Vascular lesions
Vascular lesions of the skin are common. Some are congenital, but most are acquired and can be viewed as benign tumours. Malignant vascular tumours are rare. Do not worry about the pathology or aetiology, but learn to recognise what may be differentials of the major skin malignancies.
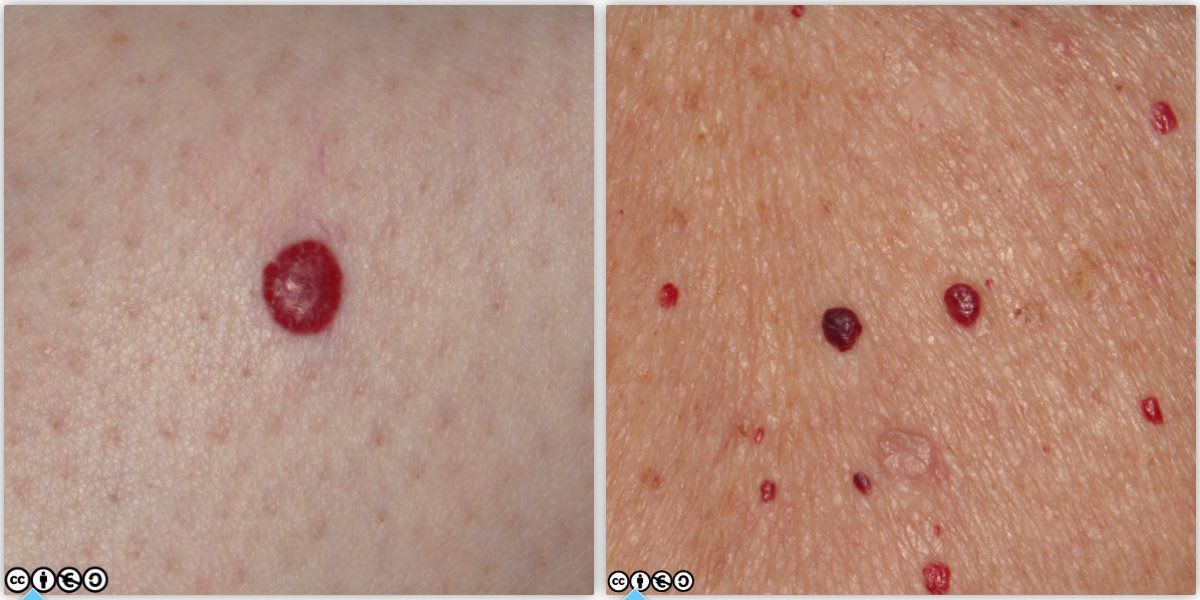
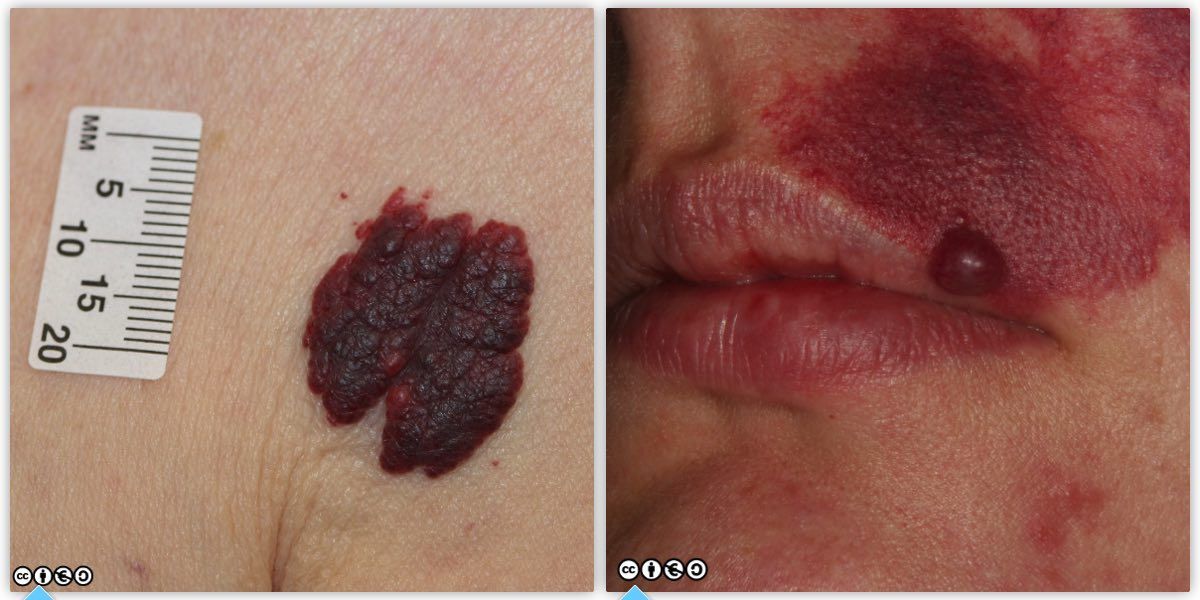
Cherry angiomas (Campbell de Morgan spots) :These are ubiquitous and rarely cause concern (images below).
In middle age and beyond many people develop angiomas that can mimic melanoma. If you can confidently remove the blood by pressure (and often the lesion will collapse and shrink temporarily in volume after you do this) you do not need to worry further.
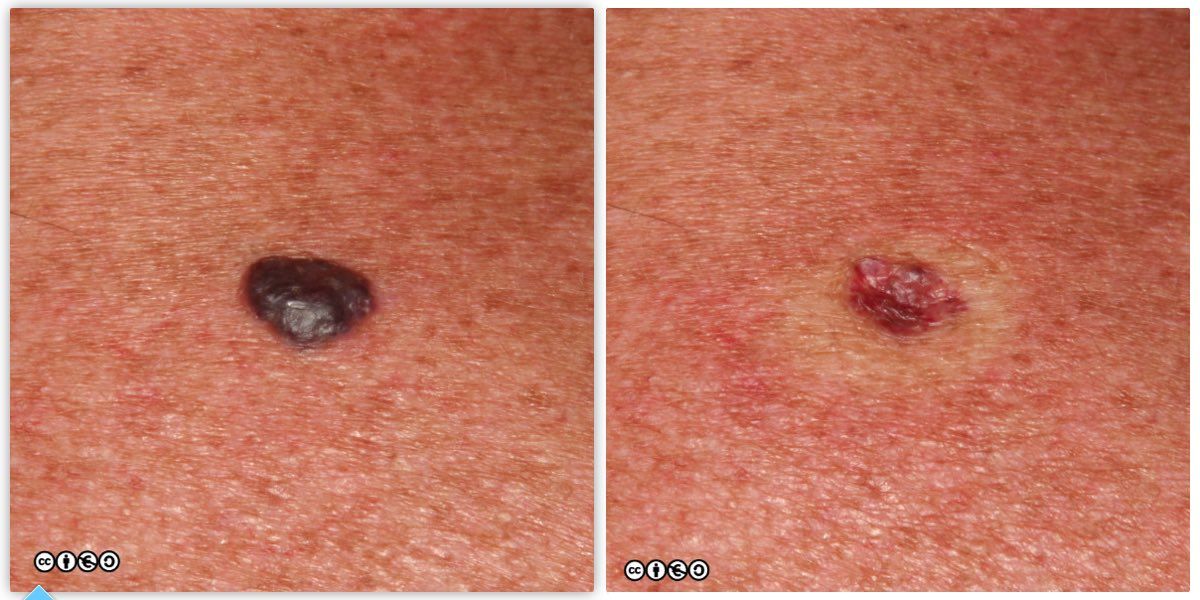
The lesion on the left is before pressure; the lesion on the right, after pressure has been applied. (images below)
If you are not certain whether you are dealing with melanin or haemoglobin, you need to seek expert advice. Not all vascular lesions will blanch with pressure: the physical sign is only diagnostic if positive.
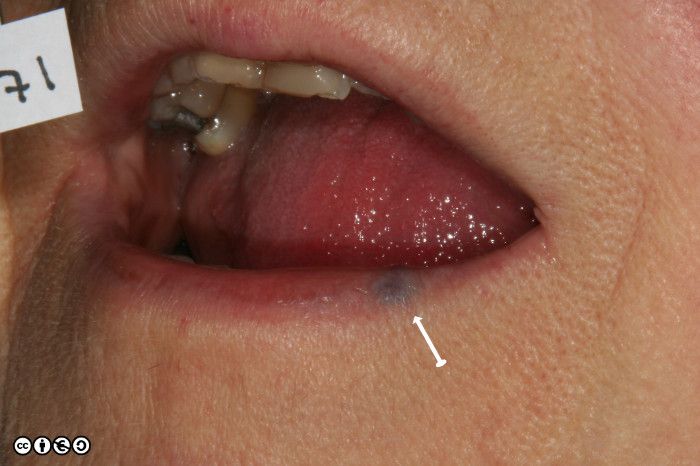
One variety referred to as a venous lake, is commonly seen on the lips, is easily compressible and is often confused with melanotic macules of the lips which are not compressible (discussed in the previous chapter).
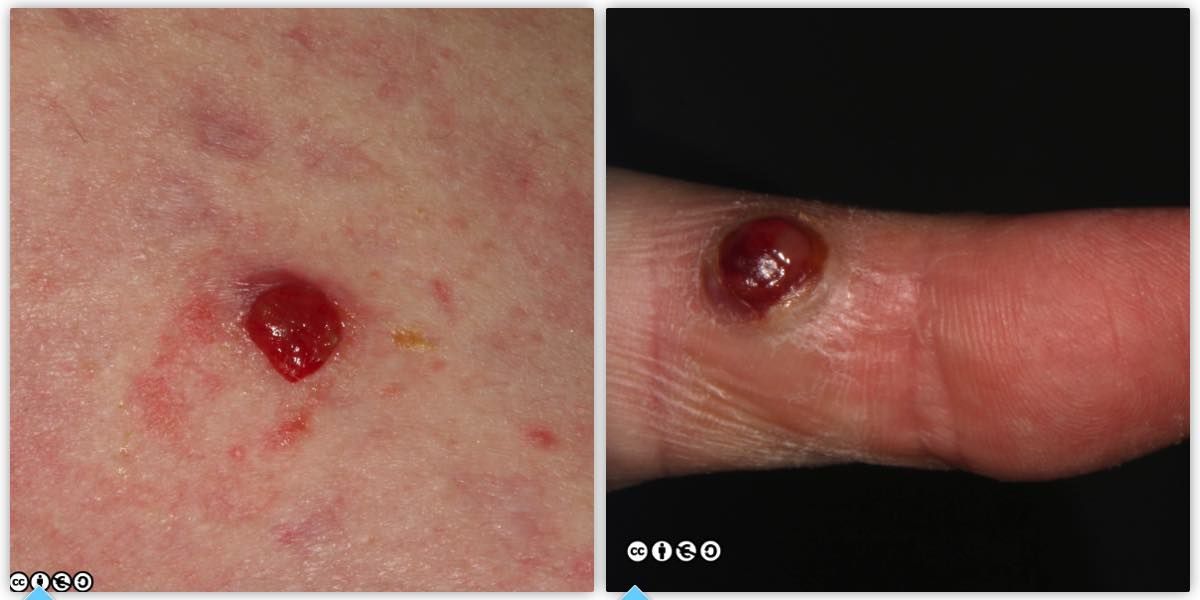
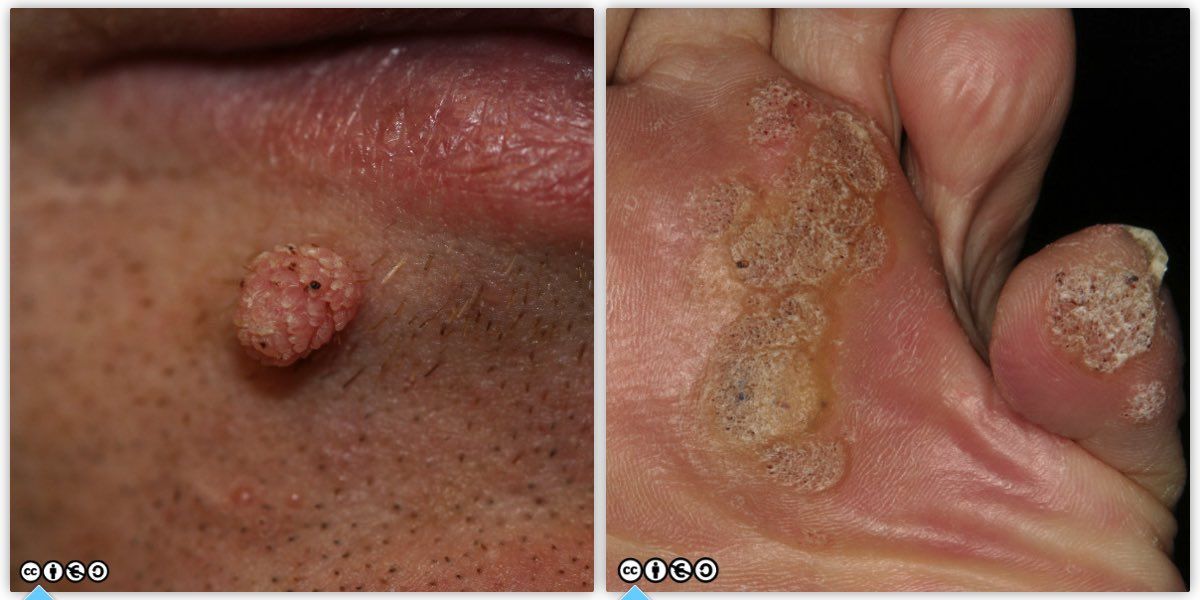
Pyogenic granulomas are best viewed as a vascular proliferation in response to wounding, and are common on the hands and around the mouth. They occur in children, as well as adults. Because they bleed with minimal trauma they are often curetted (or excised). Two examples of pyogenic granulomas are shown below.
Pyogenic granulomas can mimic amelanotic melanomas or pigmented melanomas, and it is not too uncommon for a presumed pyogenic granuloma to be curetted, only for the pathologist to report the specimen as a melanoma. The history of trauma is not always apparent.
A variety of vascular lesions present at birth or soon after. An example of such a vascular nevus is shown on the left below. On the right there is a port-wine stain, a type of vascular malformation present at birth or shortly afterwards, which become more noticeable over time.
Dermatofibromas
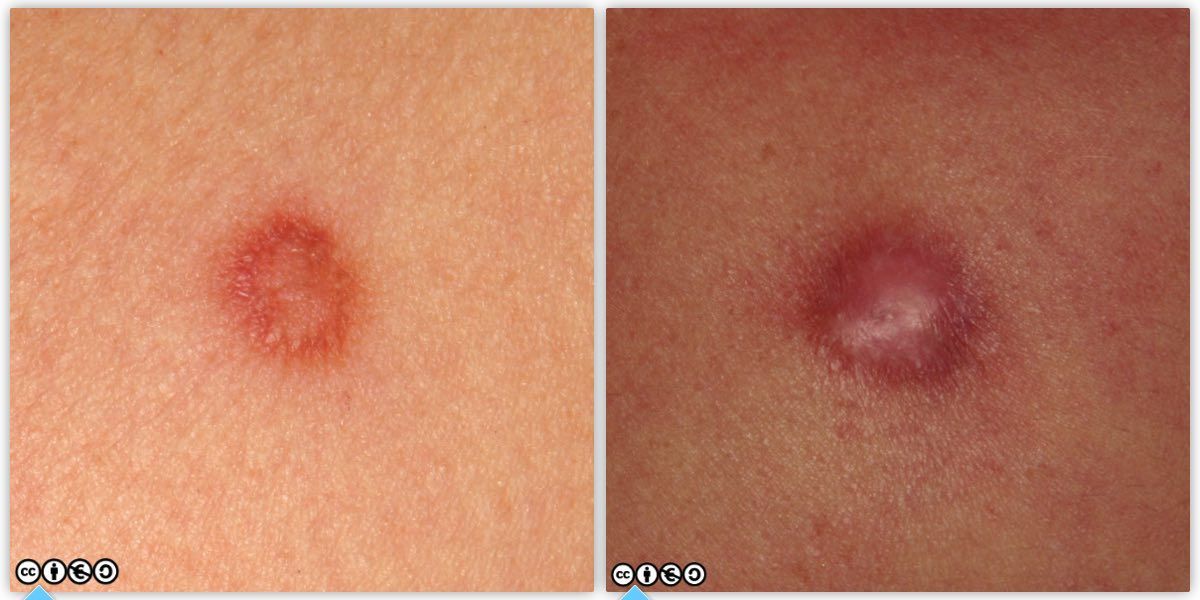
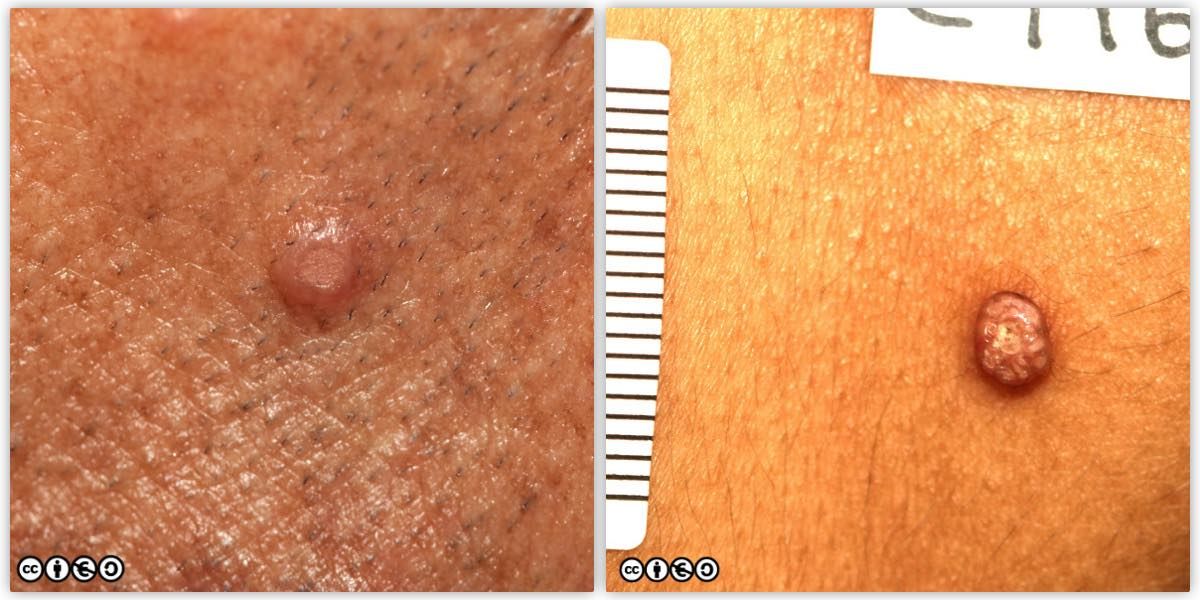
These are firm nodules usually less than two cm in diameter. They tend to appear in early adult life, and are most common on the proximal legs or arms, but can occur anywhere. They are not neoplasms but are thought to be reactive to earlier insults such as insect bites or folliculitis. They are often skin coloured but may be hyperpigmented (melanin), or be erythematous.
Histologically they show a proliferation of fibroblasts in the dermis. A big clinical clue is that they are much firmer than many other nodules, and that they feel bigger than they look. They are often misdiagnosed as melanocytic nevi.
Sebaceous hyperplasia
These are clusters of enlarged sebaceous glands most common on the face. They vary in size between 2-6mm. They have a characteristic translucent and yellow colour and an umbilicated or rosette like shape around a central follicular orifice. They are easily confused with small BCCs by the overconfident. They are often multiple.
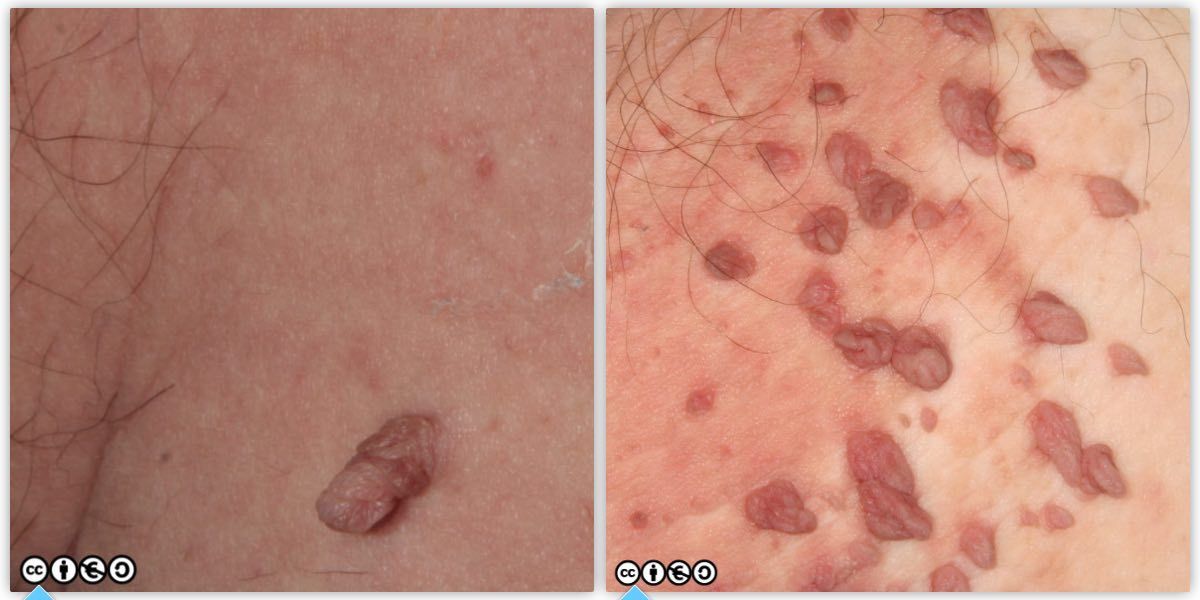
Skin tags (acrochordons)
These are focal overgrowths of epidermis and dermis. Usually multiple and common in flexural areas especially in the obese. They may have histological features of seborrhoeic keratoses or melanocytic nevi. Easier to recognise than to explain what any particular lesion will show pathologically.
Viral warts
These are the common warts of childhood secondary to human papillomavirus infection (HPV), but they occur in adults too. The image on the left is a viral wart on the face, and the one on the right, on the plantar skin.
The diagnosis of viral warts in adults is not always straightforward.
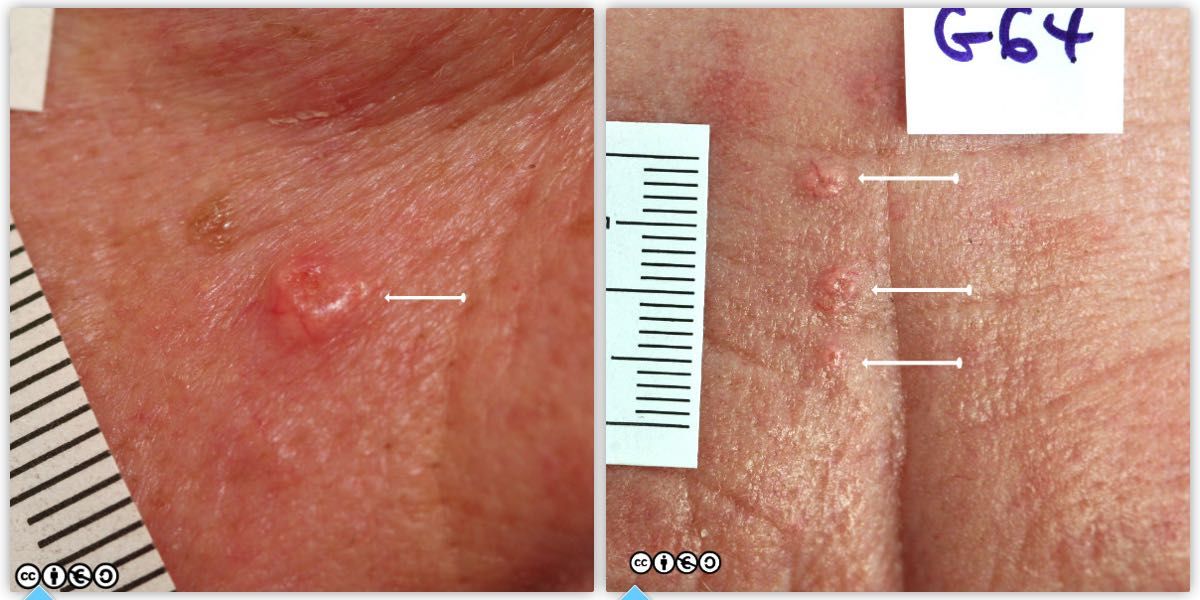
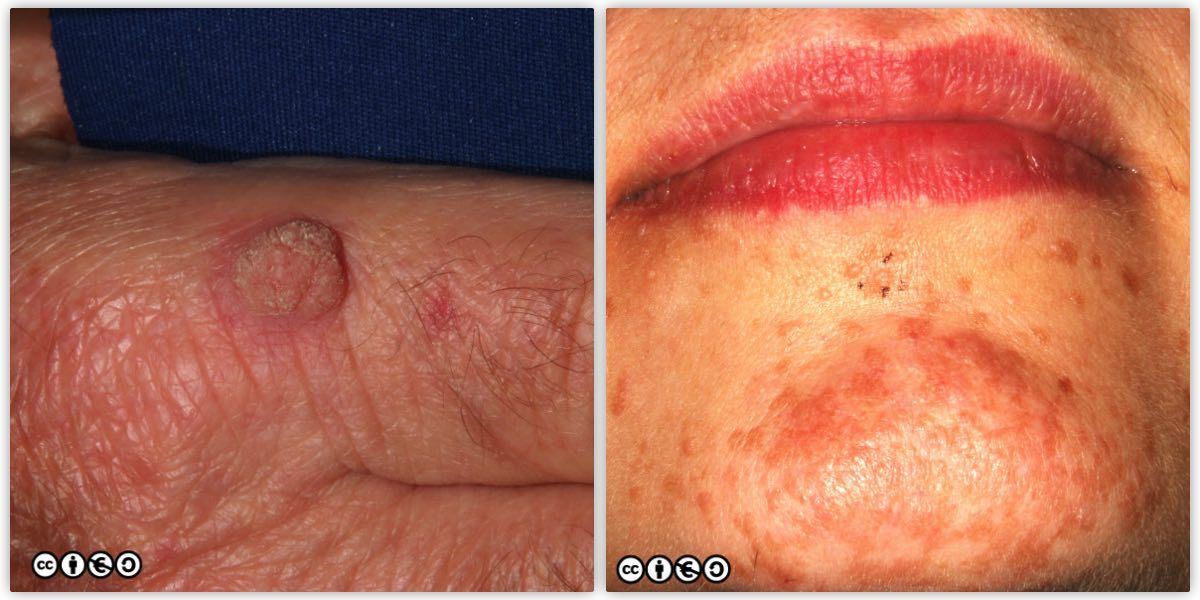
New warts may develop in older persons and can be confused with AKs, seborrhoeic keratoses or even SCCs. Patients who are immunosuppressed are at an increased risk of NMSC and have a much higher prevalence of viral warts. Clinical assessment can be difficult in these patients, and diagnostic suspicion is warranted because a SCC may be misdiagnosed as a benign viral wart. For instance the lesion on the left below is a viral wart but a SCC or a seborrhoeic keratosis comes into the differential. The multiple lesions on the chin of the patient (image on the right below), are plane warts, again due to human papilloma infection. This type of HPV lesion often pigments markedly.
Molluscum contagiosum
This is due to a pox virus infection. Common in children where they tend to resolve over 6-12 months — not as quickly as the parents would like. They are spread by casual contact, for instance used of shared towels, and may be extensive in children with atopic dermatitis. They also occur in adults and can be spread by sexual contact. If they are multiple the possibility of underlying immunosuppression due to HIV should be considered. Occasional giant forms can be confused with a SCC.
Clinically the hallmark is the central umbilication which contains the virally infected epidermal cells.
Epidermal cysts
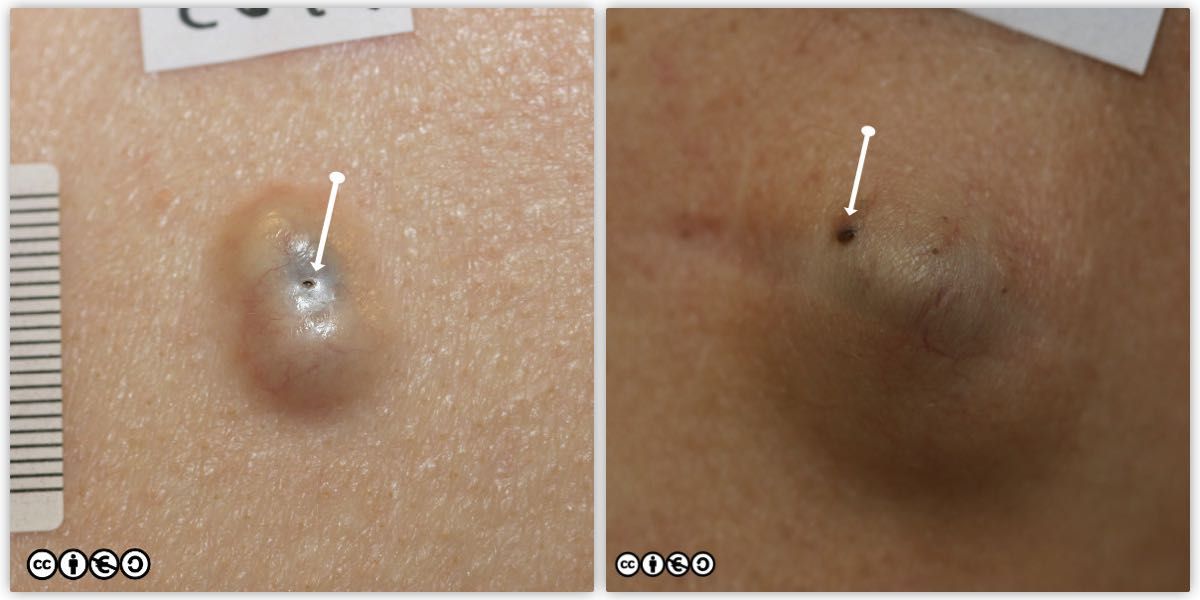
These are wrongly referred to as sebaceous cysts, but they not lined by a sebaceous epithelium, but an epithelium similar to that seen in normal epidermal differentiation. They may contain a punctum — the opening to the surface and remains of the follicular infundibulum that has become obstructed (the assumed mechanism of cyst formation). The punctum is arrowed in the two images below. Note the scar from previous surgery of the one on the right that has recurred.
Comedones
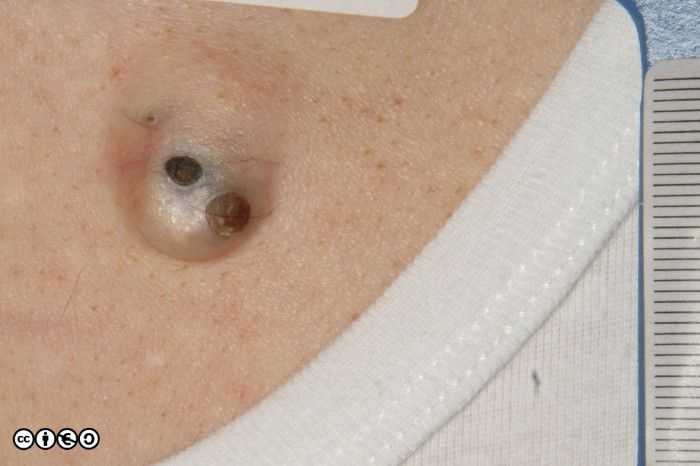
Giant comedones are epidermal cysts with a prominent opening (or more than one) as is visible in the image below. They are still referred for review as suspected melanomas.
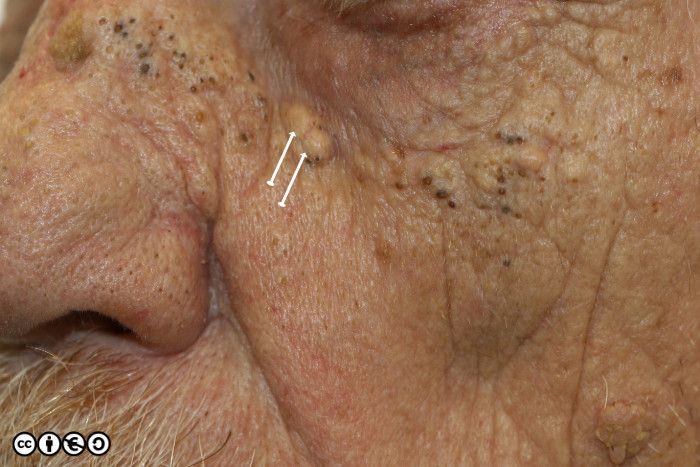
Comedones and small cysts are also seen with elastosis in people who have had high UVR exposure. The small comedones are the dark structures in the image below, and white arrows highlight some of the elastic nodules that are yellow and comprise elastotic UVR damage to the dermis.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.