The previous two chapters dealt with BCC and SCC — the two commonest types of skin cancer, both of which are keratinocyte derived. Basal cell carcinomas have no clinically identifiable precursors. By contrast, there are two lesions — actinic keratoses and intraepithelial carcinomas — that are keratinocyte precursors of SCC. Both actinic keratoses and intraepithelial carcinomas can therefore be considered premalignant — that is, some lesions, may undergo transformation into squamous cell carcinomas (but most do not).
In this chapter I also discuss another lesion — the keratoacanthoma (KA) — a lesion that is neither premalignant nor malignant, but which has a very curious pattern of clinical behaviour, and which is easily confused with SCC (and premalignant lesions).
This chapter in one minute
Actinic keratoses
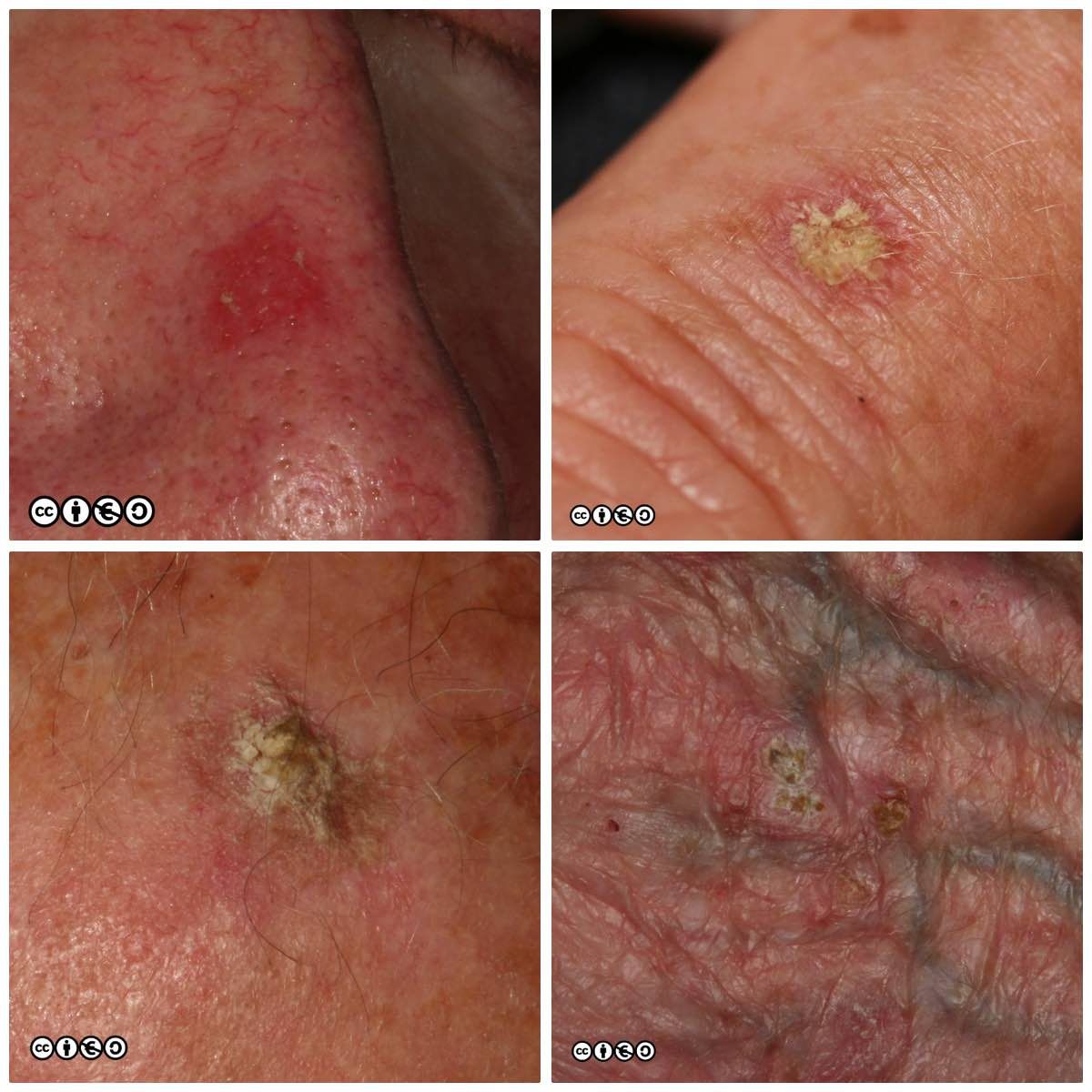
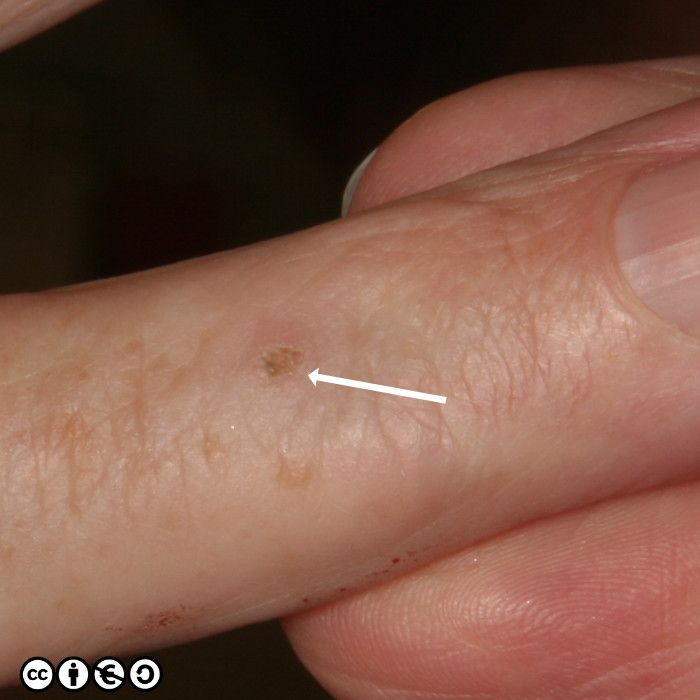
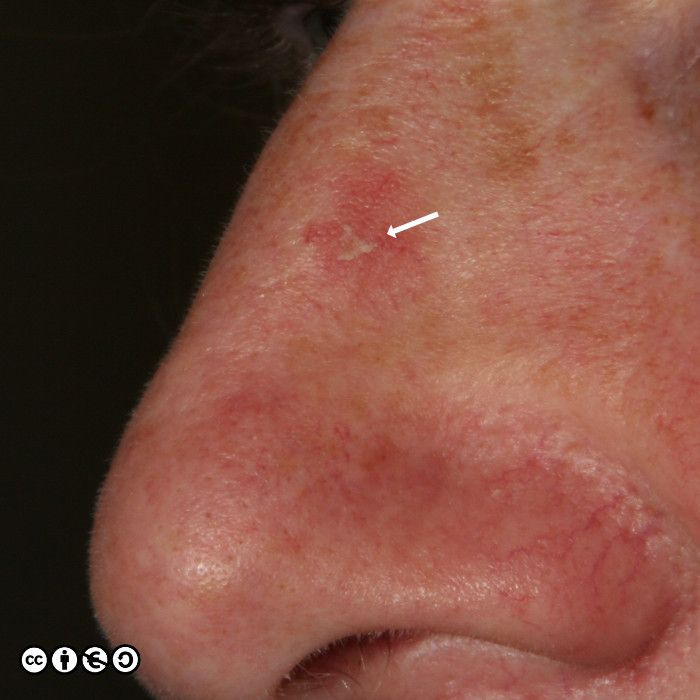
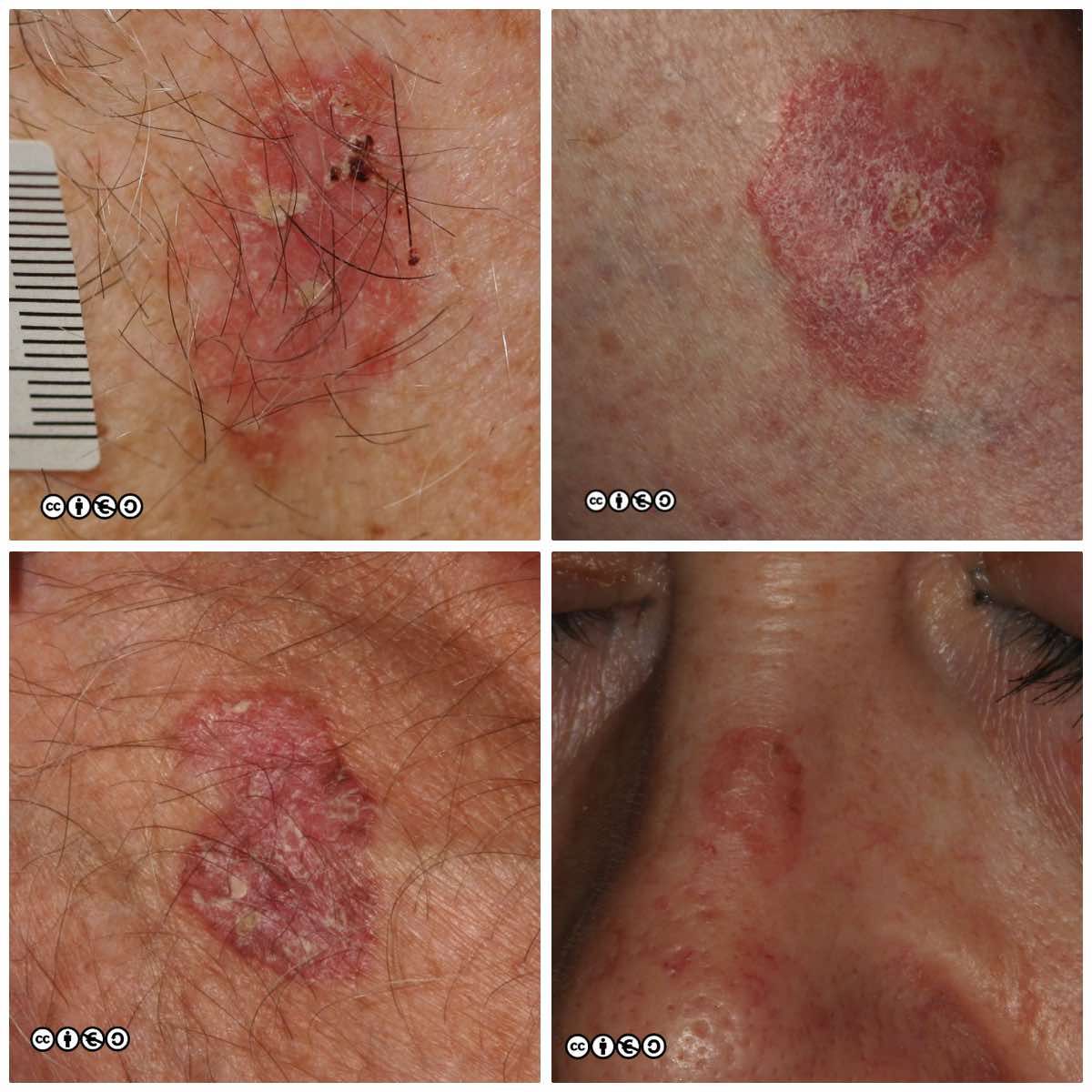
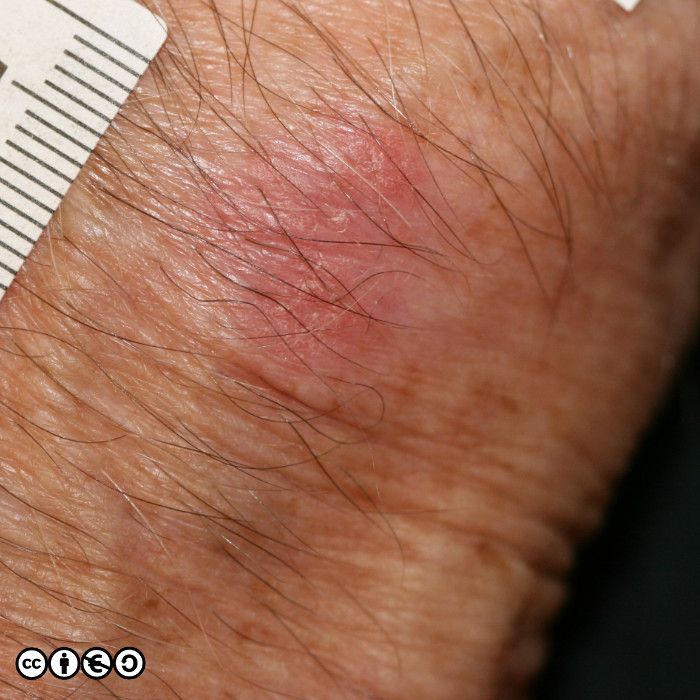
Actinic keratoses (less commonly termed solar keratoses) are focal areas of dysplasia characterised by erythema and scale that may feel rough when the fingers are rubbed over them. They are a marker of UVR exposure occurring at those sites that have received the most cumulative sun exposure, such as the scalps of bald-headed men, the backs of the hands and the nose and ears (just as for SCCs). As with most skin cancers, they are most common in those with sun sensitive skin who have had the most UVR exposure.
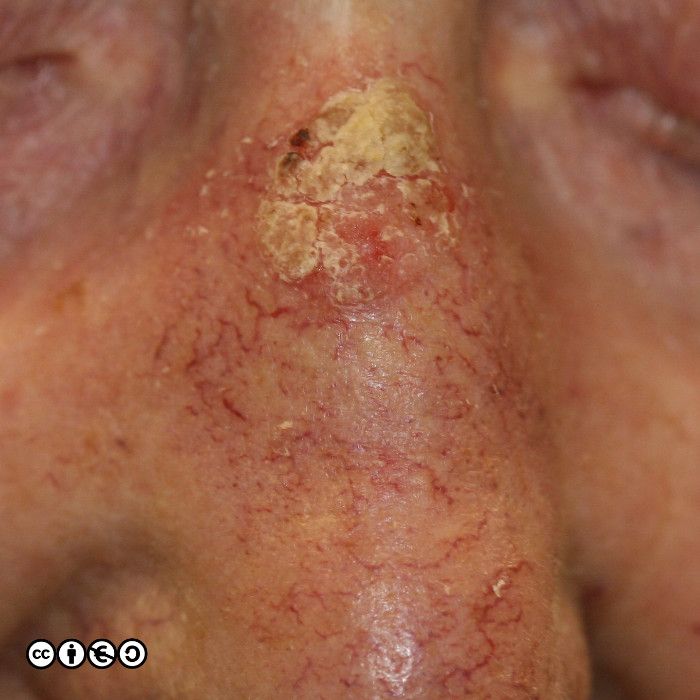
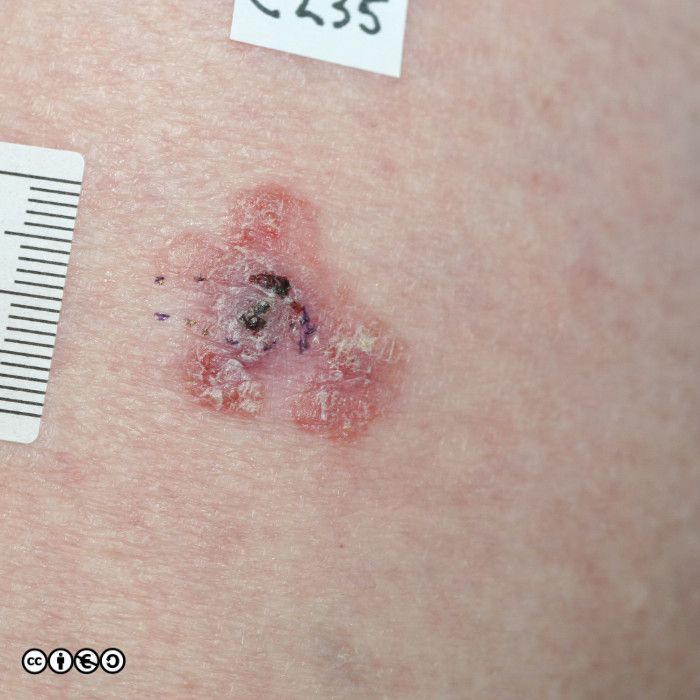
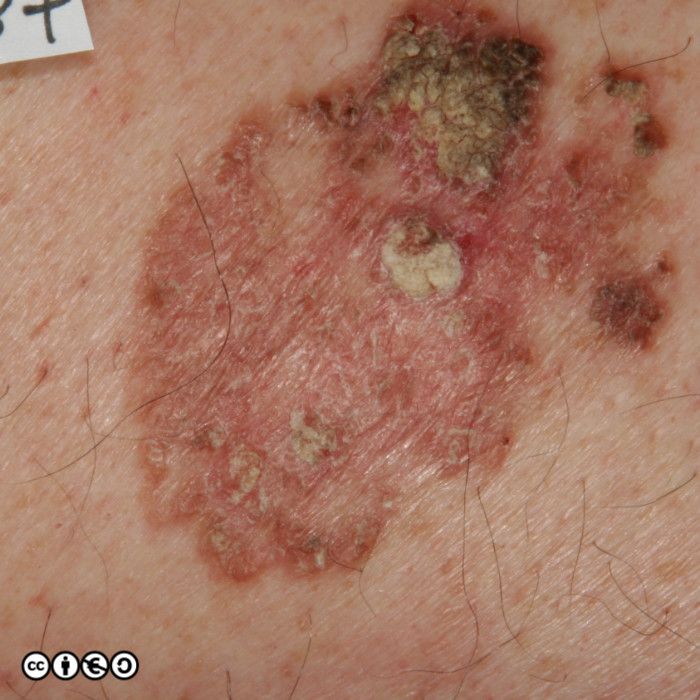
Actinic keratoses (AK) are precursors of squamous cell carcinoma in that a very small proportion of AK progress to squamous cell carcinoma. AKs vary in size from 1mm to over 1cm in diameter. They are frequently multiple with some patients having 20 lesions or more. Some images of actinic keratoses are shown below.
The distinction between sun damaged skin and early AKs may not be straightforward. In many patients with extensive solar damage, in addition to multiple AKs, there may be many areas that you can feel with your fingertips as foci of roughness. If biopsied, many of these ‘preclinical AK’ lesions would show dysplasia.
There is also considerable clinical variation in what experienced clinicians will describe as an AK. Exact, and agreed upon figures for AK incidence are therefore not known, but all agree they are the most common dysplastic or neoplastic lesion of skin (i.e they are much more common than SCC or BCC).
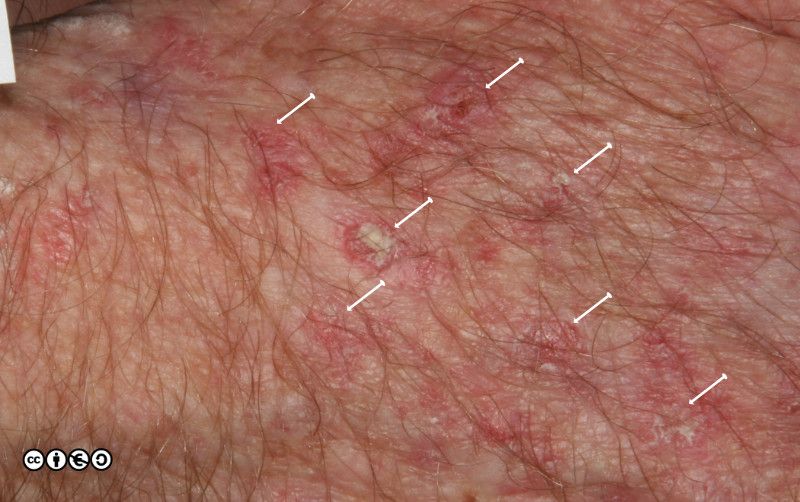
The author can rarely sit on a bus in Edinburgh without spotting many AKs on elderly passengers, and they are often multiple, as the image below shows (in which only some of the AKs are marked).
Should all actinic keratoses be treated?
The exact proportion of AKs that progress to SCC is still debated, and this influences views on how aggressively they should be sought out and treated. For instance, one estimate is that the chance of a single AK progressing to a SCC is around 1:1000/year (but remember a single patient may have 10-20 actinic keratoses). It is also thought that many regress (at least over the short term) — perhaps around 25% in one year. There are other figures that place the risk of malignant transformation much higher, however. Although there is little systematic evidence on which to base strong recommendations, in practice, the default option is to treat AKs with the following arguments being used to justify this course of action.
- Cosmetic. Most people would prefer not to have a heaped up scaly red lesion on their skin.
- Progression to SCC: Some AKs may progress to SCC and we have little explicit criteria to decide on which ones will regress or fail to progress. Perhaps larger ones are more likely to progress.
- Diagnostic error: You cannot always clinically be certain that a larger AK is not a SCC.
Carousel of 10 AK images
Below are 10 images of AKs. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
Intraepithelial carcinoma (Bowen’s disease or in situ carcinoma)
For present purposes, I will consider the terms intraepithelial carcinoma and Bowen’s disease to be synonymous.
In Bowen’s disease / IEC, the clone of cells is confined to the epidermis and has not breached the basement membrane. Such lesions are, by definition, not malignant. By contrast with actinic keratoses, in Bowen’s disease / IEC the dysplasia involves the full thickness of the epidermis. One can envisage Bowen’s disease as further along the pathway of carcinogenesis than an AK.
IEC is the result of sun exposure and therefore follows the usual risk factors. However some cases of IEC may be the result of other carcinogenic agents such as arsenic.
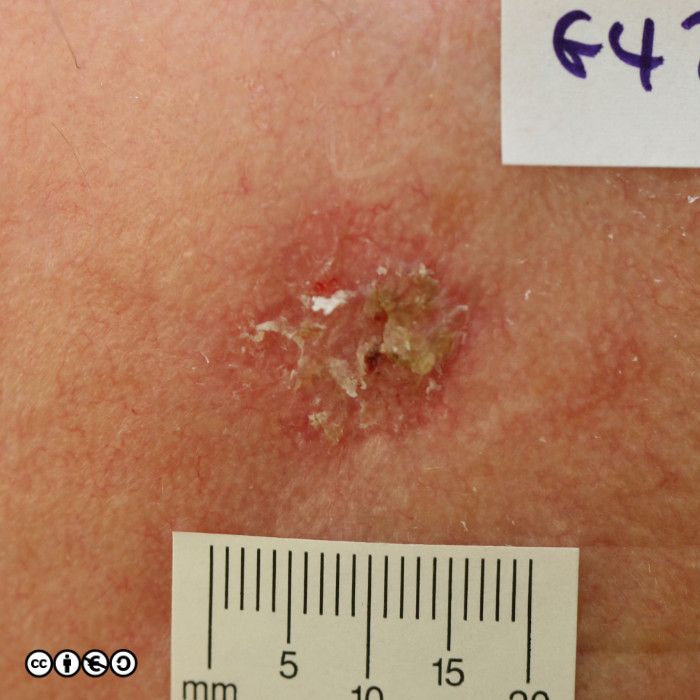
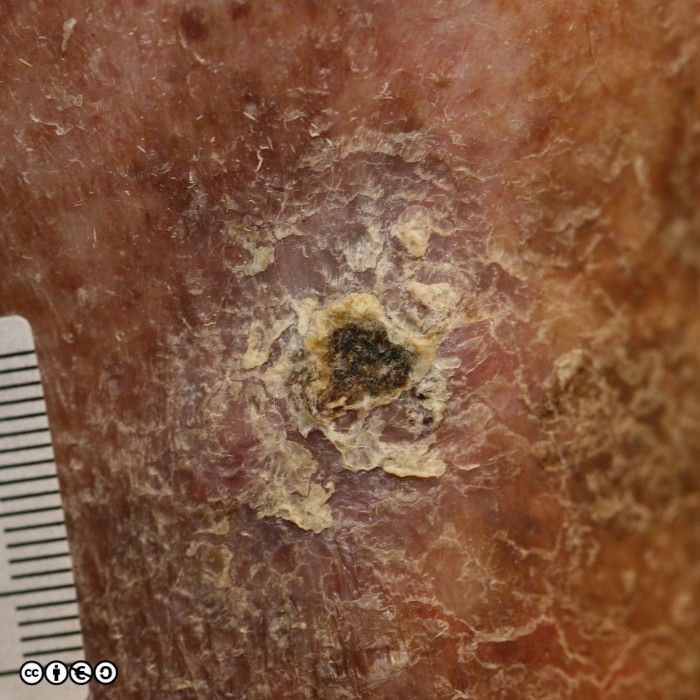
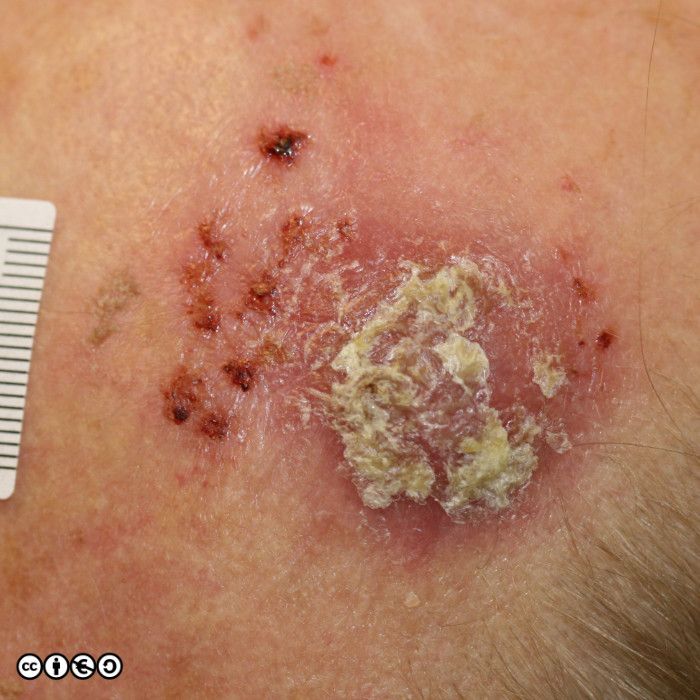
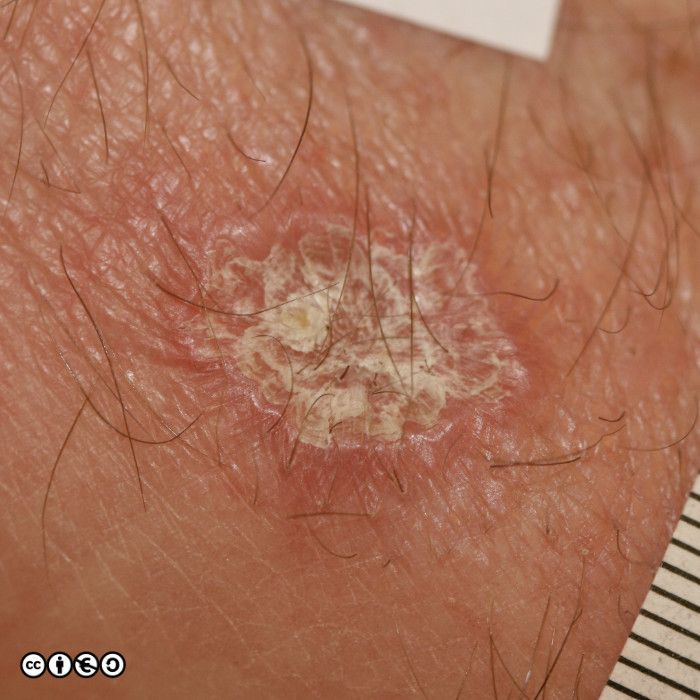
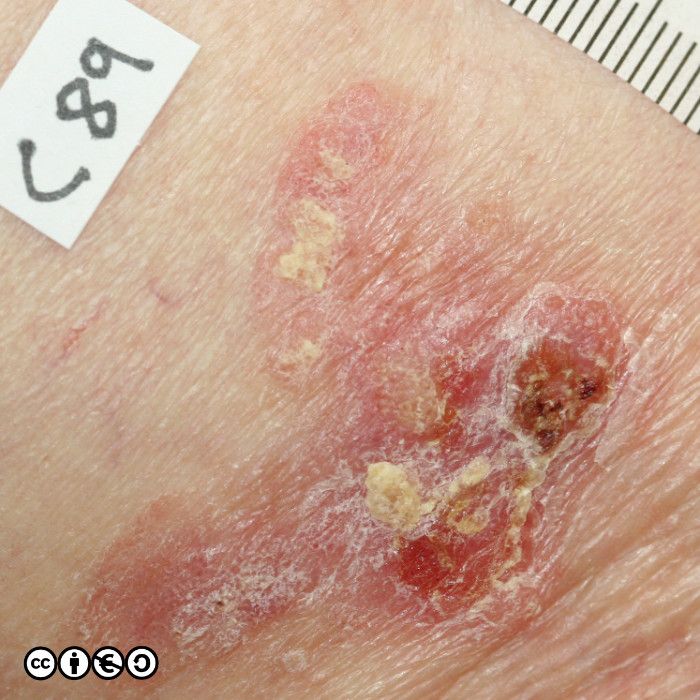
Some images of IEC/Bowen’s are shown below.
IEC/ Bowen’s disease is a precursor of squamous cell carcinoma and the rate of progression to squamous cell carcinoma (~10%?) is higher than for actinic keratoses, although (again) the figure I have quoted of ~10% can be challenged. Histopathological confirmation of the diagnosis may be required with an incisional biopsy to assay for any invasion (and hence the presence of an SCC). All surgical samples of presumed Bowen’s disease must be sent for histopathological examination.
Carousel of 10 IEC images
Below are 10 images of IECs. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
AK or IEC?
The above account makes clear that the AK is a focal area of dysplasia and IEC/ Bowen’s is full thickness dysplasia. Can these two lesions be confused clinically? Yes, is the answer. But an imperfect rule of thumb is that AK tend to be smaller and focal, whereas IEC tend to be plaque like and much larger than most AKs. Do not worry more about this at this stage, as we will come back to this in the virtual clinics.
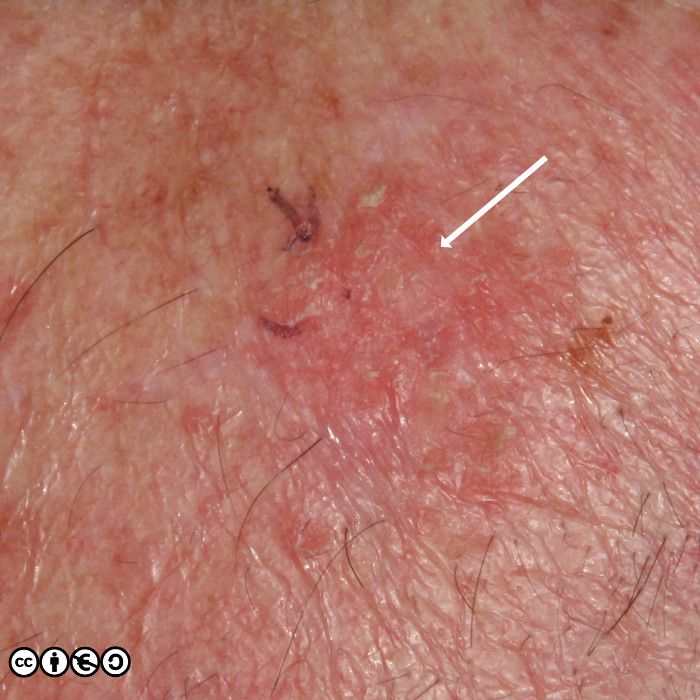
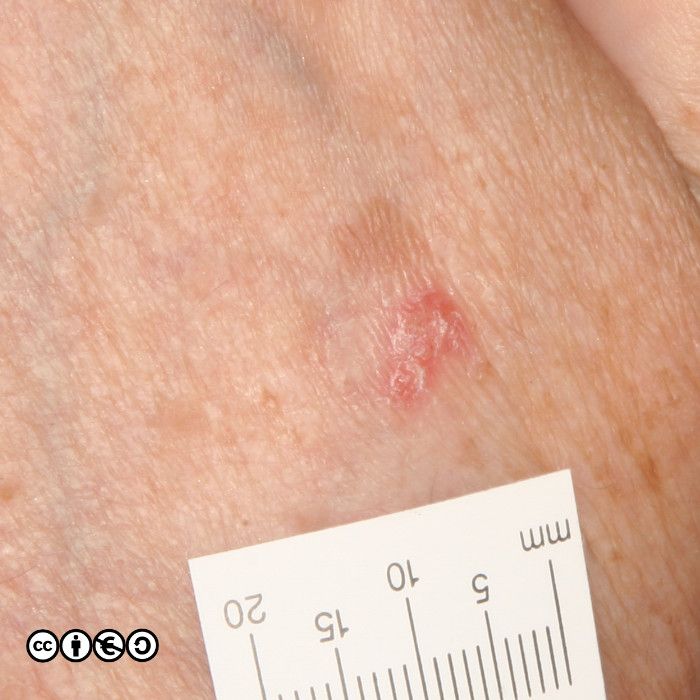
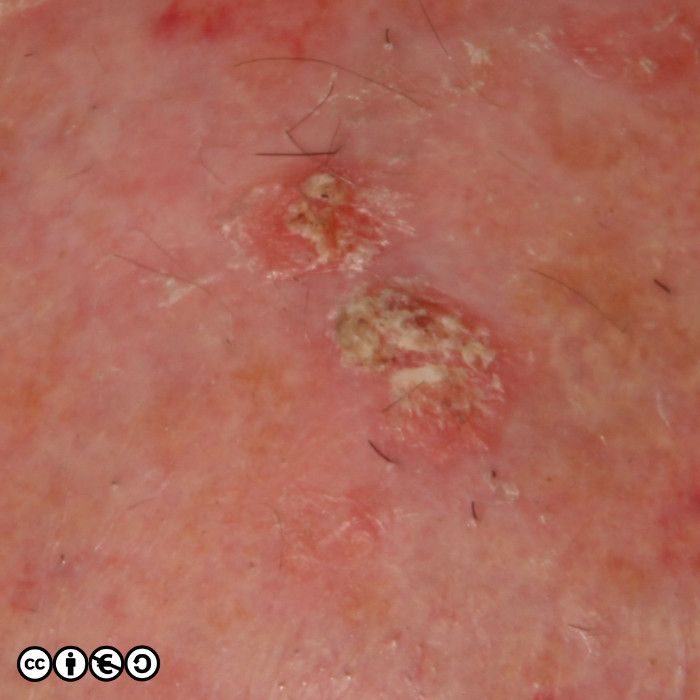
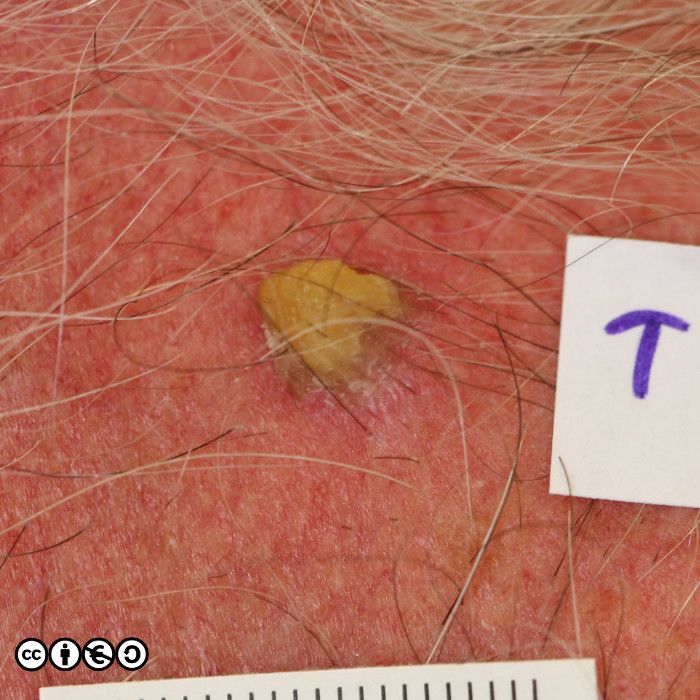
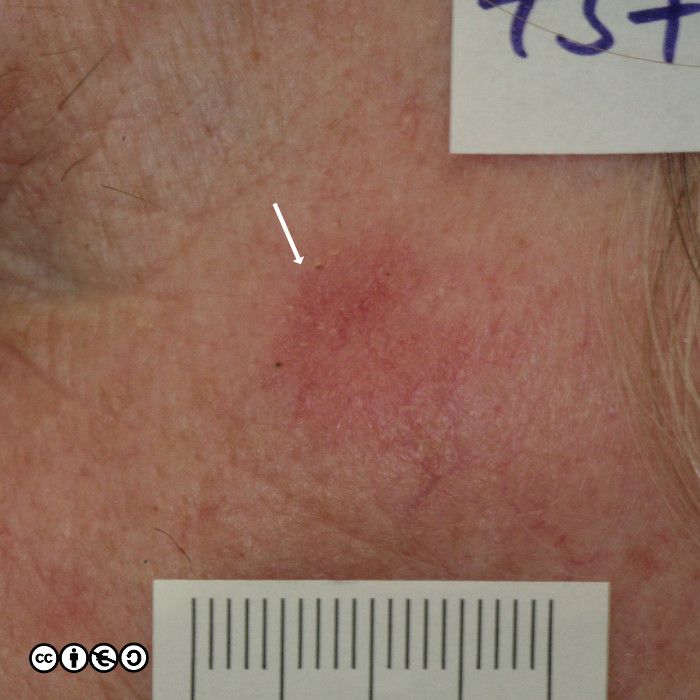
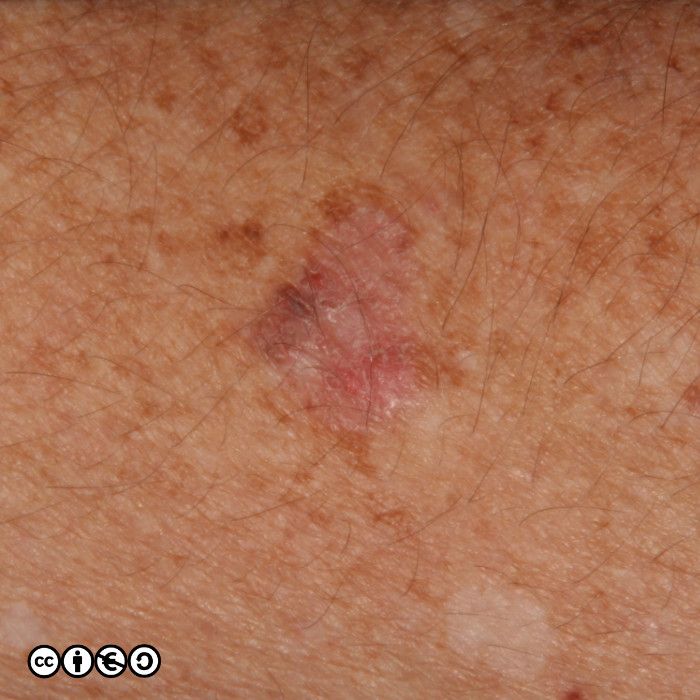
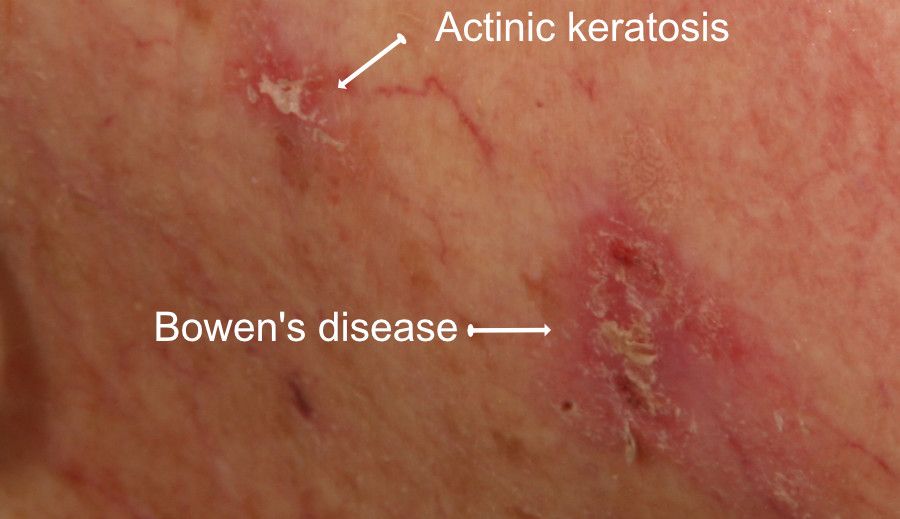
But the image below shows how the difference clinically may only be a guide. One lesion showed an AK on histology, whereas the other showed an area of IEC.
Treatment of AKs and IEC: the short version
Actinic keratoses and intraepithelial carcinomas affect the epidermis only — by definition there is no invasion. The risk of progression or serious harm from an AK is considered low. Destruction of the superficial skin will therefore often suffice, either with cryotherapy or with curette and cautery. There are also topical chemotherapeutic agents that may be appropriate in some instances, and I will discuss these in the later skin cancer therapy chapter.
Bowen’s disease or IEC has a higher risk of progression (than AK), and whereas cryotherapy or curette and cautery may suffice, excision may be warranted in some instances.
Keratoacanthoma (KA)
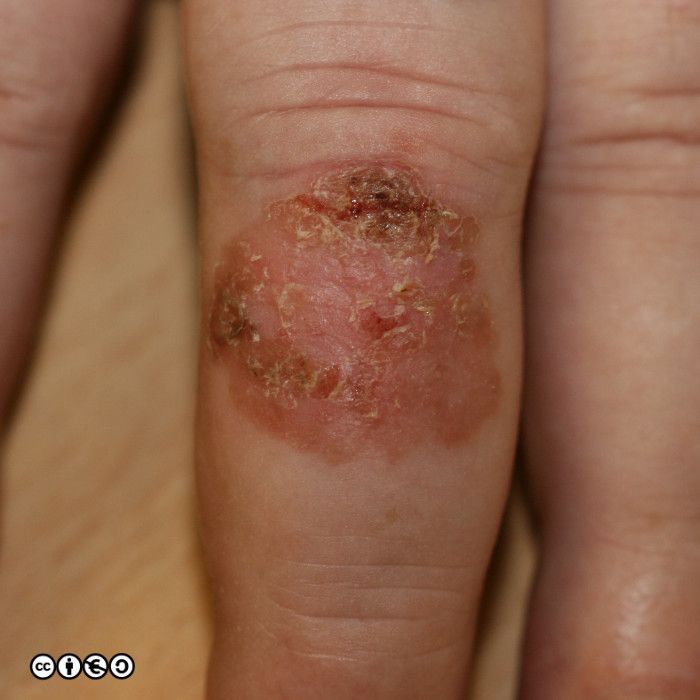
Keratoacanthomas (KA) are biologically fascinating lesions. Morphologically, they resemble a SCC but they behave very differently. The clinical scenario is as follows:
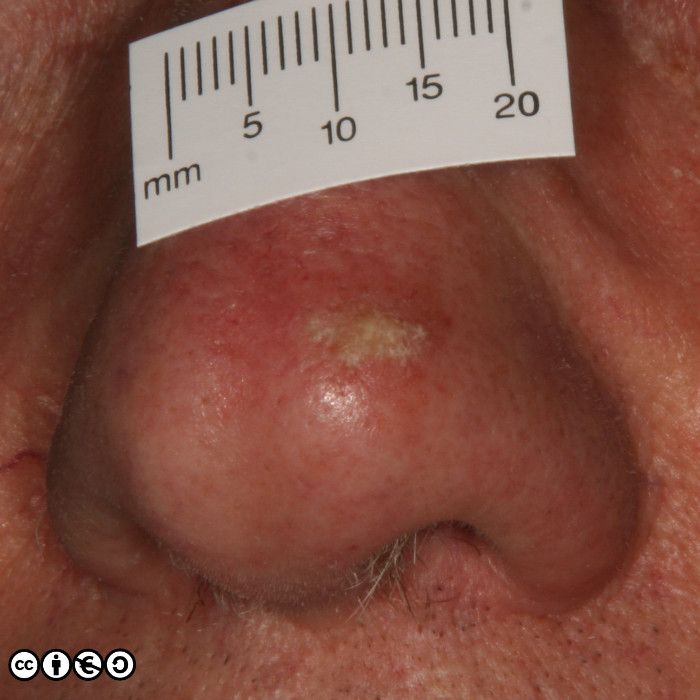
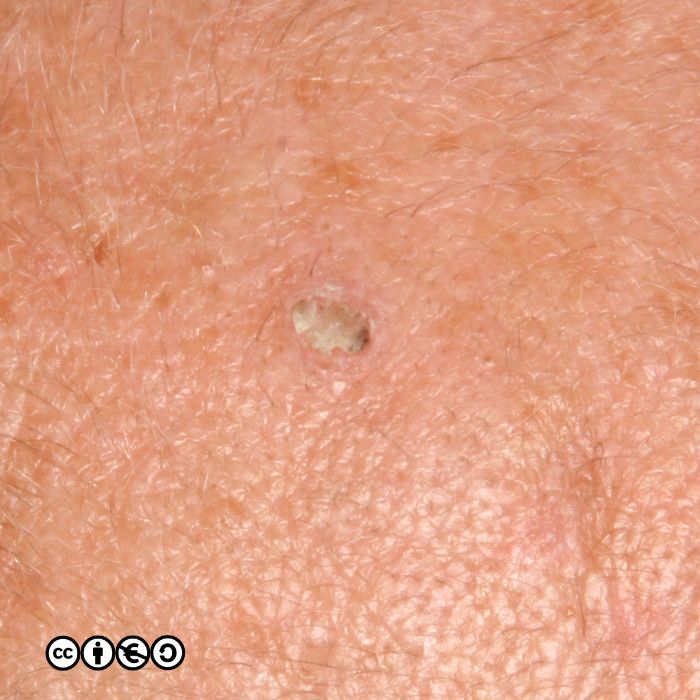
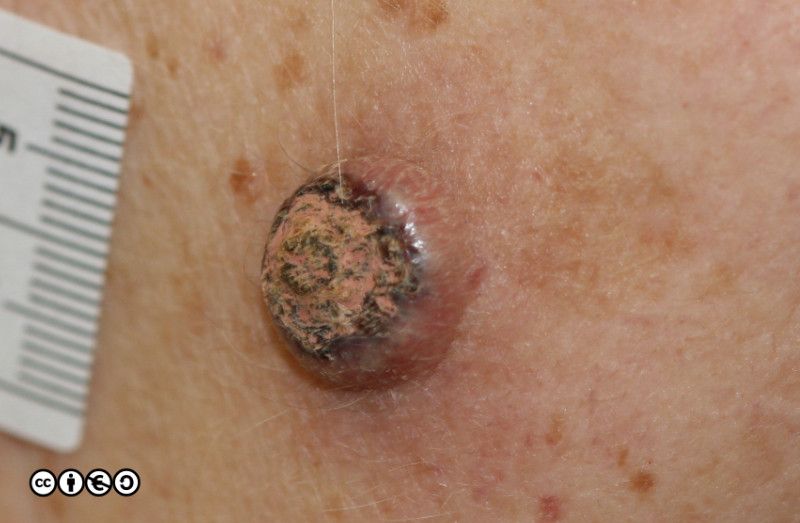
A lesion that looks like a volcano-like SCC grows very quickly over a period of 6-8 weeks, perhaps attaining a size of up to 6cm or more. (image below).
Unlike SCC, keratoacanthomas:
- involute and disappear without any treatment.
- do not metastasise.
- when they do disappear they tend to leave an unsightly scar.
- are not premalignant.
Keratoacanthomas are less common than SCCs, but are more common in the usual skin cancer risk group (sun sensitive skin and high UVR exposure). They are occasionally seen in younger people without a history of excessive UVR exposure.
Keratoacanthoma or squamous cell carcinoma?
From a clinical (rather than biological) perspective the main issue is distinguishing keratoacanthomas from SCCs. The short rapid growth is a clue as is the typical ‘volcano’ morphology. However, both these features can be seen in fast growing SCCs, which are more common than keratoacanthomas.
In practice, the fact that most keratoacanthomas heal leaving an unsightly scar suggests that keratoacanthomas should be excised as though they were SCC. This approach is bolstered by the fact that for a histopathologist to diagnose a keratoacanthoma with confidence, an incisional biopsy needs to be across the whole lesion (rather than say a small punch biopsy). In the majority of instances the appropriate management is therefore to manage as for SCC, and completely excise the lesion.
Not treating a SCC is a worse offence that ‘over-treating’ a keratoacanthoma.
From a student’s perspective, remember that a KA would involute but it is better not to give it the chance to do so.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.