This chapter provide a précis of the whole book, a short video of the key points about skin cancer, and a note about what skills the clinician (and medical students) requires. Finally, I outline the structure of skincancer909 and how I think you may get the most from it.
Skin cancer in five minutes
Skin cancer in less than 400 words
In many populations skin cancer will affect close to one in four persons sometime during their life: skin cancer is the commonest cancer in most pale-skinned populations. Many more than this one in four will worry about skin cancer or be seen by doctors with a skin lesion that might be skin cancer. In some health care systems — like the UK — skin cancers account for over half the referrals from primary care to the local hospital dermatology centre.
Most skin cancers are the result of the interaction between:
- exposure to ultraviolet radiation (UVR), and a
- relative absence of the protective pigment melanin.
The higher the UVR exposure and the paler the skin, the higher the rates of skin cancer.
Skin cancers fall naturally into two groups.
- Malignant melanoma (MM) skin cancers are derived from the melanocytic lineage, are relatively uncommon but have a significant case fatality. (Terminology: melanoma and malignant melanoma are the same thing — there is no such thing as a benign melanoma)
- A group of tumours collectively referred to as non-melanoma skin cancers (NMSC) which are usually keratinocyte derived, and much more common than melanoma, but have a much lower case-fatality rate.
The diagnosis of skin cancer largely depends on clinical observation and to a lesser degree clinical history. Histopathology is required in virtually all cases to confirm or refute clinical impressions of skin cancer, but is still not necessary in the assessment of most suspicious lesions seen by experts (i.e. experts only biopsy a minority of the ‘suspicious’ cases they see).
The main modality of treatment for most skin cancers is surgery and for non-melanoma skin cancer this is usually curative. For melanoma, surgery is only curative if the tumour is confined to the primary site (i.e. it has not metastasised). Most skin cancers can be cured, but since the face is frequently affected, advanced surgical skills including reconstructive techniques (i.e. flaps and grafts) are a key component of many dermatologists’ clinical skill set.
Both clinical diagnosis, and pathological diagnosis, rely on perceptual expertise, and owe little to the rule-based-reasoning strategies so common in some other branches of medicine. The ability to distinguish between diseases, and between disease and normality is the key clinical skill.
Clinical skills in dermatology rely almost entirely on the ability to recognise and interpret what we see with our eyes.
Two domains of specialist knowledge
The above brief account implies that clinical expertise in this area is made up of expertise in two distinct domains: perceptual skills, and basic science or clinical knowledge. These two distinct domains of specialist knowledge meet in the clinic. The science provides the conceptual framework in which to organise and interpret what you see, and allows you to explain to patients what will happen to them with and without any intervention. You cannot reason about patients without the framework that science provides. However, without the necessary perceptual skills you will literally not know what you are talking about. Read that last sentence again.
Medical students are used to learning the ‘facts of science’ and explicit rule-based clinical schemas that are now common in many branches of medicine. They are often confident of their abilities to assimilate such information. Acquiring perceptual skills is however often more challenging, and consequently learning dermatology is often viewed as hard. In the following few paragraphs I try to explain how skincancer909 aims to make this process if not pain free, less intimidating. The following paragraphs provide the kernel of the design approach I follow — please read through them.
Layout of skincancer909, chapter by chapter
Skin structure: I describe the the basic cell biology of skin, with the focus on the epidermis — most skin cancers are epidermal in origin.
Sunburn, DNA, and cancer: explores the basis for sunburn and relates how UVR induces DNA damage. I use the rare disorder xeroderma pigmentosa to pick apart the chain of causality between UVR, DNA damage, sunburn, freckling and skin cancer. The chapter also includes a necessary primer on the physics of UVR.
Skin pigmentation: Variation in pigmentation — together with variation in UVR exposure — is the main determinant of skin cancer incidence. I explain the origins of human pigmentation, the biology of the melanocyte, and the relation between the different types of melanin and skin cancer risk. Albinism is used as a case study to tease open the causal pathways.
Bench to clinic: I recapitulate what we have already covered, showing how based on the simple models presented in the previous two chapters, we can make a number of useful clinical predictions about skin cancer. I also cover some key genetics about skin carcinogenesis, as well as highlighting the the contribution an intact immune system plays in ‘preventing’ cancer.
Skin surgery & therapy part 1: The main modality of treatment of skin cancer is surgery. Before learning more about skin cancer, you need to be familiar with some very basic surgical terms. This chapter fills this gap. A later chapter on surgery (part 2) will deal with the more advanced aspects of skin cancer therapy.
Basal Cell Carcinoma: Basal cell carcinomas (BCC) are the commonest skin cancer. They are also highly unusual in their clinical behaviour and because of this they are a key point of reference for any discussion about ‘skin cancer’.
Squamous Cell Carcinoma: Squamous cell carcinomas (SCC) are the second commonest type of skin cancer. There is a key contrast in clinical behaviour to be made with basal cell carcinoma.
Premalignant lesions: There are no clinically recognised precursors of basal cell carcinomas, but two premalignant lesions, actinic keratoses and intraepithelial carcinomas may progress to squamous cell carcinomas. I also discuss an odd biological entity, the keratoacanthoma, a lesion that morphologically resembles an SCC, but which has a drastically different clinical course.
Melanoma: Melanoma is the most common cause of death from skin cancer. It also remains the most difficult to confidently diagnose. This chapter is an introduction, but we will expand on some of the issues raised, later in skincancer909.
Mimics of skin cancer (2 chapters): Skin cancer diagnosis is made so difficult because of the myriad of benign skin lesions that affect most humans. Prepare for the ride.
Rarer skin cancers: The cancers dealt with already account for 98% of all skin cancers. For completion, this chapter tells you about some of the rarer ones such as Kaposi’s sarcoma and the other virus related cancer, Merkel Cell Carcinoma.
The clinician’s approach: I talk about the theory behind skin cancer diagnosis, signal to noise ratios, why diagnosis is difficult, and what you can do to get better at it. I recap on some of the popular heuristics such as the ABCD method that are said to aid diagnosis.
Skin surgery & therapy part 2: We are on the home stretch, moving on from diagnosis to advanced surgery and non-surgical management.
Skin cancer prevention (2 chapters): I discuss primary and secondary prevention. We cover UVR protection, the physics of ambient UVR (again), and human behaviour. I then discuss what we know about screening or informal detection of skin cancer.
Virtual clinics: These are some slide shows in video format to test your knowledge.
Learn more: A guide to further reading and some ‘extra’ material.
Questions, answers, questions
Avoid re-reading just for the sake of it. Instead, try answering the questions. Students are obsessed by MCQ format questions — because they dominate their exams — but the evidence is that open ended questions are a much better way to reinforce learning. For the questions, I provide short textual answers on the attached PDFs, but I also provide short (talkover) videos in which I can explain my reasoning more thoroughly. See what you think.
Videos
I make use of different types of videos: direct talking to camera; talkovers; quizzes; demonstrations, as well a few in which I meet my doppelgänger. Sometimes I cover similar content in the video and the text, although the style and level of detail differs. The placeholder will always tell you how long a video lasts……and there are no adverts. Personally, I would watch the video first before reading the text.
And yes, some of the ‘This chapter in one minute‘ videos are a wee bit over one minute.
Learn more
I provide a guide to further reading and some material that is not core, but which you might find interesting. If Botox is your thing, you might want to explore this a little more. I draw the line at ‘scrotox‘ however.
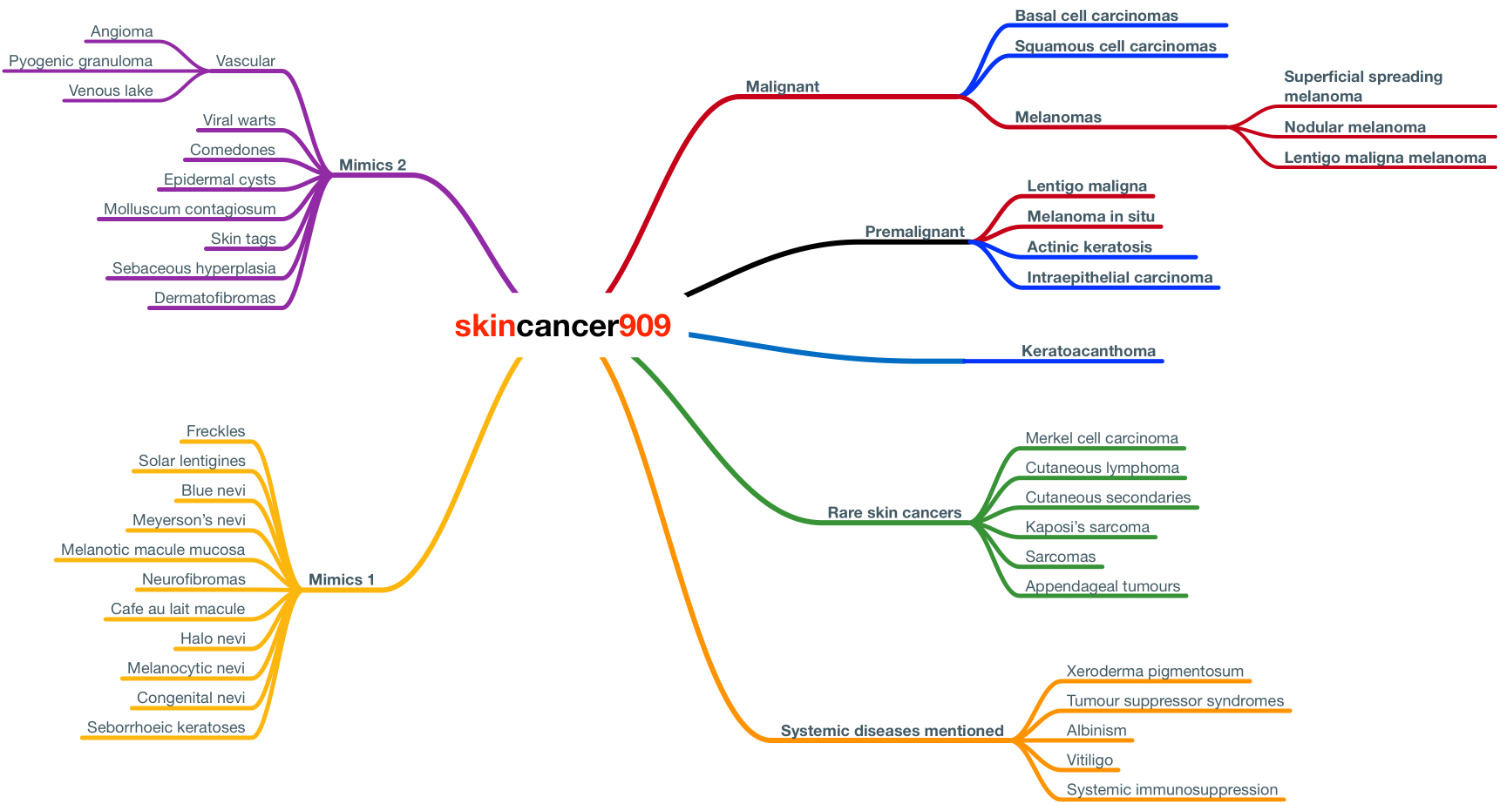
Mindmaps
If you like mind-mapping, below is a simple visual display of the disorders mentioned in skincancer909. The ones on the right hand side, starting on the top, are the most important. You only need to know a small amount about some of the diagnoses on the left. Click on the figure to see a larger version within the browser. You can download a PDF version by clicking here. This figure is not meant to induce a state of panic nor despair.
Skincancer909 by Jonathan Rees is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. Where different rights apply for any figures, this is indicated in the text.