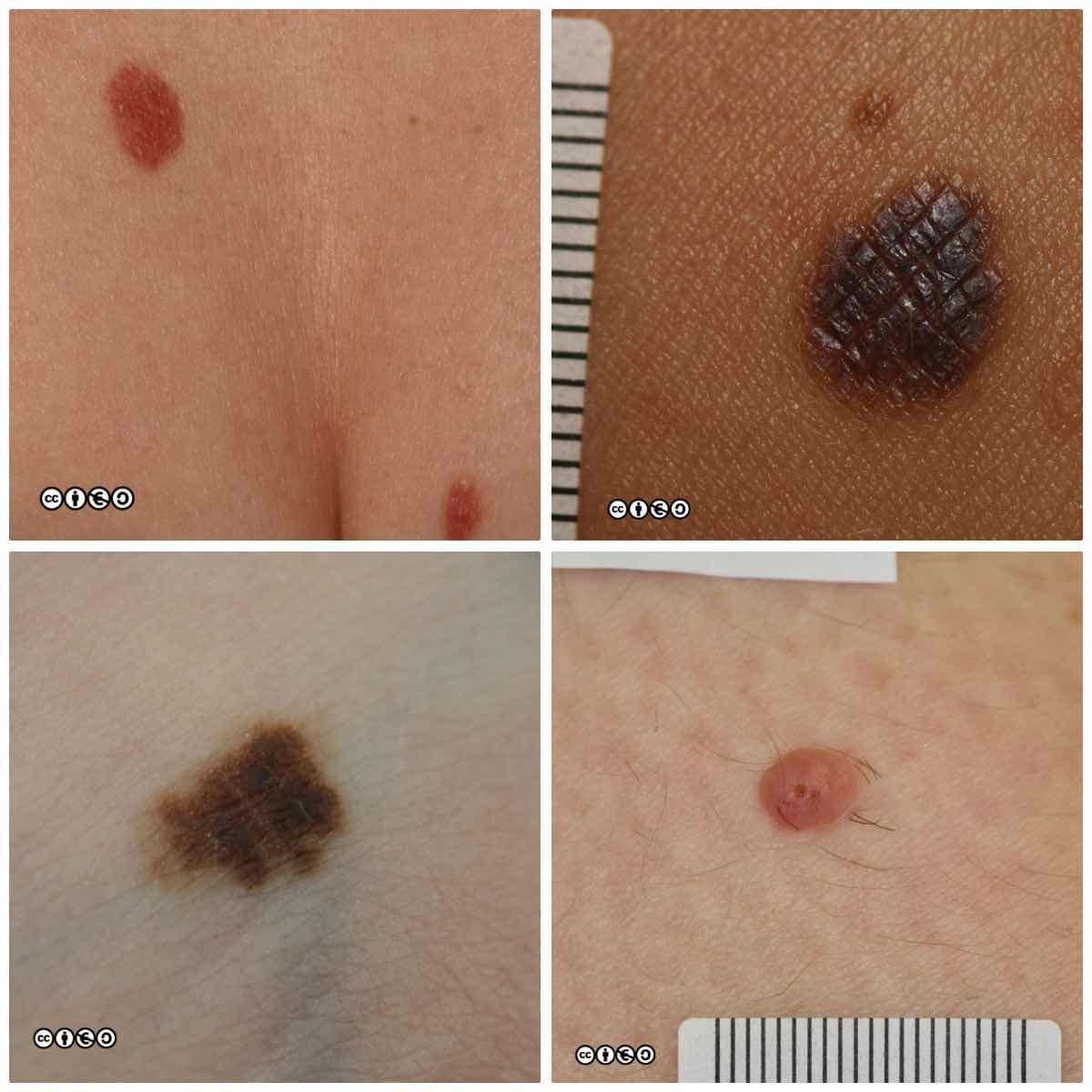
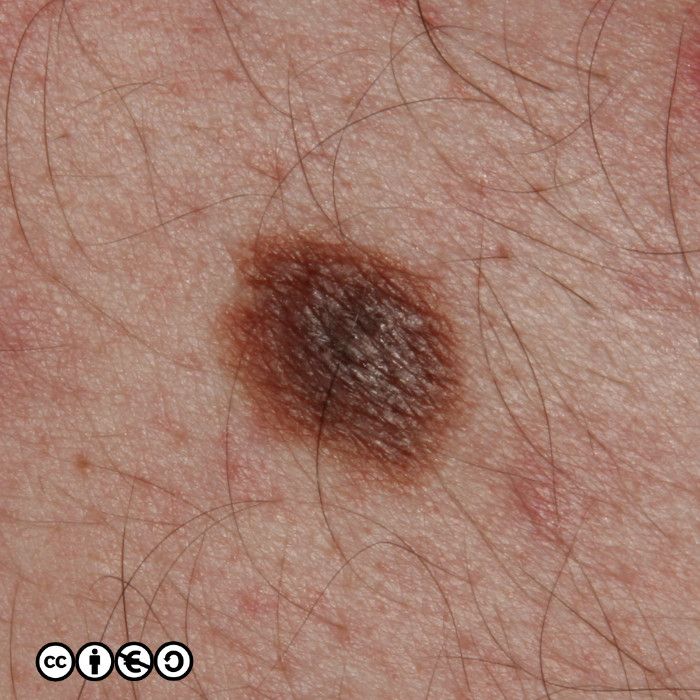
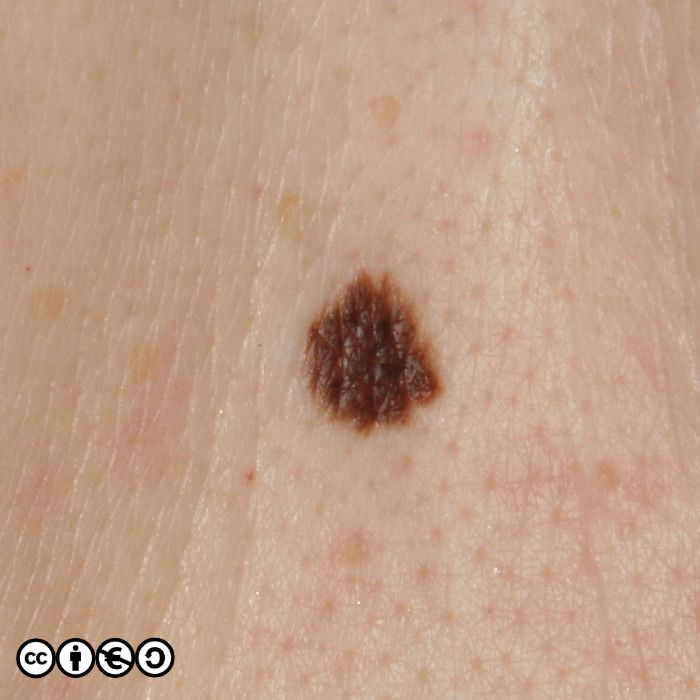
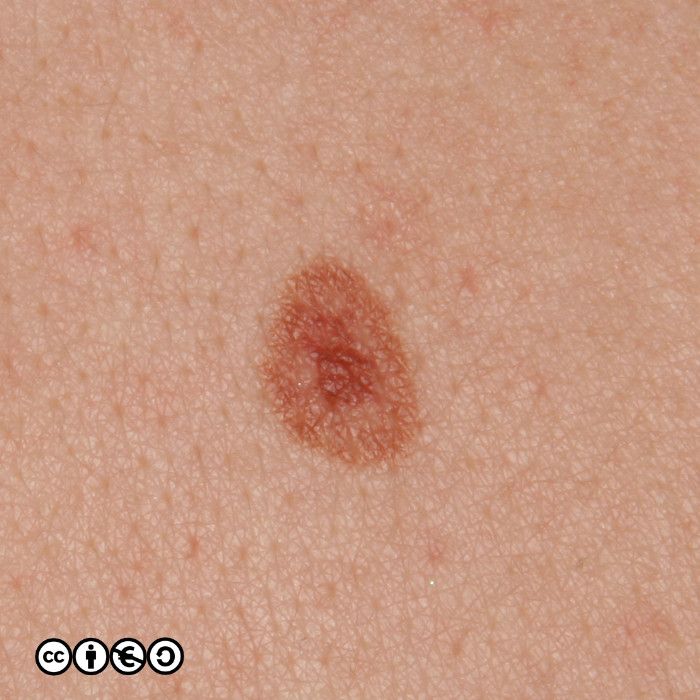
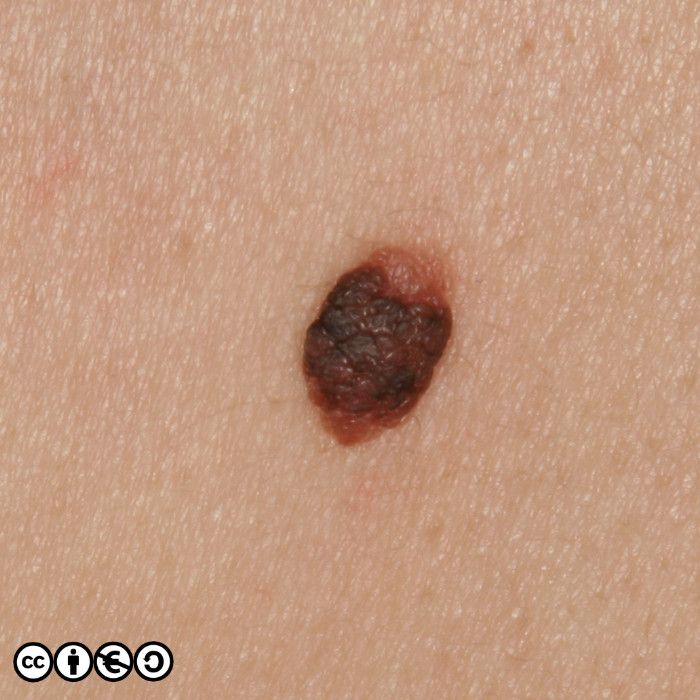
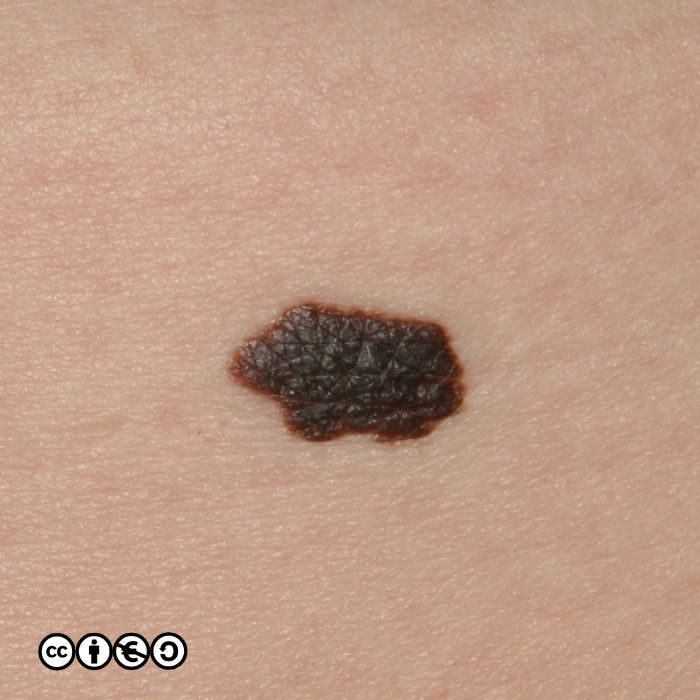
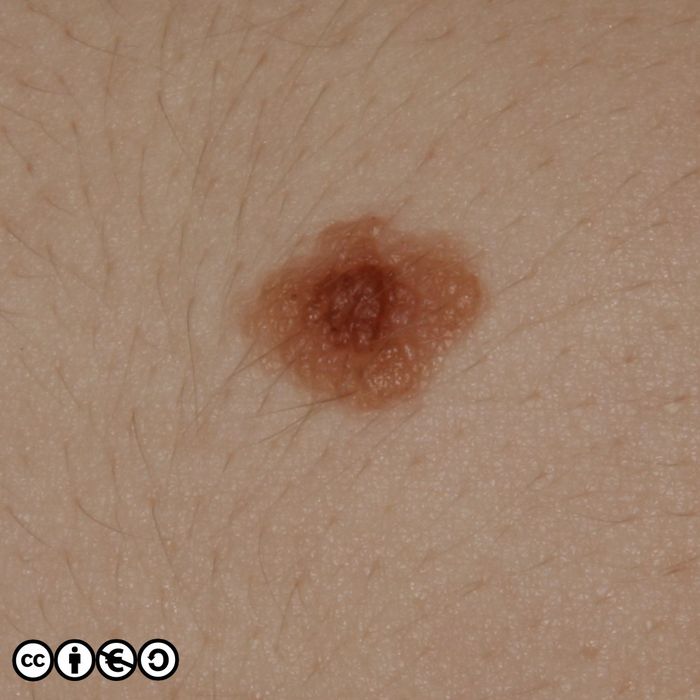
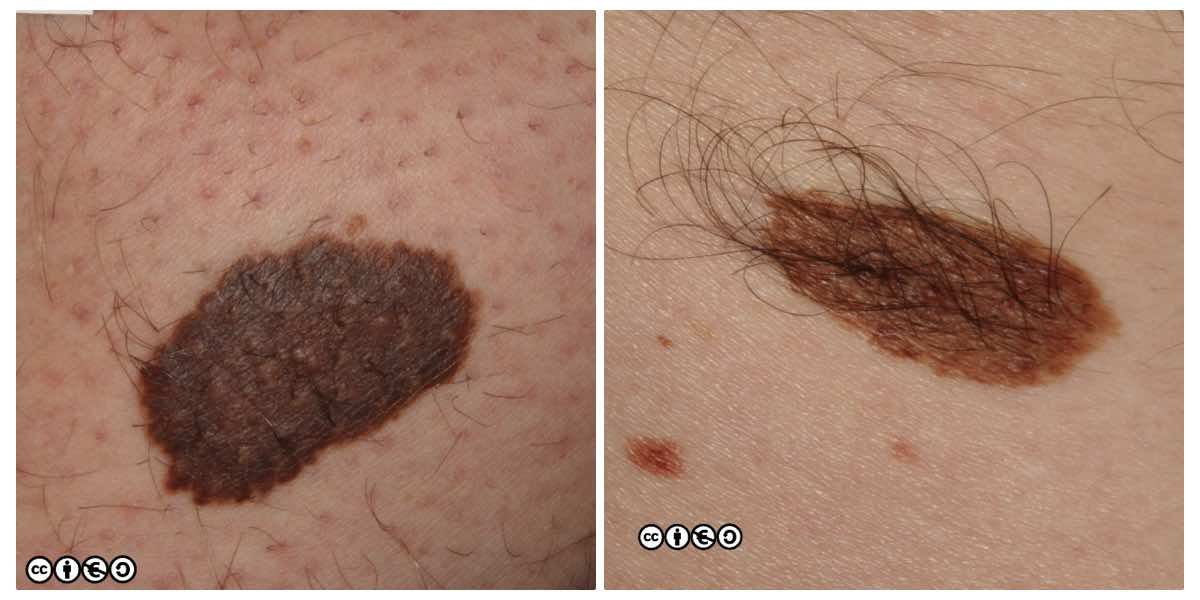
Melanocytic nevi (‘moles’)
Melanocytic nevi are focal collections of melanocytes clustered in a nest (or ball like clump) that may or may not produce pigment. Melanocytic nevi are clonal and harbour mutations in growth controlling pathways. They are therefore benign tumours, but benign tumours that contain some of the mutations that are found in many melanomas.
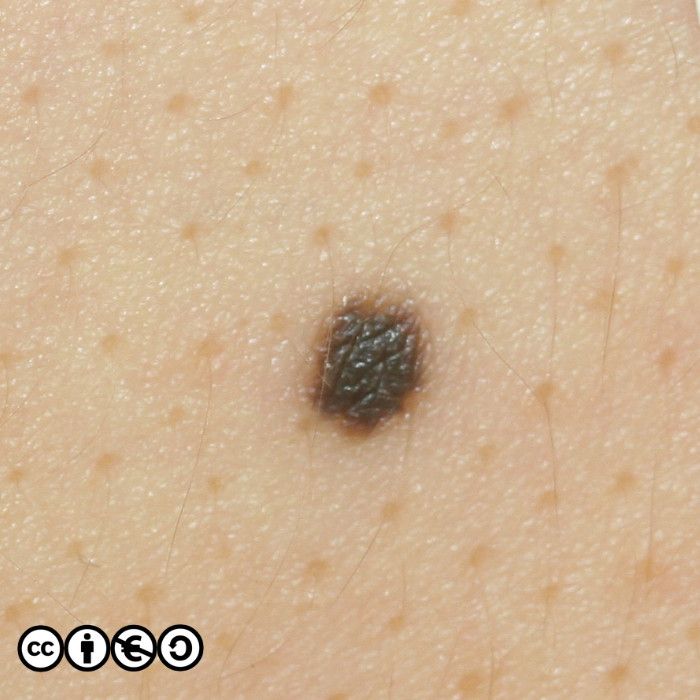
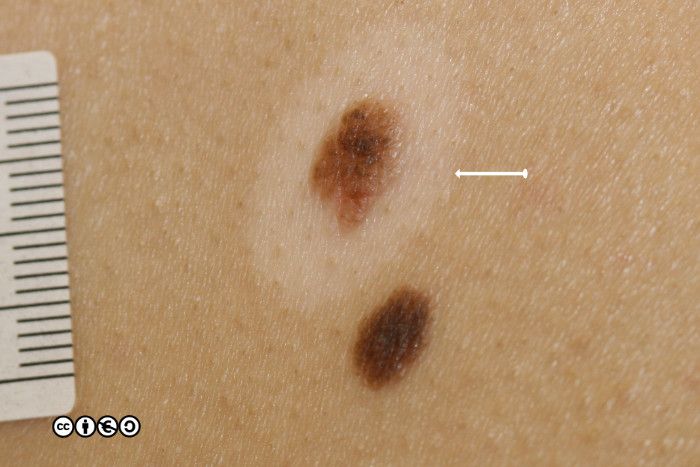
Melanocytic nevi are not static throughout life. They typically start to appear in childhood, reaching a maximum in the third and fourth decades. In early life they are often flat and dark, before becoming raised whilst still being pigmented, before losing their pigment but remaining raised. They can take on a myriad of morphologies and some resemble seborrhoeic keratoses with a very warty appearance. Melanocytic nevi are more common in those with a history of greater sun exposure in childhood, and melanocytic number reflects genetic influences too.
The medical significance of melanocytic nevi is as follows:
- They are benign melanocytic tumours, wheres melanomas are malignant melanocytic tumours.
- Most melanocytic nevi harbour mutations of genes know to be implicated in melanoma (e.g. BRAF). However, the rate of progression of a benign melanocytic nevus to melanoma is extremely low (~1/200,000 per year), so clearly other genetic changes are required to produce the malignant phenotype.
- Melanocytic nevi and melanomas may look very similar. Often distinguishing between them is hard clinically and, in a minority of instances, excision biopsy will be required.
- Some nevi do progress to melanoma although the percentage is extremely low. Conversely, a significant fraction of melanomas are derived from melanocytic nevi (figures of up to 30-50% are quoted in the literature).
- Melanomas may (apparently) arise de novo without there been a preexisting nevus (or at least not a visible one).
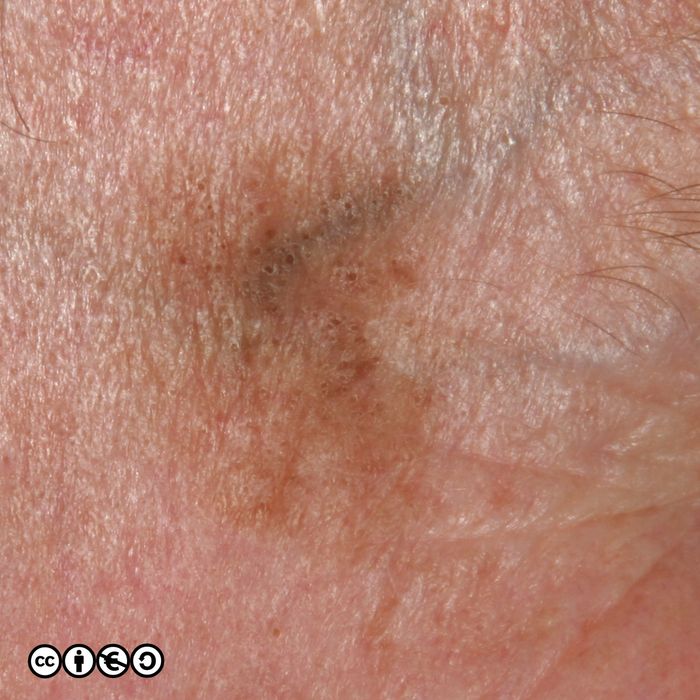
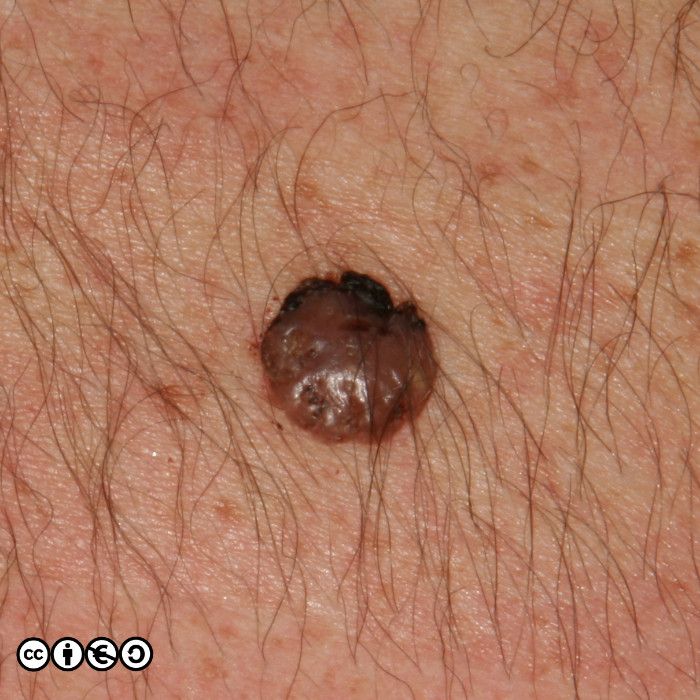
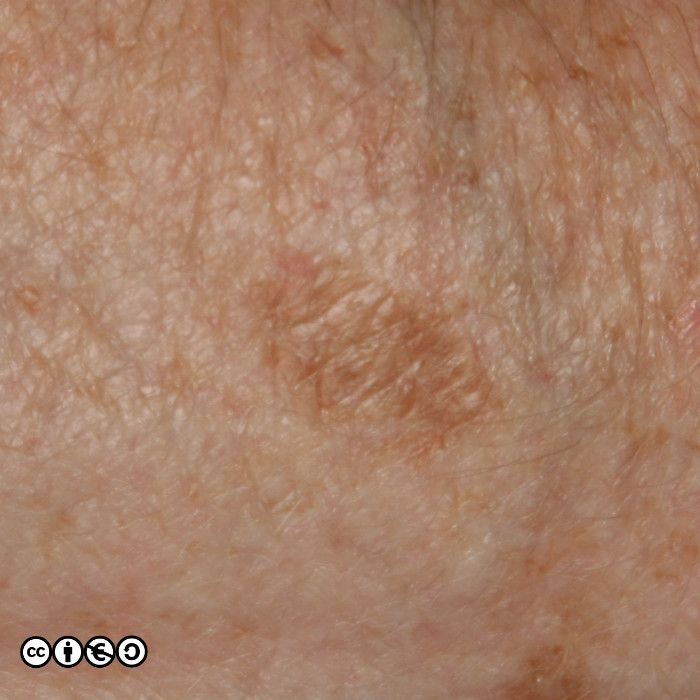
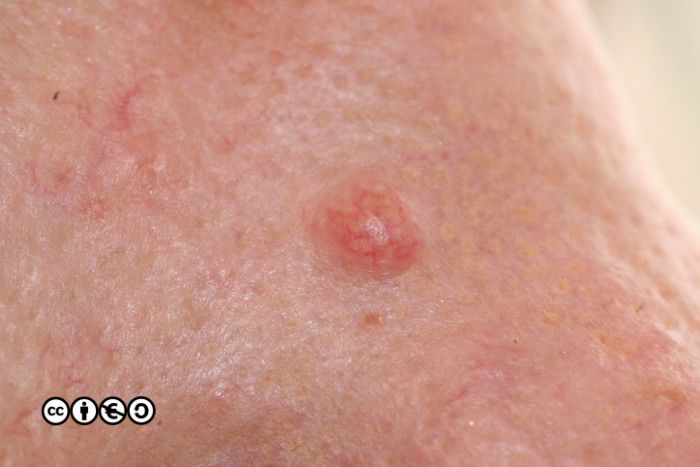
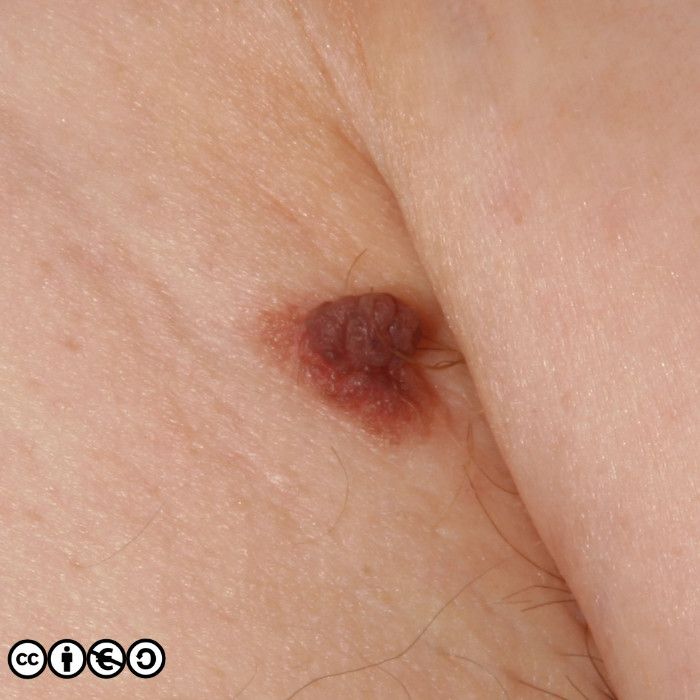
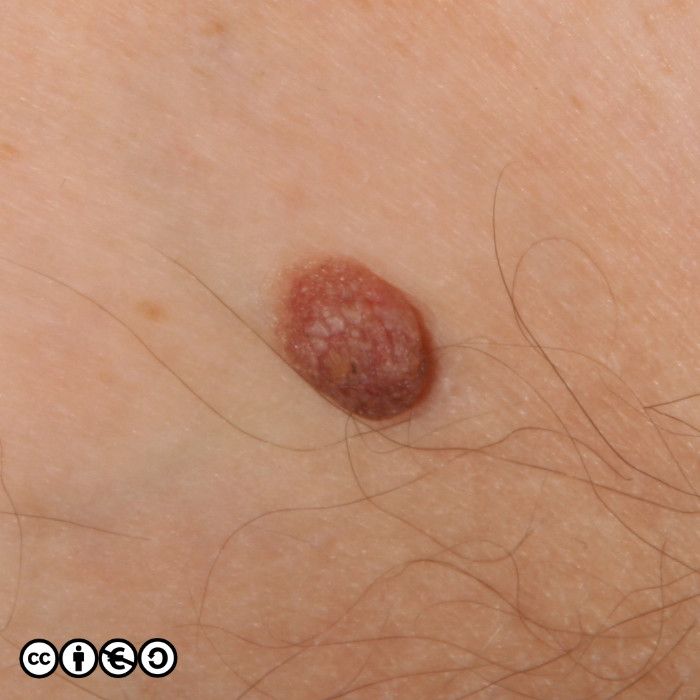
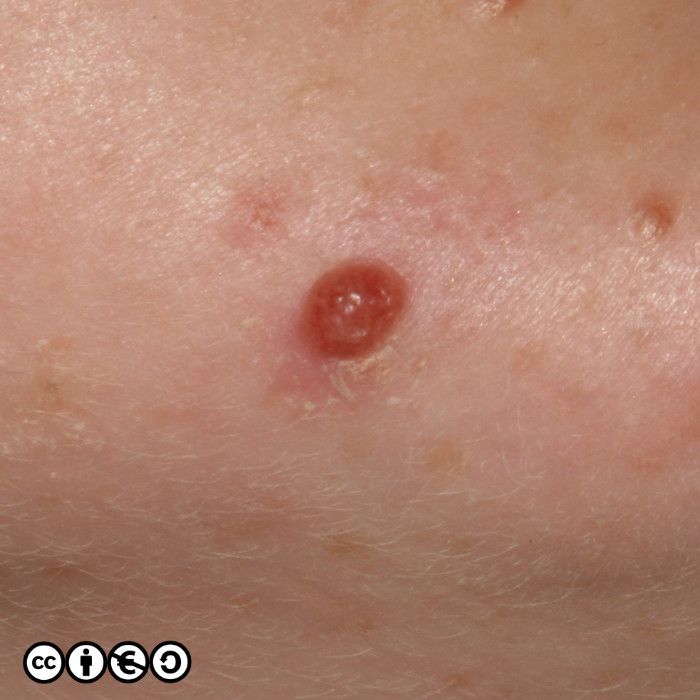
There are lots of descriptive names which whilst helpful to specialists, are not core knowledge for students, and I suggest you do not bother trying learn them all. It is important however that you realise how varied the appearance of benign melanocytic nevi are. For instance the image below is of a type of melanocytic nevus, called a dermal nevus, in which there is very little pigment. Not all melanocytic nevi are pigmented.
Carousel of 15 images of melanocytic nevi
Below are 15 images of melanocytic nevi. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
Congenital melanocytic nevi
Some pigmented nevi are present at birth or appear soon after birth and are known as congenital melanocytic nevi. These occur in a few percent of the population and are harmless unless they are very large (>10cm) when they may (rarely) undergo malignant change.
Many of these nevi do not contain just melanocyte proliferation but other tissue elements (e.g. hair follicle, sweat glands, neural tissues). Although traditionally said to be hamartomas, some or all of such congenital nevi might be viewed as the result of somatic mutations affecting cellular growth pathways.
Atypical or dysplastic nevi?
The term dysplastic nevus can refer to either a clinical or histopathological appearance, but their is little overlap between these usages. The term was meant to embrace a melanocytic nevus that seems unusual in appearance and is reminiscent of a superficial spreading melanoma. The implication being that this type of atypical or dysplastic nevus is in danger of progressing to melanoma.
Nobody can agree on what these terms mean in a clinically useful way.
In practice a large proportion of the population seem to have melanocytic nevi that meet the criteria for dysplastic nevi and there is little consistency between dermatologists. In practice, if you think a melanocytic nevi is suspicious of melanoma, say that, and act on it. Do not bother trying to delve deeper into this topic, as it is resembles a branch of politics.
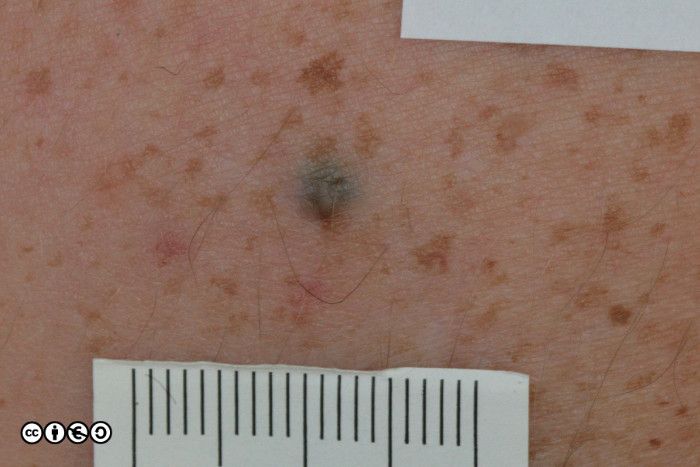
Blue nevi
Melanin deep in the dermis appears blue due to light scattering. Clusters of melanocytes that are deep in the dermis appear blue. If you want to understand light scattering, check out the video below at the bottom of this section, but feel free to skip.
They often appear in childhood, and are more common in some Asian populations. However a new onset blue nevus in middle age or older should be looked upon with suspicion: could this be a nodular melanoma? Physical signs alone will not always allow a clear distinction, and you may need to biopsy the lesion.
Halo nevi
These are melanocytic nevi that appear to be under immune attack from the host with destruction of melanocytes. They are easy to diagnose.
Halo nevi are of no clinical significance except that halo nevi may appear in a patient with a melanoma elsewhere — examine the whole skin of such adult patients. They are common in childhood and harmless. They do not require excision unless the nevus itself looks like a melanoma.
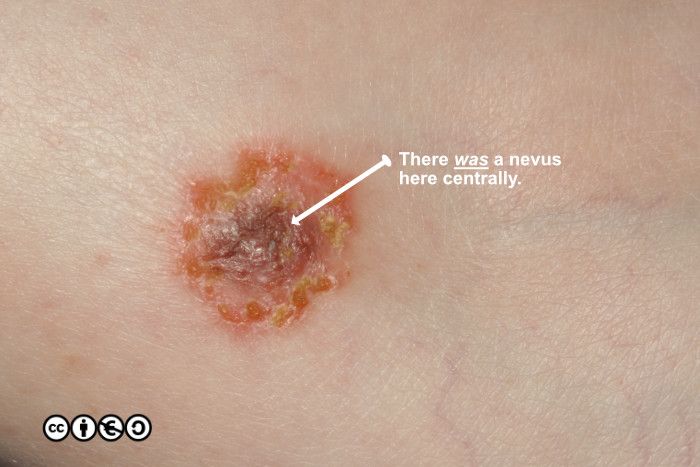
Meyerson’s nevus: Some melanocytic nevi become surrounded by what appears to be a patch of eczema although there is not a halo present (known as a Meyerson’s nevus). These again seem to represent some form of host response to a nevus and are of no great medical consequence. (image below).
Melanotic macules of the lips
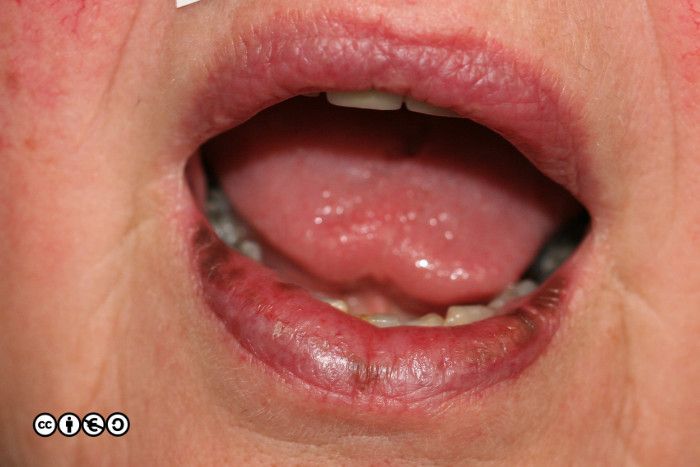
These are also known as mucosal melanotic macules. They are macular areas of increased pigmentation seen on the lips (and the genitalia).
In the image above there are multiple pigmented macules on the lower mucosal lip. Such mucosal melanotic macules are usually multiple. Solitary lesions can be confused with melanomas or venous lakes (discussed in the next chapter). If in doubt, refer to an expert.
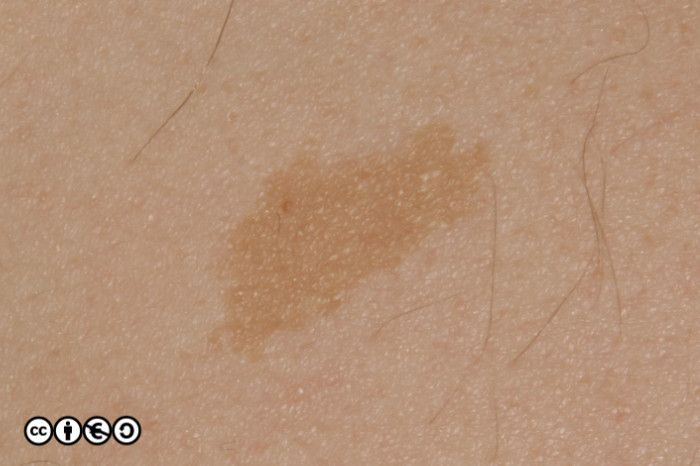
Café au lait macules
These are light brown macules measuring from one centimetre upwards to 10cm or more.
They are present in up to 10% of the normal European population, and are present from early childhood. If more than five are present consider neurofibromatosis and check for axillary freckling and neurofibromas.
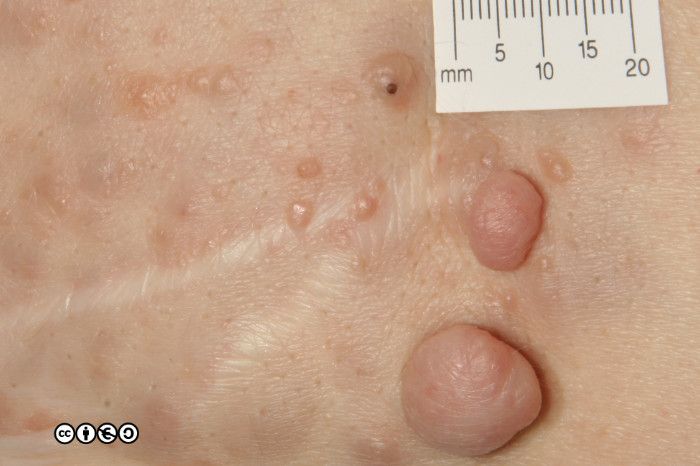
A patient with the multiple neurofibromas of neurofibromatosis is shown below.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.