OK, now we are on to the real heart of this book. Basal cell carcinoma is both common and unusual. We will compare all other cancers with it.
This chapter in one minute
Basal cell carcinomas are keratinocyte tumours whose cells histologically resemble the morphology of basal cells. (This is not the same as saying they are basal cells, but clearly any cancer must contain a fraction of cells capable of long term cell replacement).
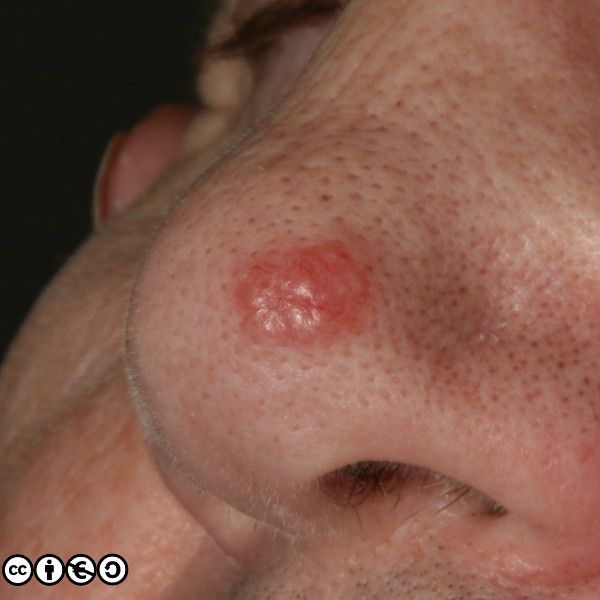
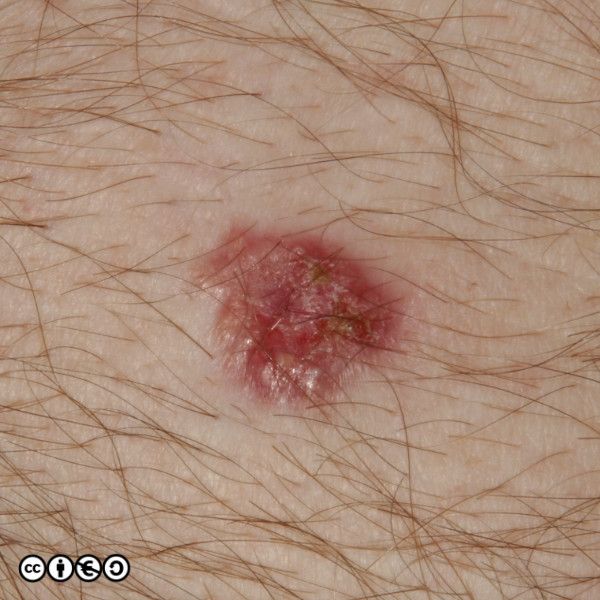
BCCs are the commonest skin cancer and the commonest cancer (of any type) in most European countries. I will show you some images of BCCs before we talk more about their behaviour and how we diagnose and manage them.
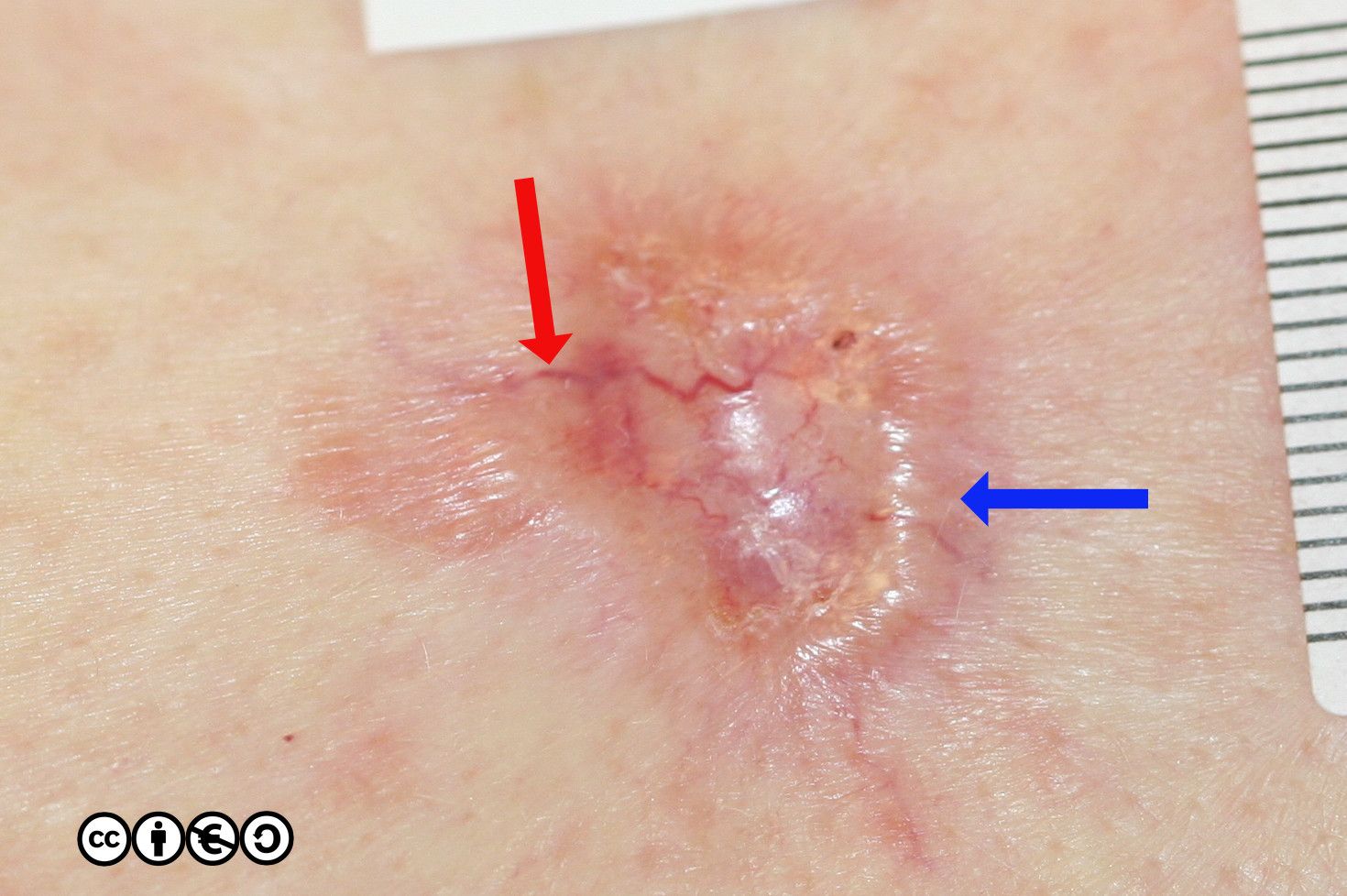
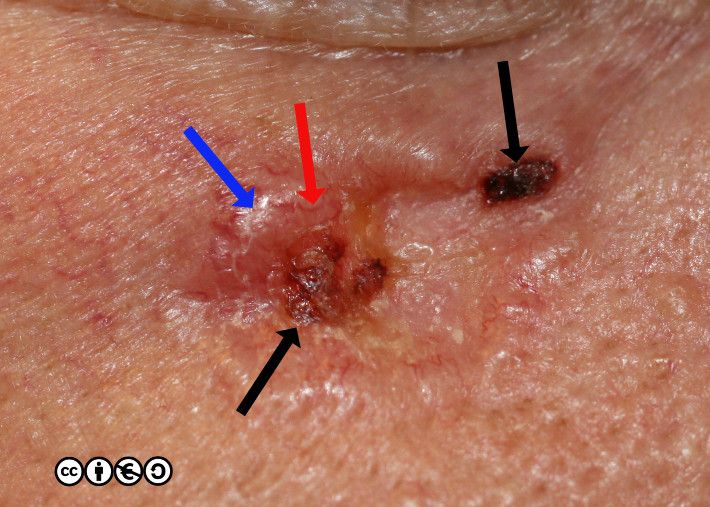
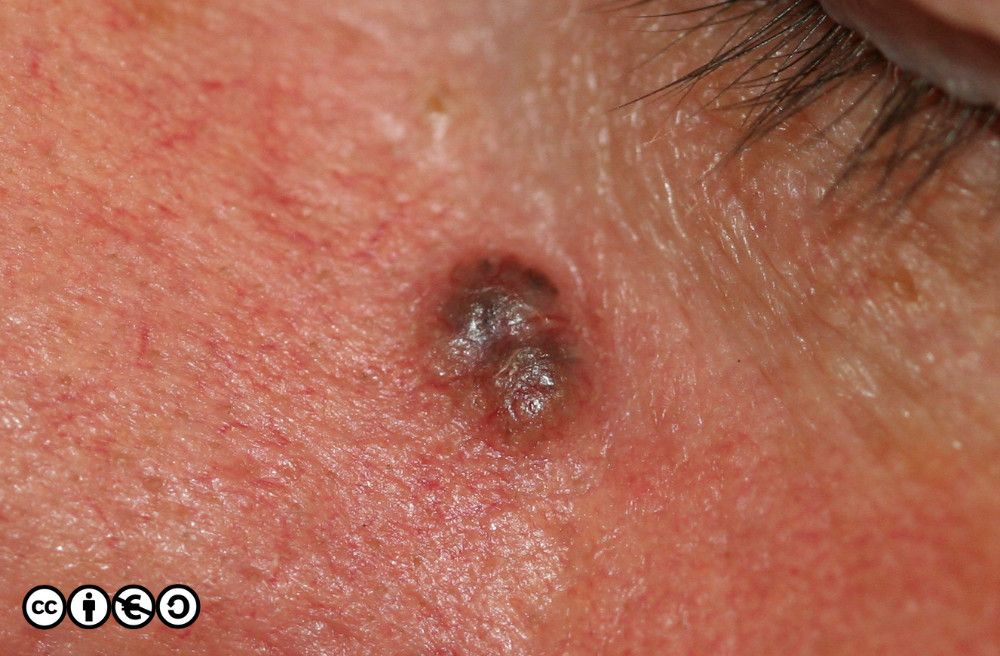
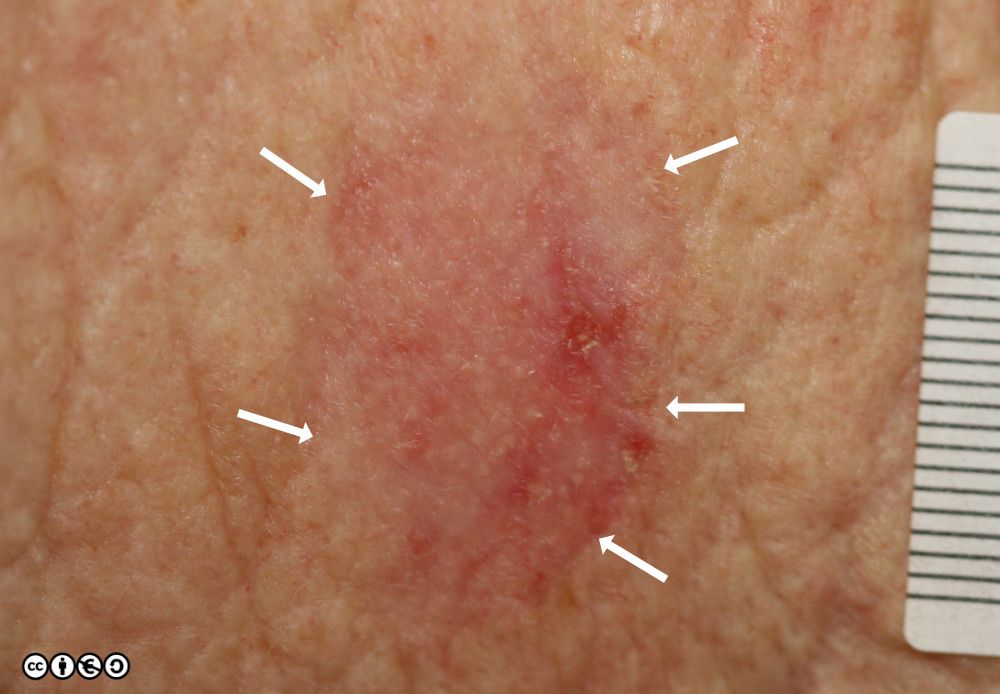
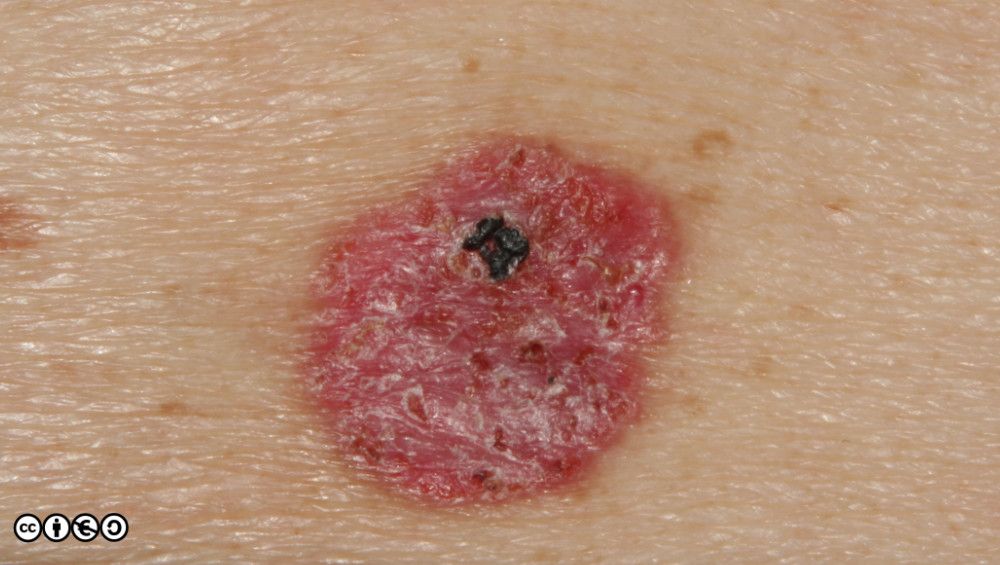
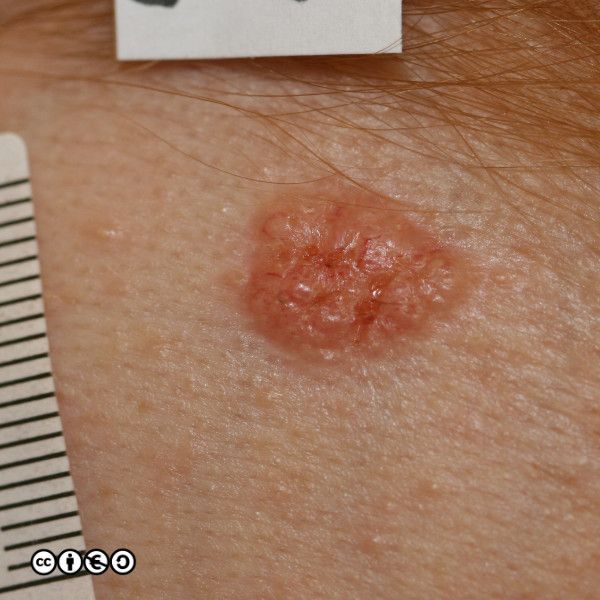
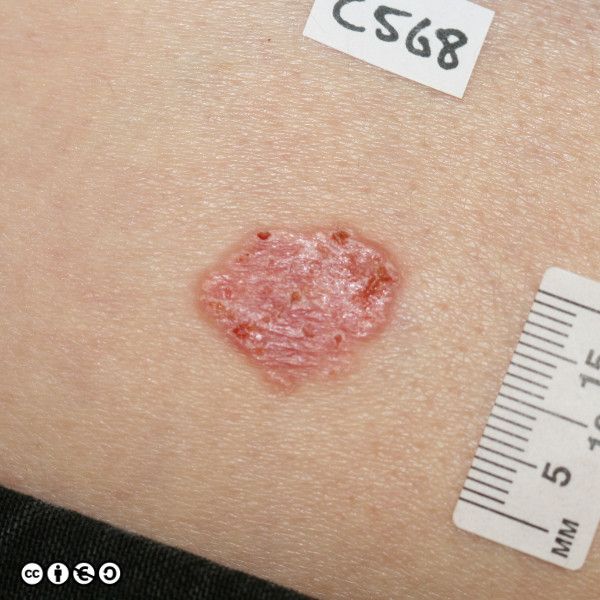
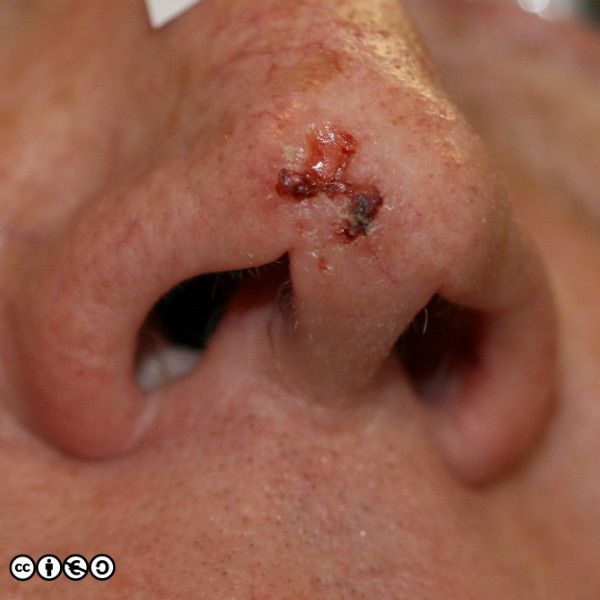
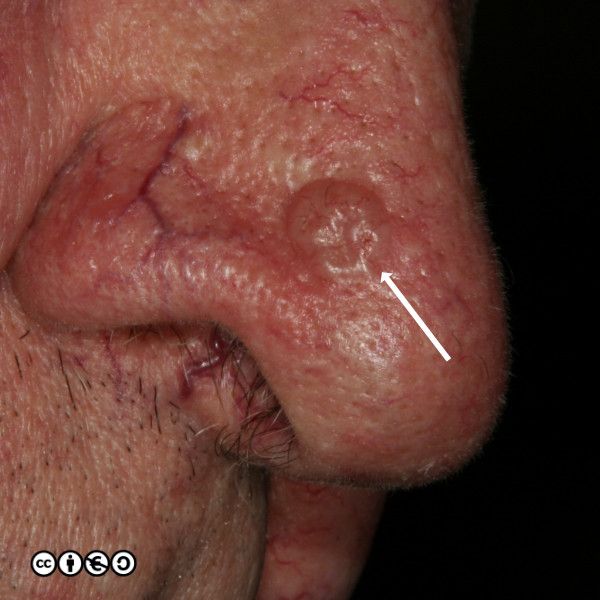
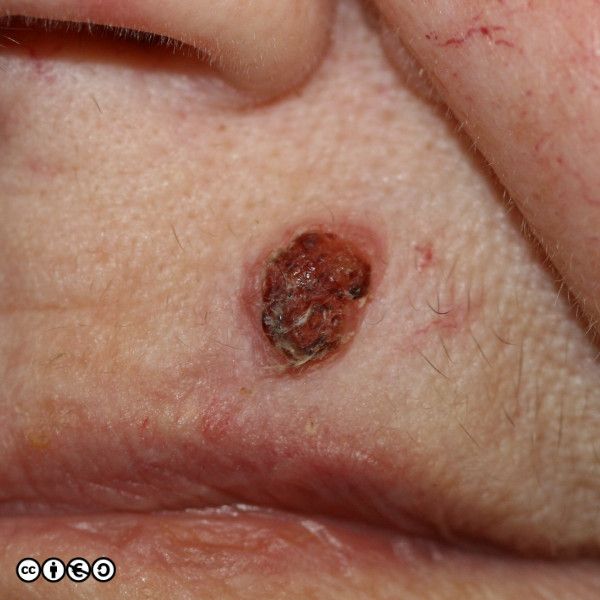
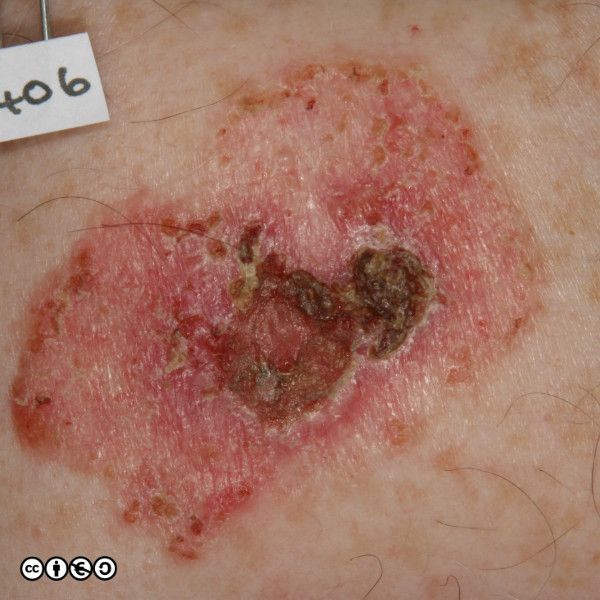
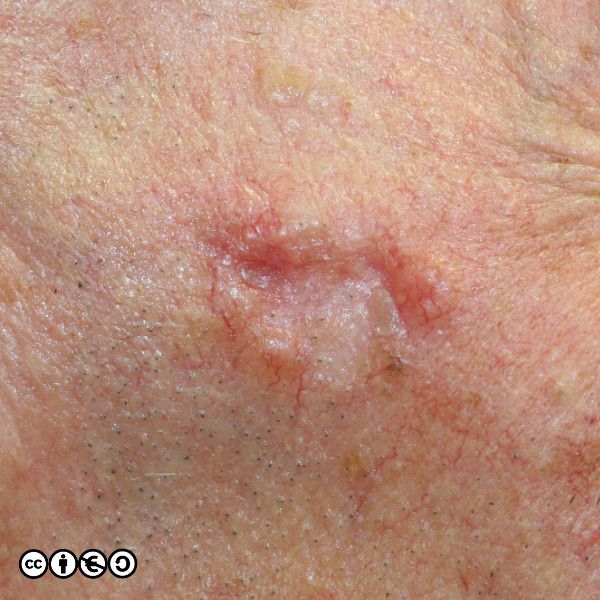
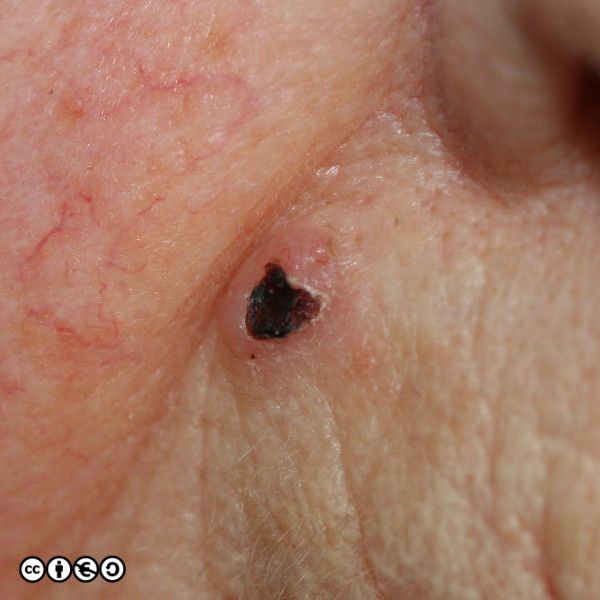
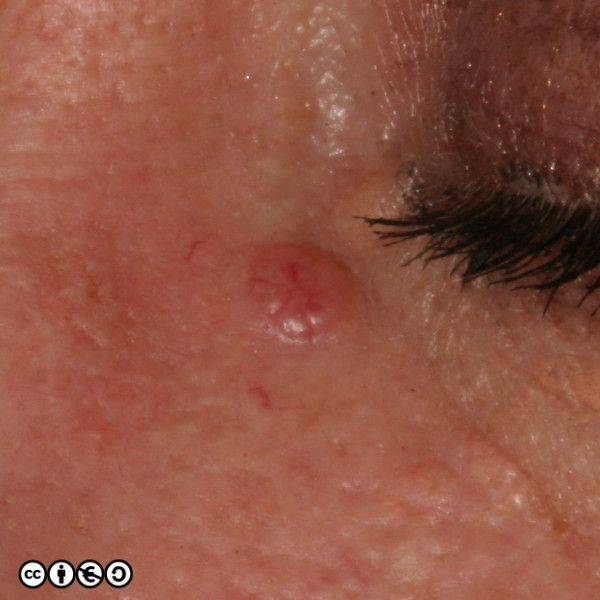
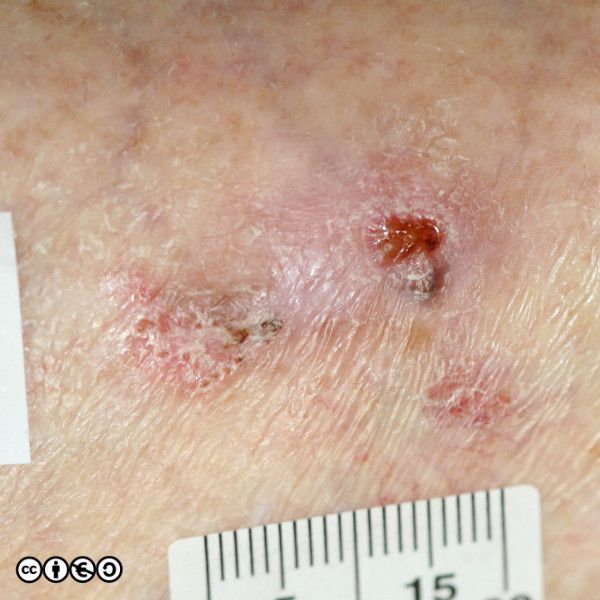
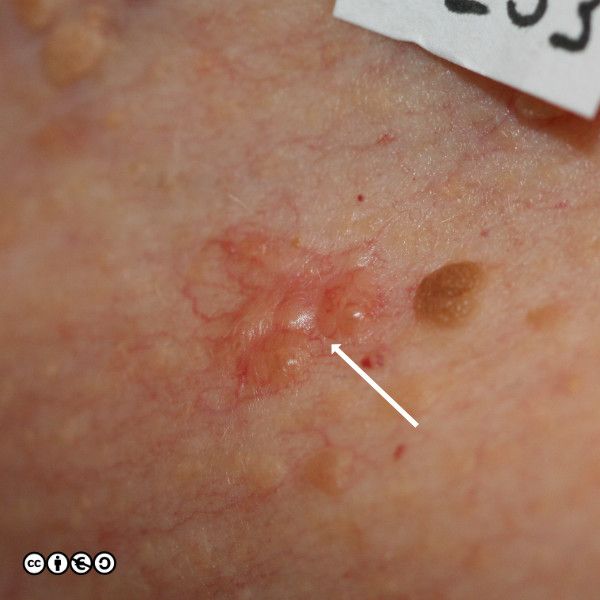
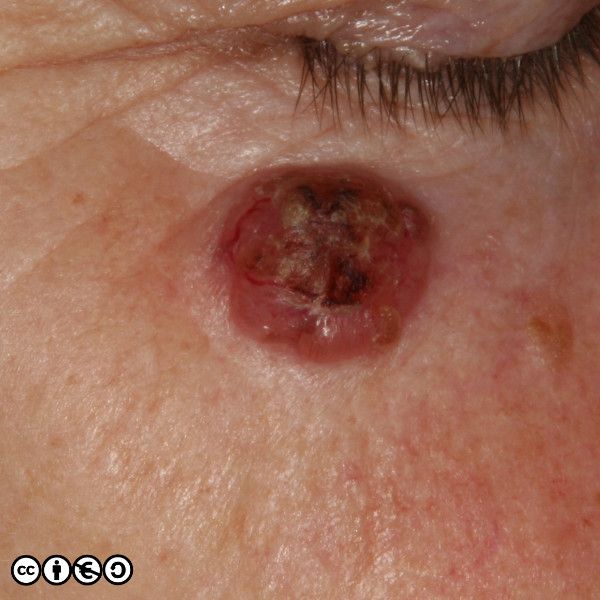
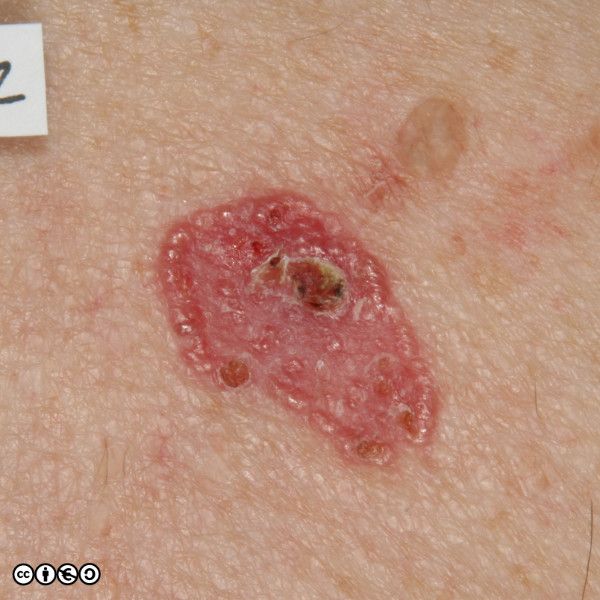
BCCs often have a translucent quality (blue arrow in the images below), and often translucent papules (‘pearly papules’) surround an ulcerated crater (black arrows). Telangiectasis may be prominent (red arrows).
In the image below the ulcerated areas are shown with the black arrows. Telangiectasia (red arrow) and the pearly translucent edge is visible too (blue arrow).
Most BCC are found on the middle third of the face, but perhaps 30% occur on other sun exposed sites too such as the scalp, back, legs and arms. Very rarely they occur on sun protected sites such as the genitalia. BCCs on less frequently affected sites are often harder to diagnose as they look atypical.
The typical BCC measures less than 1 cm across but some are much larger (>5cm) They may appear over a matter of months or over many years growing only very slowly. Sometimes patients will mistakenly rationalise their presence in terms of a cut or episode of skin trauma that has failed to heal.
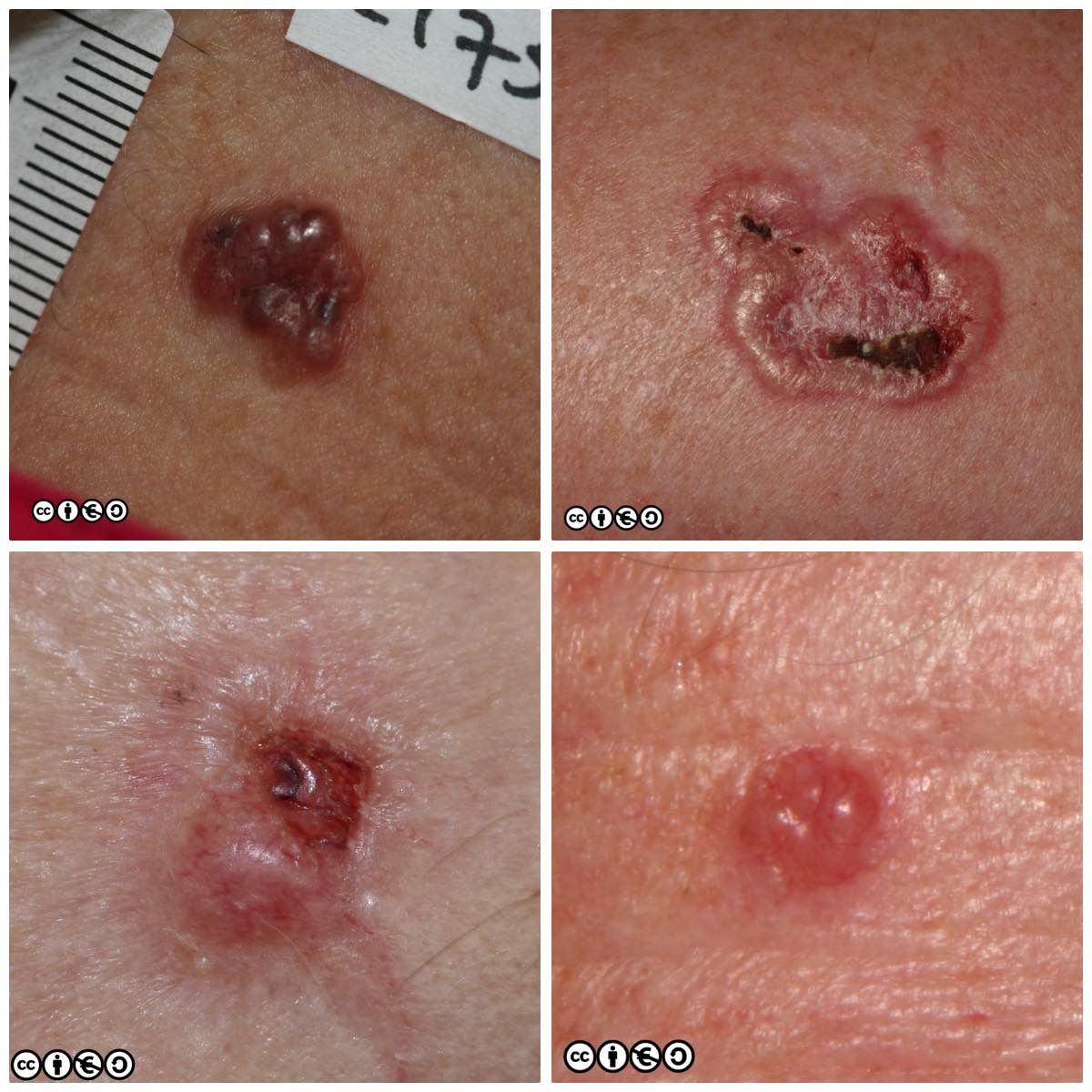
Some more examples of ‘typical’ BCCS are shown below. Try and imagine what they have in common.
Epidemiology
BCC like most skin cancers are UVR related, and therefore they are most common in those with sun sensitive skin, who have received the most UVR exposure.
BCCs are the commonest human cancers with an incidence rate of ~100:100,000 (1:1000) in some Northern European populations. Incidence rates of over 1000/100,000 (1:100) are seen in some Australian populations. For comparison, estimated rates in some parts of Africa are a thousand-fold lower than those seen in Australia. Do not memorize the raw numbers, but appreciate the magnitude of the variation.
The median age of cases is 67, and the sex incidence is equal. BCC incidence increases with age, but in some parts of the world it is not unusual to see BCCs present in those in their late twenties if their skin is pale and there is high UVR exposure.
There are no known clinical precursor lesions of BCCs, but for reasons that should be obvious to you, they are more common in those with other common skin cancers or other premalignant lesions (because most skin cancers are caused by lack of pigment and UVR exposure).
Are BCC true cancers?
BCCs are genuine carcinomas — they are made up of malignant epithelial cells that invade through the basement membrane and can destroy underlying structures such as the eye, cranium or nose. They can even track along nerves into the brain.
However, most malignancies kill due to metastatic spread, and whilst cases of metastatic BCC have been recorded, they are so rare that the everyday management of BCC assumes that metastasis will not occur.
As we shall see later, there is a clear contrast in clinical and biological behaviour between BCC and the other common cancer types such as squamous cell carcinoma or melanoma.
Do not confuse their almost absolute lack of metastatic potential with BCC being harmless. They are extremely common, they are destructive, and most occur on the central face. They can cause loss of the eye, destruction of the nose and rarely, invade into the brain or erode large vessels. Because they are so common on the central face, surgical excision and reconstruction is frequently challenging. By contrast a small BCC on the mid back presents few significant management concerns.
Not all BCCs look — or behave — the same
Dermatology would be much easier to learn if all instances of a particular diagnosis looked the same, but this is not the case. (Indeed if it were that simple, I would probably be out of work).
For BCCs there are well recognised clinical and pathological subtypes that are of importance to the expert but of less value to students. So, you may across terms such as nodular BCC (as in the images above), superficial BCC and morphoeic BCC. These subtypes influence BCC behaviour and our management, but students do not need to delve deep into this topic.
Nodular BCC: These are usually the classical BCC that are often shown in textbooks: the four images above are of classical nodular BCCs. The clinical and tumour margins are often well defined and excised using conventional surgical approaches, with low rates of recurrence.
Morphoeic BCC: Defining the edge of these tumours is often tricky (as it is ‘blurred’), and sometimes they can be several centimetres (yes, centimetres) larger than they first appear. This means that confidently defining the edge to allow an excision with the appropriate margin may be impossible. Mohs’ surgery would appear more appropriate (for a discussion of margins and Mohs’ surgery see this later chapter).
Superficial BCC: These are relatively more common on the back and limbs. They do not show any significant induration and, as we will learn later, cryotherapy and chemotherapeutic agents may be more appropriate than surgery for some of these tumours.
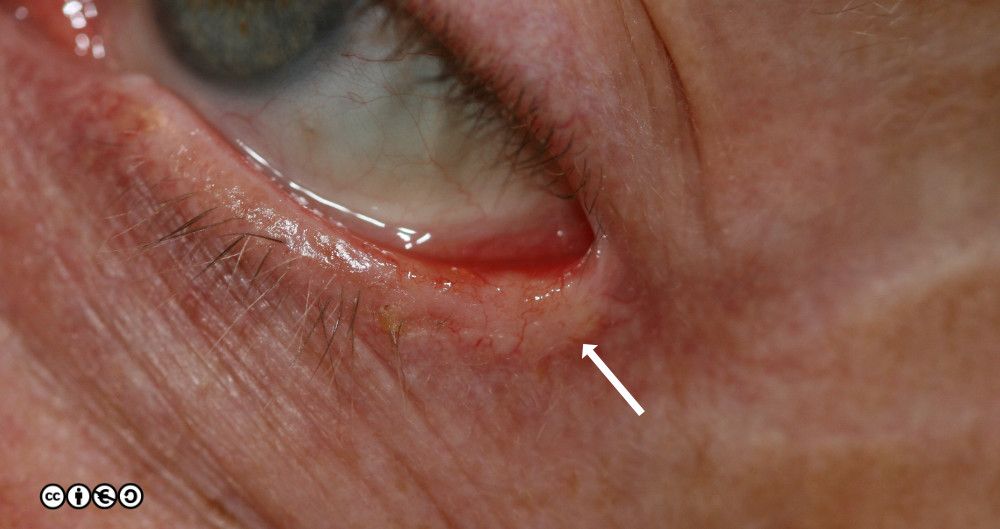
The images below — together with the ones you have already seen — give you a feel for the range of clinical presentations of BCCs.
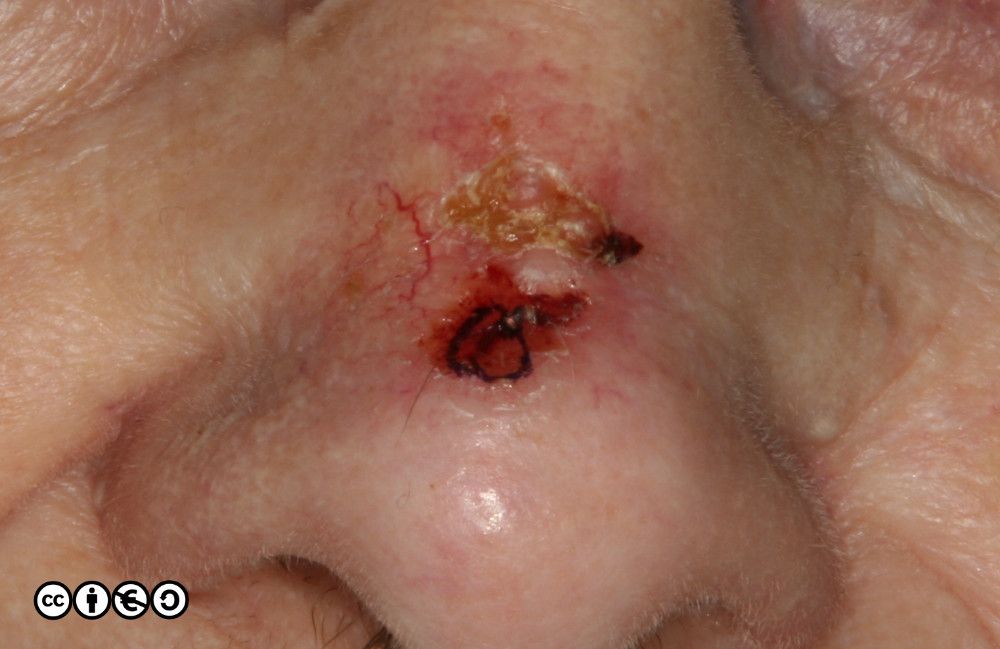
A morphoeic BCC on the nose (the dark pigment inferiorly is ink prior to biopsy). Such tumours are aggressive and recurrence rates higher than for nodular BCCs). Mohs’ surgery is a favoured approach for management of these tumours (discussed in a later chapter).
Treatment of BCC (the short version).
Confirmatory histopathology is required in virtually all cases especially for the non-expert.
BCC cannot always be reliably distinguished from a number of related tumours (especially benign appendageal tumours).
The treatment of choice for most BCCs is excision with a 4mm margin. There are lots of caveats to this statement, however. There are alternatives, including cryotherapy, radiotherapy and topical chemotherapeutic agents. At this stage I do not want to overwhelm you, so we will return to this topic in the later surgery and therapeutics chapter.
What to say to patients who have a BCC (< 4mins)
You might think this is self-evident, but I disagree. In this very short video I explain why you have to give patients a positive diagnosis and explain what a particular lesion is not.
Some other things about BCC I should have mentioned
BCCs are more common in those who are immunosuppressed, especially those who have undergone organ transplantation (as is the case for many other skin cancers). The increase in risk is not as great as for squamous cell carcinoma.
There are rare inherited syndromes that feature BCC. The most important is Gorlin’s syndrome, also known as the Basal Cell Nevus Syndrome (OMIM # 109400). This syndrome is inherited as an autosomal dominant and is due to a mutation in the patched (PTCH ) gene that plays a key role in epidermal physiology. Clinically these patients present with a large numbers of BCCs at a young age and show small pit-like abnormalities on their palms as as well a variety of extracutaneous abnormalities and dysmorphic facies. There may not be any family history as new mutations are common and expressivity varies. The first ‘hit’ is inherited and the second is the result of UVR. (This topic has been discussed in the ‘Bench to clinic’ chapter).
A history of a previous BCC or other type of skin cancer means that any patient is at an increased risk of a further tumour — this simply reflects past UVR exposure and genetic (pigmentary) susceptibility. Because BCCs are so common, it is not at all unusual to diagnose more than one BCC on a patient at the same time. My highest figure was a patient referred with a single tumour who had another 22 on a full skin examination. Over time he developed more, even though he had no detectable inherited syndrome such as Gorlin’s syndrome.
Carousel of 15 BCC images
Below are 15 images of BCCs. Click the (faint) arrows / chevrons half way down on the right or left sides of the image (or the grey-blue dots at the bottom of the image) to navigate. On an iPad ‘swipe’ sideways.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.