Of all skin cancers melanoma is the most feared by both patients and doctors. The former, because melanoma is a significant cause of mortality; the latter because the diagnosis of MM is difficult and relies on the ability to distinguish between the rare suspicious lesion and the ubiquitous harmless pigmented lesions that are found on all of us. Clinicians who claim certitude in this area are likely deluded.
The term malignant melanoma is synonymous with melanoma: there is no such thing as a benign melanoma.
This chapter in one minute
Vignette
Melanoma is a malignancy of the neural crest derived melanocytes. Most melanomas are pigmented and may be confused with benign melanocytic nevi (‘moles’) or other benign pigmented lesions of the skin that are found on all of us. A minority (up to 30%?) of melanomas are the result of malignant change in a former ‘mole’. Melanomas, unlike virtually all other skin cancers metastasise early, and it is these metastases that lead to death.
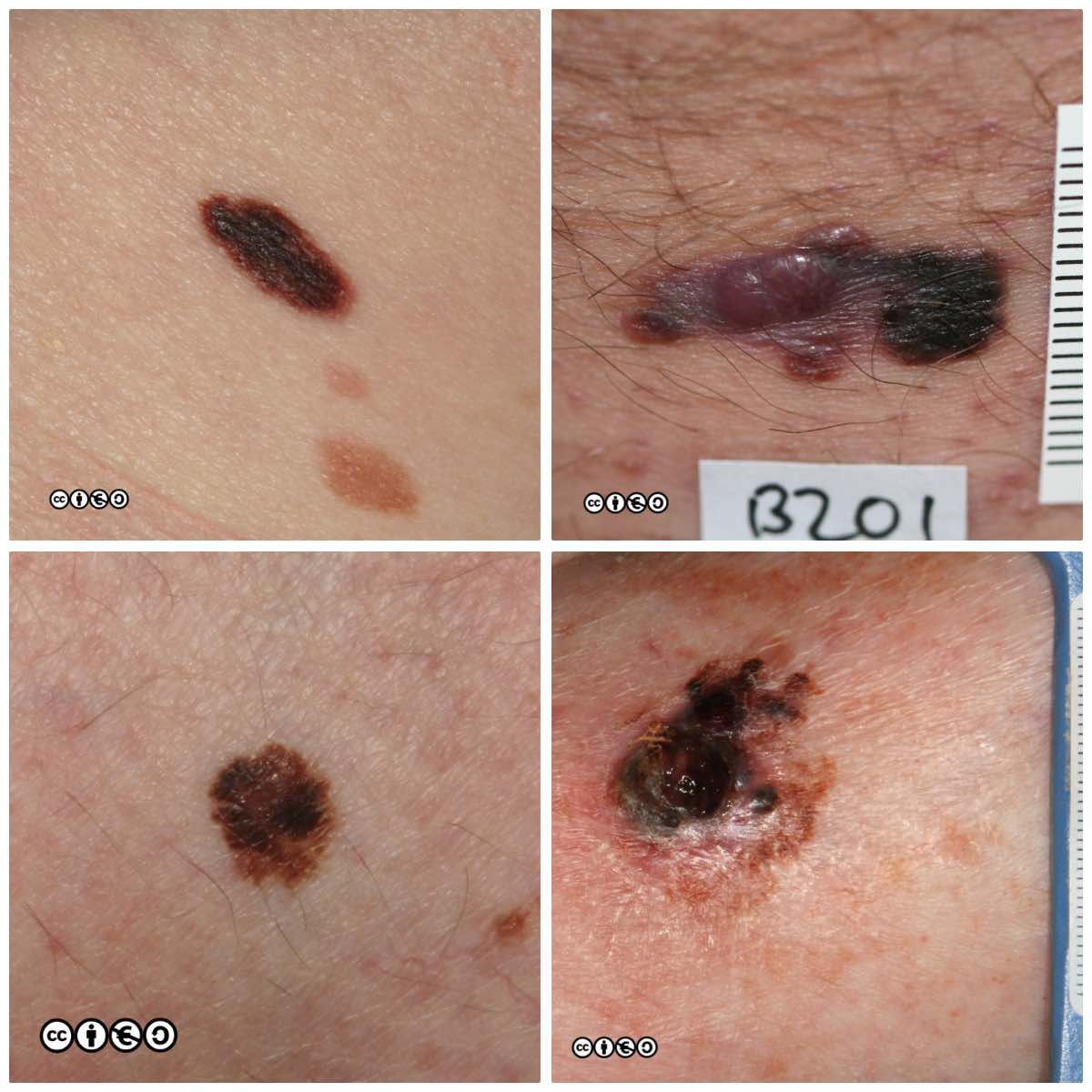
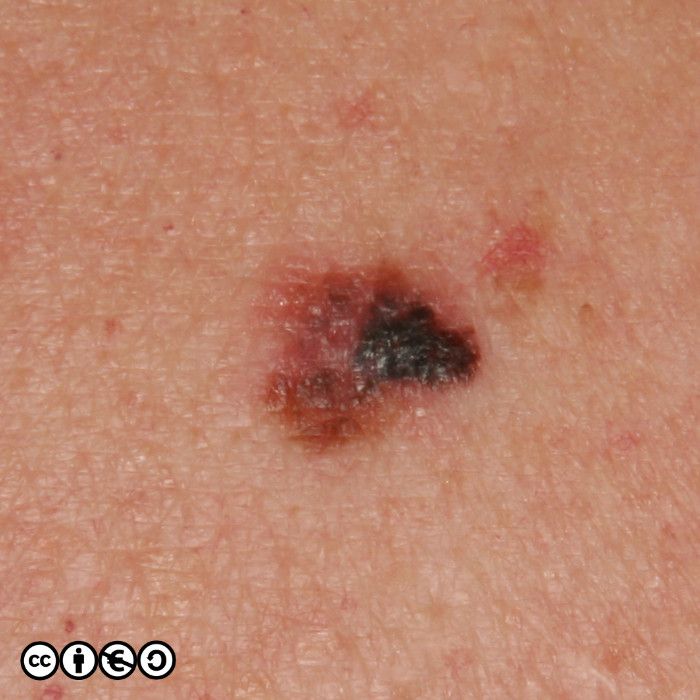
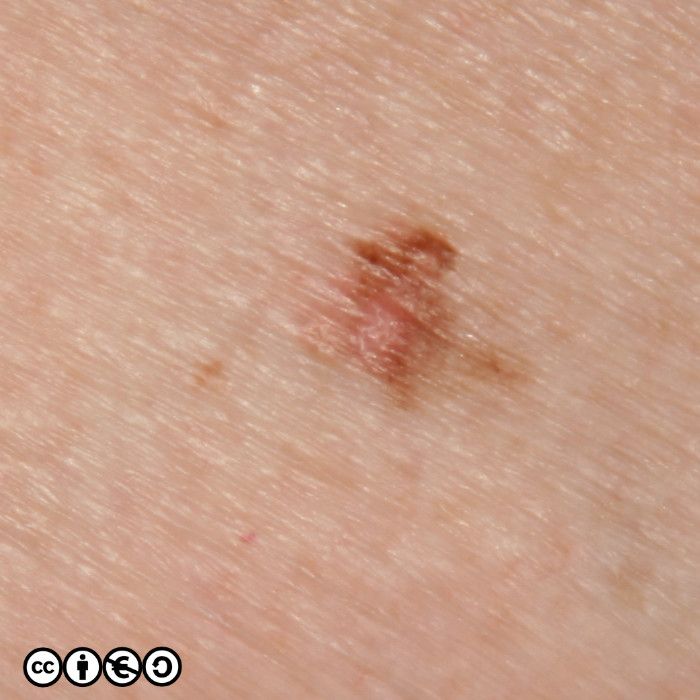
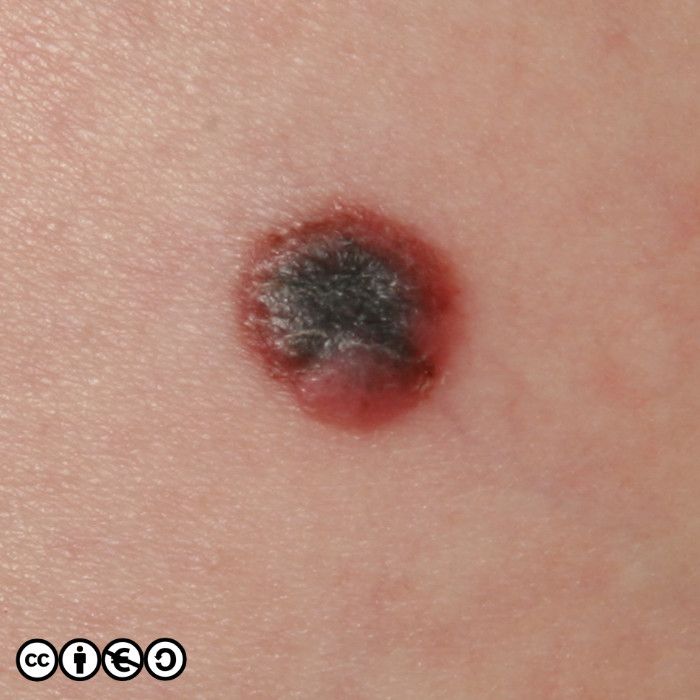
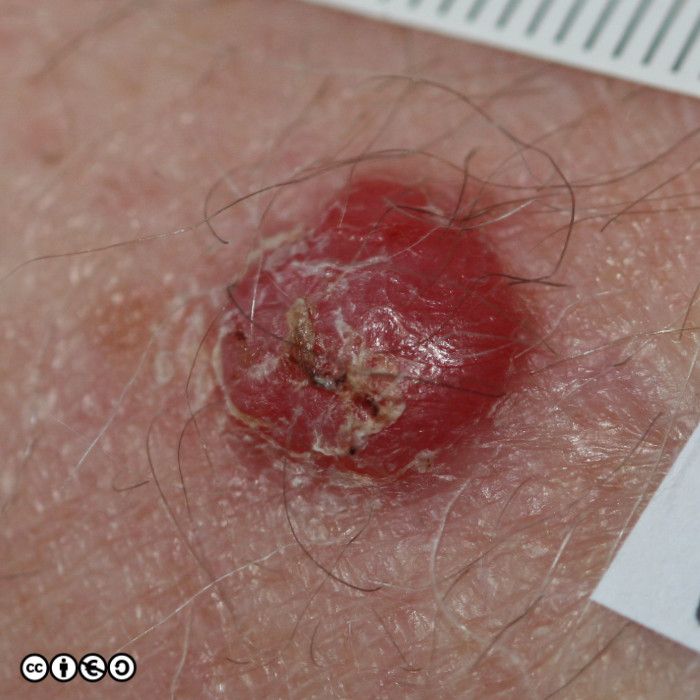
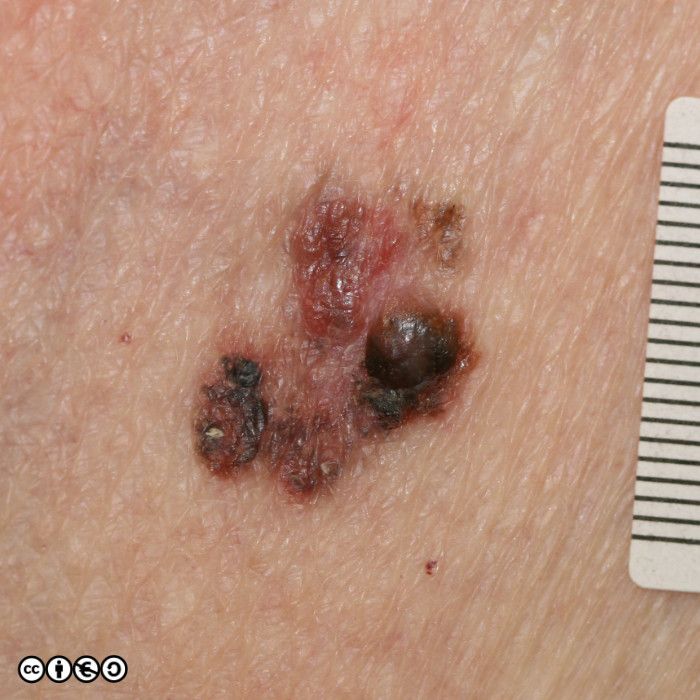
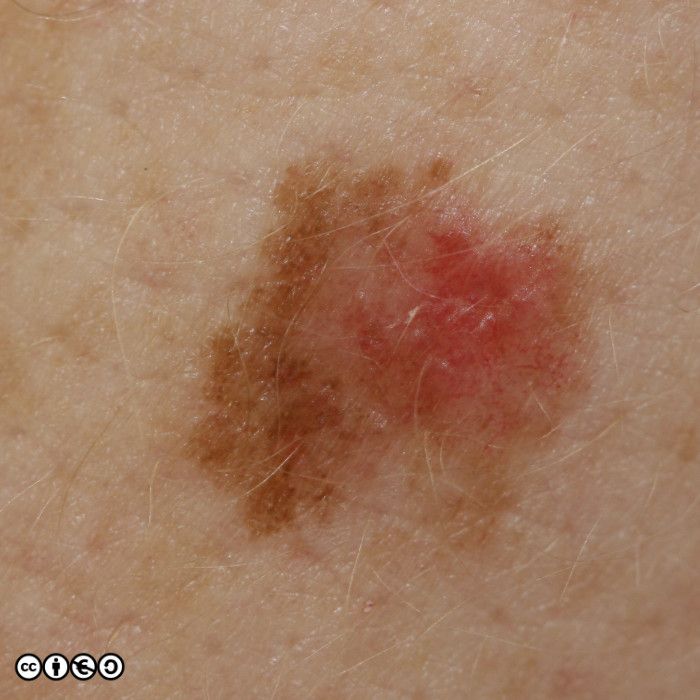
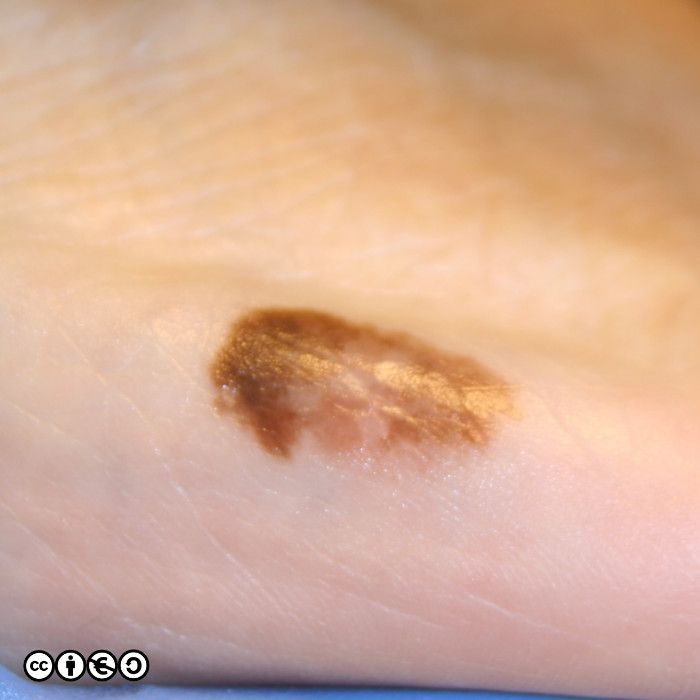
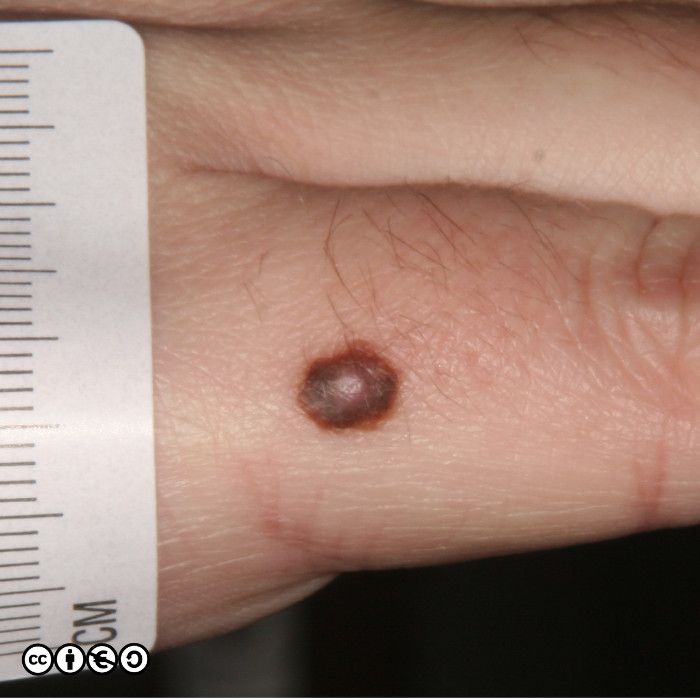
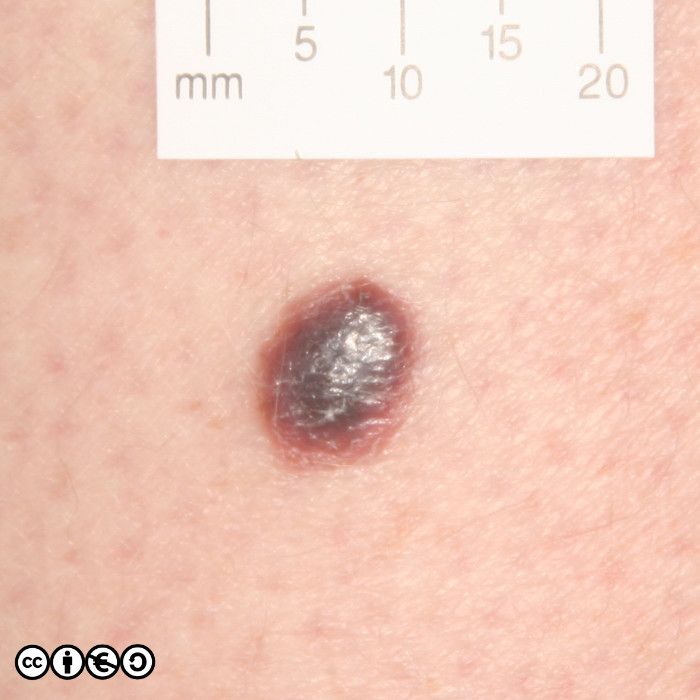
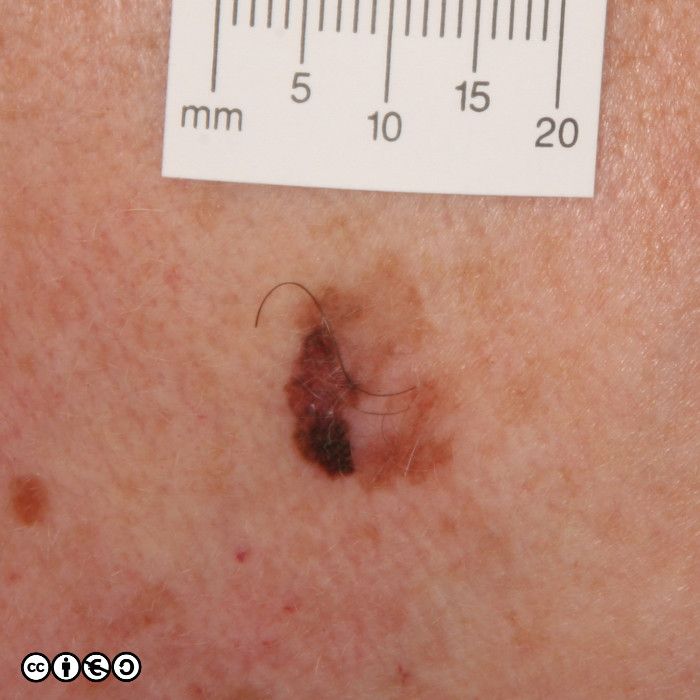
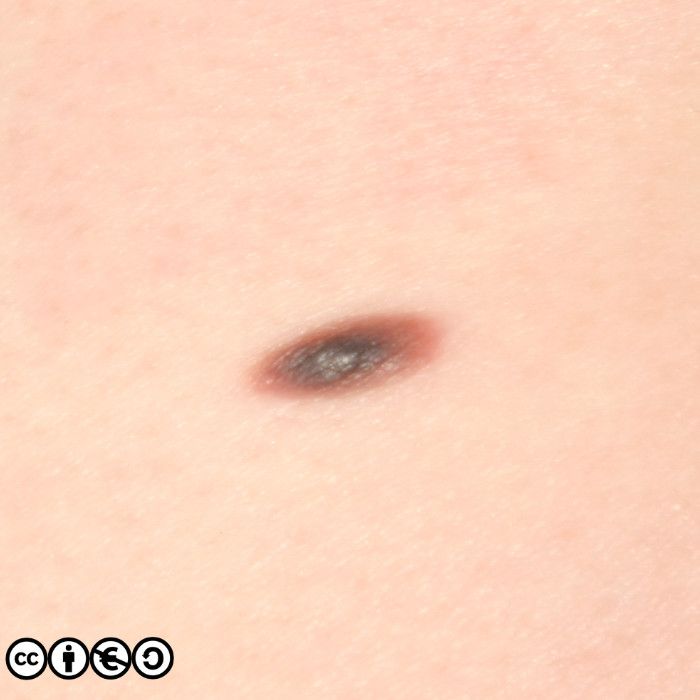
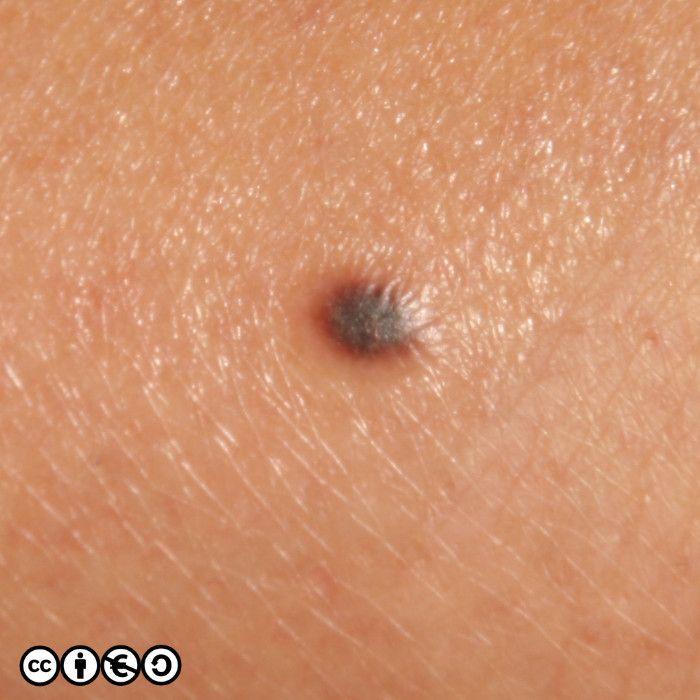
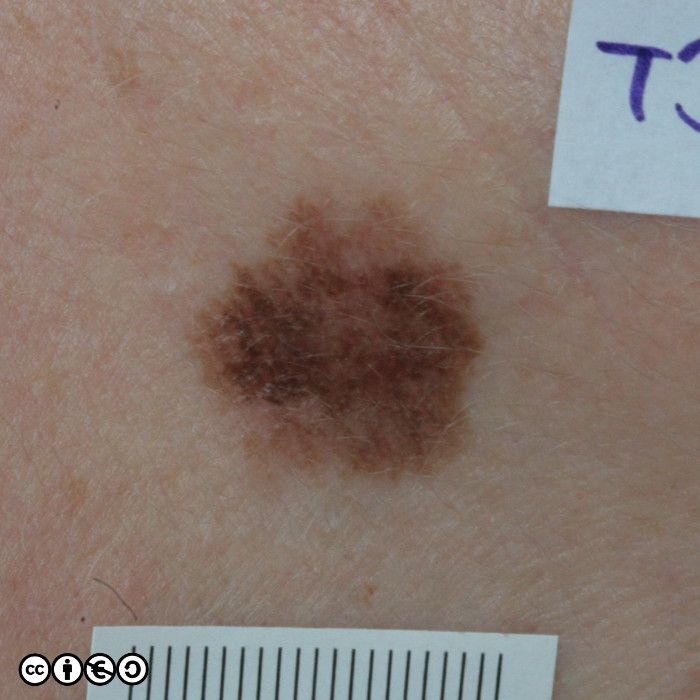
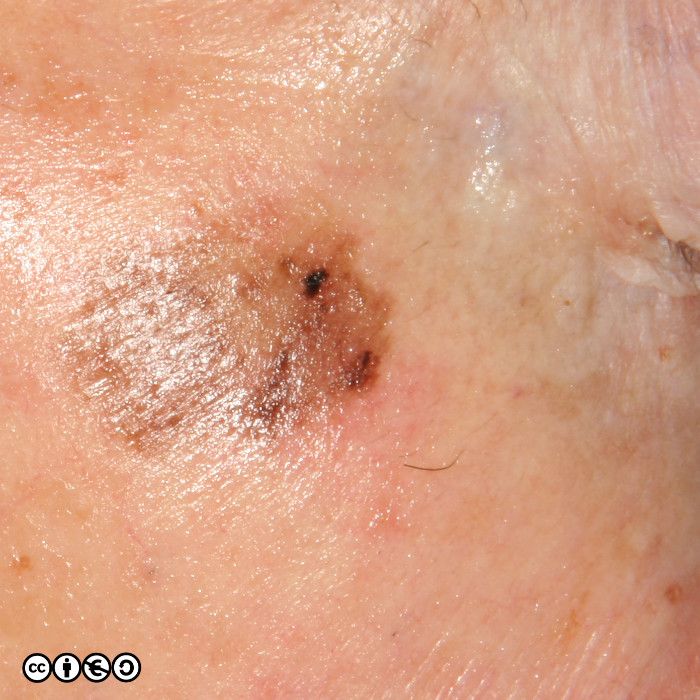
The main cause of melanoma — as with most skin cancers — is UVR exposure and sun sensitive skin. Some images of melanomas are shown below.
Epidemiology
The incidence of MM in Northern Europe is 17:100,000 with a median age of 53. Melanomas are more common in women than men (3:2) in some (but not all) populations. Melanoma is therefore much less common than non-melanoma skin cancer (NMSC), and accounts for about 10-15% of all skin cancers.
Like all the UVR related skin cancers, the incidence of melanoma is increasing every year: for melanoma this increase is about 4% per year.
The majority of deaths from skin cancer are a result of malignant melanoma with a death rate of ~3:100,000.
Melanoma has a much higher case-fatality rate (10-20%) than either SCC or BCC.
Causes of melanoma
Most cases of melanoma can be accounted for in terms of exposure to UVR and sun sensitive skin. There are some patient subsets that you need to be aware of.
Acral melanoma: Around 10% of MM occur on the palms or soles. The absolute incidence of MM at these (acral) sites is the same in all world populations — whatever the colour of their skin or sun exposure. Given that palmoplantar skin is sun resistant, because of the very thick epidermis, it is safe to assume that melanomas at these particular sites are not UVR related. In fact, we are ignorant of the cause of acral melanomas. In some pigmented populations, where UVR related melanoma is uncommon, acral melanomas are the commonest type of melanoma.
Familial melanoma: Up to 10% of MM occur in those with a family history of MM. With a tumour that effects up to ~1% of the population during their life time this clustering will sometimes occur due to chance. However, in some families melanoma almost seems to be inherited in close to an autosomal dominant manner. In some of these kindreds the affected individuals have a larger number of nevi (often several hundred) and these nevi look ‘atypical‘. Clinical clues are therefore a large number of nevi and the presence of multiple family members with melanoma (>2 or 3). In some of these kindreds the underlying genes have been identified, and advice from clinical geneticists should be taken on who should undergo testing (in collaboration with the patient).
Psoralen and UVA (PUVA) therapy : As for squamous cell carcinoma there is some evidence that those who have received higher cumulative doses of PUVA are at an increased risk of melanoma. The evidence is far less convincing than for SCC, but that a known carcinogen like PUVA increases MM rates seems quite plausible.
Immunosuppression: There appears to a be a small increased risk of melanoma in those who are immunosuppressed, particularly following organ transplantation. The increase in risk is much lower than that seen for SCC.
Clinical presentation and clinical subtypes
There are a number of clinical and pathological variants of melanoma. Some of the more common ones are mentioned below.
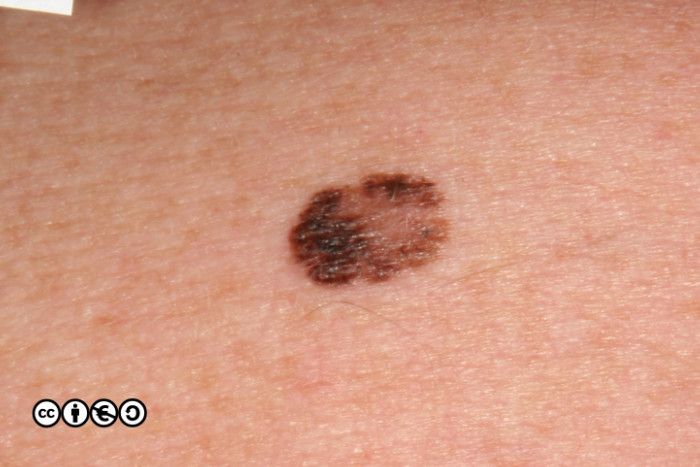
Superficial spreading melanoma (SSM). These are flat or almost flat lesions in which the malignant clones of cells appears to have spread laterally from a central point. They resemble normal flat melanocytic nevi or may even be confused with freckles or lentigines. (image below)
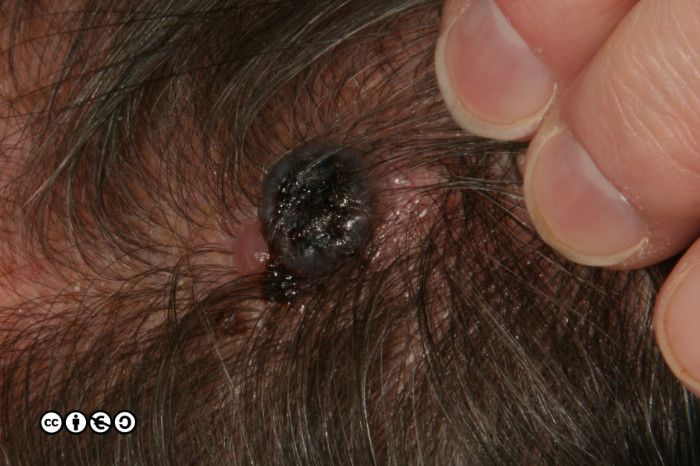
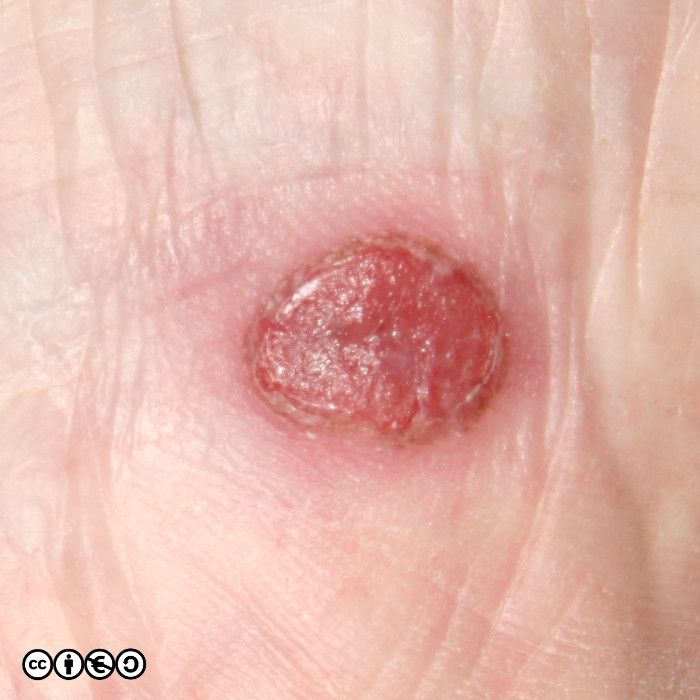
Nodular melanoma. As the name implies these are nodules. Such nodules are inevitably a reflection of a large downward (vertical) collection of malignant cells. It is of course possible to imagine that the nodule represents a later stage of the superficial spreading melanoma in which the cells have acquired the propensity to migrate deeper in the skin. They may be confused with normal melanocytic nevi or angiomas. (image below)
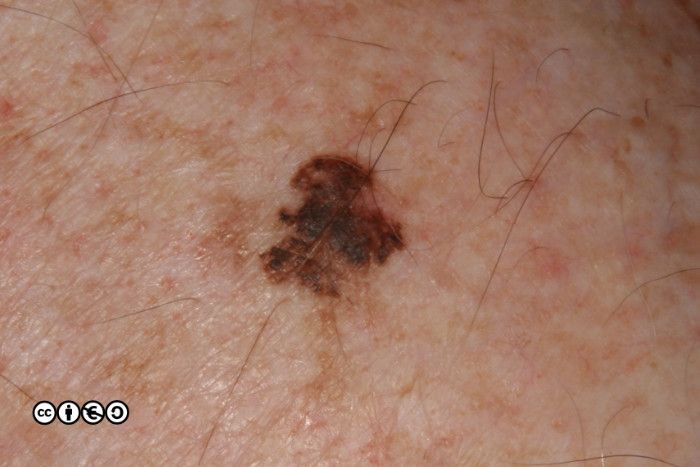
In situ melanoma. This is not a true melanoma but an earlier in situ variant, that we assume might progress to full malignancy. By definition in situ melanoma is confined to the epidermis and cannot metastasise. If we diagnose an in situ melanoma, we tend to think we have caught a future melanoma before it could do any harm. (image below)
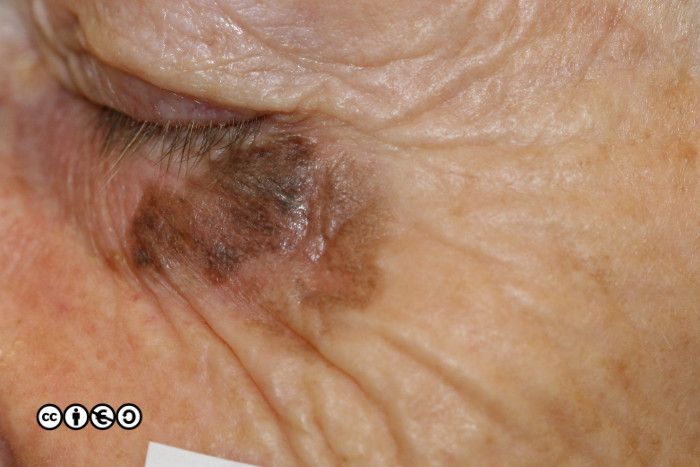
Lentigo maligna melanoma. This refers to melanoma on continually sun exposed skin, most usually the face or the backs of the hands, in which the melanoma develops on the background of severe UVR damage. They often present as lesions that develop over many years, that show a slow increase in area and gradual darkening in colour. (image below)
( The in situ (i.e. in situ melanoma) counterpart is called lentigo maligna).
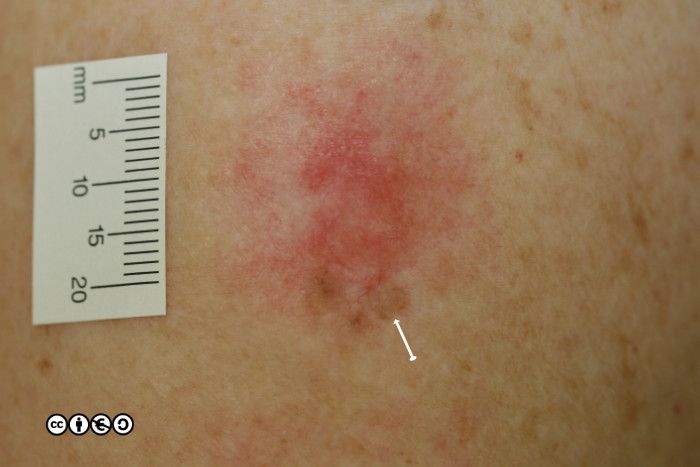
Amelanotic melanoma. Some melanomas (perhaps ~10%) present as largely amelanotic lesions. In reality such lesions usually contain some melanin (see the arrow in the image below) but their differential diagnosis is wide and they are hard to pick up clinically (this should be obvious to you). (image below).
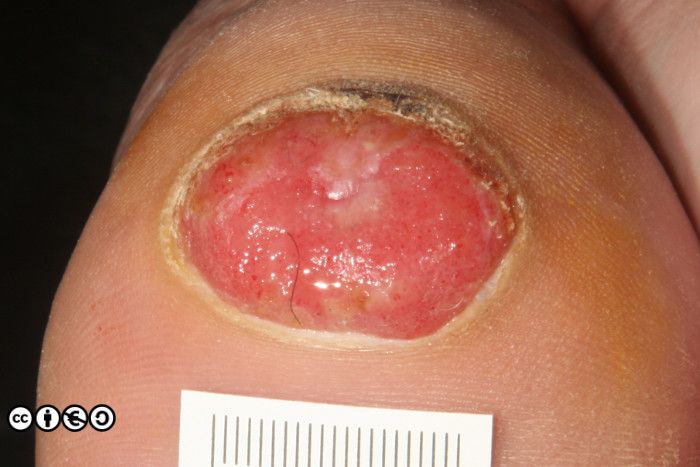
Acral melanoma: these are melanomas on the palms or soles. They have been discussed above. They are usually pigmented, but the large acral melanoma on the heel shown below has no visible pigment. (image below)
The skin cancer body site puzzle
Most skin cancers are the result of UVR exposure (on those with pale skin). However, different types of skin cancers have different body site distributions, and many have mistakenly used this apparent ’paradox’ to argue against the role of UVR in melanoma. I need to explain a little of what is going here, but not delve too deeply, otherwise I might lose your interest.
SCC and actinic keratoses occur most frequently on those body sites with the highest cumulative UVR exposure: bald headed men, tops of the ears, backs of the hands etc. Most BCC by contrast, occur on the middle third of the face. This difference in body site does not negate the role of UVR, but merely suggests other factors are also relevant. For instance, it has been suggested that many BCC are derived from follicular (hair) epithelium. Since the density of follicular epithelium is higher on the face then say the back, then this may be why BCC are most common on the face.
UVR is therefore important but it is not the only factor in determining where BCCs occur.
The issue with melanoma is that most melanomas occur on the legs and the trunk, sites that for most of us only receive intermittent UVR exposure. What is the explanation?
The first factor to consider is the need to adjust for body area. Your torso or legs are, after all, larger in surface area than say your ears! If you adjust in this fashion for surface area, you find that the highest rates of melanoma per unit area are indeed on those sites that receive the most UVR.
However, this fact not withstanding, there are a number of threads of evidence to suggest that melanomas on different body sites differ biologically. That is: melanomas on chronically exposed sites are genetically and biologically different from those that occur on the trunk and legs. For instance, the ratio of melanomas on intermittently exposed sites such as the torso, to melanomas on chronically sun-exposed sites, is higher in young and middle aged persons that in older persons. These torso melanomas also differ genetically from those found in older persons on UVR exposed sites, in terms of the frequency of particular mutations (e.g. BRAF mutations).
Do not worry if you find the above confusing. The take away message is loud and clear: differences in the body site distributions of different skin cancers does not negate the key causal role of UVR in skin cancer.
Prognosis, and the Breslow thickness
The single most important predictor of what will happen to a patient who presents with a melanoma without metastatic spread at the time of diagnosis is the Breslow thickness. The Breslow thickness is the distance measures in millimetres from the granular layer down to the deepest part of the tumour (it is not the diameter of the tumour on the skin’s surface).
Most melanomas present as thin lesions (less than 1mm), and these have the best prognosis (>95% at 5 years). Melanomas with a thickness of 4mm would be considered ‘thick’ and have a much worse prognosis (55% at 5 years). I discuss prognosis again in a later chapter.
Treatment of melanoma (the short version)
The treatment of malignant melanoma is excision of the primary lesion with the overall clinical goal to diagnose melanoma at an early stage before spread has occurred.
Lesions suspicious of melanoma should be excised with a 2mm margin, the sample examined by the histopathologist, and a further excision carried out based on the Breslow thickness if the diagnosis is confirmed. The further excision might require surgical margins of a further 1 to 2cm, depending on the exact Breslow thickness. I will talk more on this topic in the later surgery and therapy chapter.
Carousel of 15 melanoma images
Below are 15 images of melanomas. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.