Chapter 8
Common mimics of skin cancer
Common as skin cancer is, it is dwarfed by the prevalence of benign lesions that frequently mimic the appearance of skin cancer. Here we are talking about melanocytic nevi, freckles, benign keratinocyte tumours such as seborrhoeic keratoses, haemangiomas, and a host of other often fairly banal lesions. Even common warts — especially in the elderly — can be confused with skin cancers. For every patient referred to secondary care because of concern that a lesion might be a melanoma, more than 20 will have been false positives — they will turn out to have harmless benign mimics of melanoma.
In this chapter I describe the most important of these mimics. With the exception of melanocytic nevi, which have an importance because of their relation to melanoma and sunshine, few of these mimics of skin cancer have any intrinsic interest except that knowledge of them is clinically important because they are frequently confused with skin cancer. So, scientifically they may indeed be a little dull, but anybody who treats patients is obliged to know something about them. Often, all you need to know is their name and how to recognise them — sometimes easier said than done.
Terminology
It is with some professional embarrassment that I point out that for some benign lesions we are unsure whether they are benign clonal neoplasms or hamartomas. For others, such as solar lentigines there is debate about their actual pathological nature in terms of which ones are real lentigines (that is linear proliferations of melanocytes in the basal layer) versus what some believe them to be, flat seborrhoeic keratoses. From a student’s perspective try and avoid the controversy, keep your head down, and use the names suggested below.
Brown Marks
Freckles
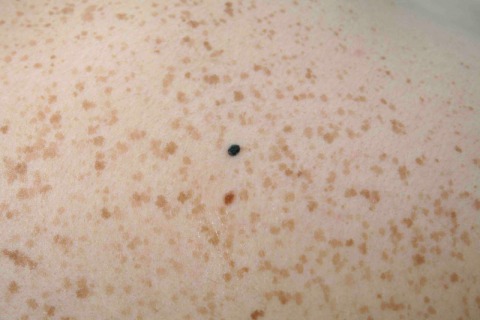
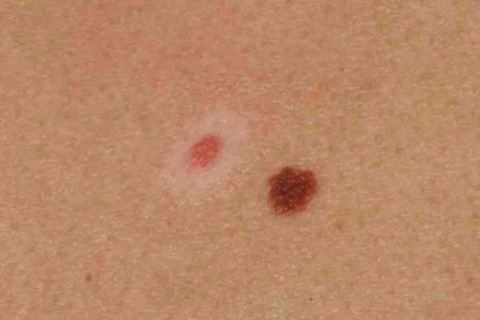
Freckles are flat (macular) focal areas of overproduction of melanin. The number of melanocytes is not increased (cf with lentigo in which there is an increased number of melanocytes). Freckles are the result of sun exposure in those with sensitive skin. Therefore you can expect to see freckles most commonly in red headed persons who live in areas with high ambient sun exposure and a history of sunburn. It is therefore obvious that they are markers of skin cancer risk. Freckles are most common on the face, shoulders and arms. They darken in response to sunshine. They rarely enter into the differential diagnosis of skin cancer
Freckles such as these rarely cause diagnostic confusion. They are of course a marker of sun exposure on the background of sun sensitivity. The darker lesion in the middle is a blue nevus (discussed later in this chapter).
Seborrhoeic keratoses (basal cell papillomas, seborrhoeic warts)
These are benign keratinocyte tumours some of which are known to harbour particular mutations. Clinically they vary from being almost flat to being raised by up to a centimetre. They have a stuck on appearance, and a warty (highly irregular) surface, and often appear ‘greasy’ (hence the name seborrhoeic, even though they have nothing to do with sebaceous glands). They are most common on the trunk but can occur on the face and limbs, but not on the palms or soles. They start to appear in early middle age and increase as the years go by.
Some patients may have hundreds of them. They can virtually mimic any skin cancer including BCC and SCC, but they are frequently confused with melanoma. They may itch or bleed, they are usually irregular in shape, edge and pigmentation and change over time — hence they often fulfil the ABCDE criteria for melanoma. Most putative melanomas referred from primary care to secondary care will be either be seborrhoeic keratoses or melanocytic nevi.
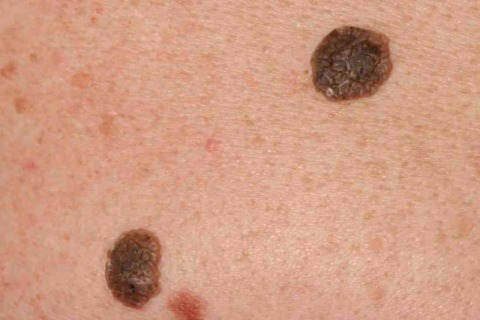
Seborrhoeic keratoses are often greasy in appearance and have a rough craggy surface. On the image on the left the larger brown lesion is a seborrhoeic keratoses, and there is a small melanocytic nevus inferiorly. On the righthand image the larger lesion is a seborrhoeic keratosis.
Solar Lentigines (single is lentigo, plural lentigine)
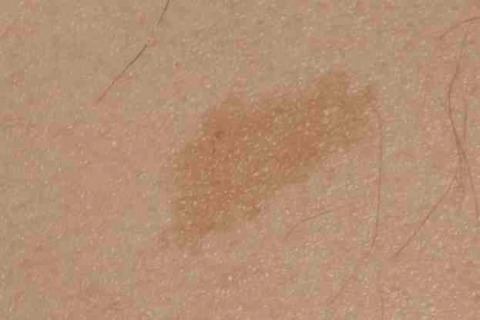
These are flat or almost flat brown marks most common on the backs of the hands, forearms and the face. They reflect previous sun exposure and the surrounding skin may show other features of sun damage. Some of these lesions may be true lentigines in that there is a proliferation of melanocytes, whereas others appear to be almost flat seborrhoeic keratoses with a slightly warty appearance visible if examined with a lens. Their medical significance is that if they are flat and without any warty appearance they can be easily confused with lentigo maligna (in situ melanoma on sun exposed skin, most commonly the face). A history of growth and increasing dark and variable pigmentation suggest that an expert opinion is required. They are almost ubiquitous after middle age in sun sensitive patients. If an index lesion looks like lots of others on the patient’s skin it is very unlikely to be a melanoma.
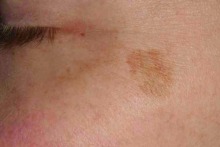
If you look carefully you will see there is more than one lentigo on the face of the patient in the left image (closer to the eye than the main circular lesion). The image on the right shows multiple lentigines on a background of obvious photodamage.
Melanocytic nevi (‘moles’)
Melanocytic nevi are focal collections of melanocytes clustered in a nest (or ball like clump) that may or may not produce pigment. Many melanocytic nevi are clonal and harbour mutations in growth controlling pathways. They are by definition benign. Some nevi are present at birth or appear soon after birth and are know as congenital melanocytic nevi. These occur in a few percent of the population and are harmless unless they are very large (>10cm) when they may (rarely) may undergo cancerous change.
Acquired melanocytic nevi are not static throughout life. They typically start to appear in childhood,reaching a maximum in the third and fourth decades. In early life they are often flat and dark, before becoming raised whilst still being pigmented, before losing their pigment but remaining raised. They can take on a myriad of morphologies and can often resemble seborrhoeic keratoses with a very warty appearance. Melanocytic nevi are more common in those with a history of greater sun exposure in childhood.
Their medical significance is that perhaps half of melanomas arise in preexisting melanocytic nevi, and that many melanomas, even if they do not arise in a known melanocytic nevus, may be difficult to distinguish from a benign melanocytic nevus (distinguishing melanocytic nevi from melanoma is discussed in the earlier chapter on melanoma). There are lots of descriptive names applied to different types of melanocytic nevi which you are advised to skip over.
Melanocytic nevi have an enormous range of morphologies — which is one of the reasons why differentiating them from melanomas can be so difficult.
Atypical or dysplastic nevi
Nobody can agree on what these terms mean in a clinically useful way. They can refer to either a clinical or histopathological appearance but their is little overlap between these usages. The term was meant to embrace a melanocytic nevus that seems unusual in appearance and is reminiscent of a superficial spreading melanoma. The implication being that this type of atypical or dysplastic nevus is in danger of progressing to melanoma. Some patients seem to have lots of such nevi. In practice a large proportion of the population seem to have melanocytic nevi that meet the criteria for dysplastic nevi and there is little consistency between dermatologists. In practice, if you think a melanocytic nevi is suspicious of melanoma, say that and act on it. Expunging terms form the lexicon is hard!
Blue nevi
Melanin deep in the dermis appears blue due to light scattering (we met this phenomenon in earlier chapters). Melanocytic nevi therefore that are deep in the dermis appear blue. They often appear in childhood, and are more common in some Asian populations. However a new onset blue nevus in middle age or older should be looked upon with suspicion: could this be a nodular melanoma? Physical signs alone will not always allow a clear distinction.
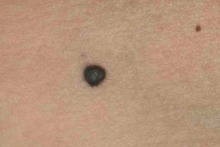
The hint of blue colour was more obvious for both these lesions in real life rather than on these photographs. It is easy to see how these lesions may be confused with melanoma if there is no history available.
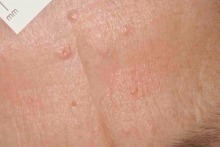
Halo nevi
These are melanocytic nevi that appear to be under immune attack from the host with destruction of melanocytes. They are easy to diagnose. They are of no clinical significance except that halo nevi may appear in patient with a melanoma elsewhere — examine the whole skin of such adult patients. They are common in childhood and harmless. Some melanocytic nevi become surrounded by what appears to a patch of eczema although there is not a halo present (known as a Meyerson’s nevus). These again seem to represent some form of host response to a nevus and is of no great medical consequence.
Note the depigmentation around only one of the two melanocytic nevi.
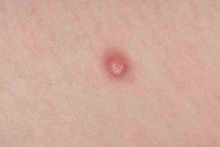
Spitz nevus
A type of melanocytic nevus. Typically a reddish brown nodule in a child or young adult. They are most common on the upper arms or face.They are benign but histologically very unusual and easily confused with melanomas even by expert dermatopathologists. Their terminology is confusing.
Melanotic macules of the lips
These are macules of increased pigmentation seen on the lips (and the genitalia). Usually multiple, solitary lesions can be confused with melanomas or venous lakes
Café au lait macules
These are light brown macules measuring from one centimetre upwards to 10cm or more. They are present in up to 10% of the normal European population, and are present form early childhood. If more than five are present consider neurofibromatosis and check for axillary freckling and neurofibromas.
Other benign skin lesions
Haemangiomas and pyogenic granulomas
These are both vascular lesions, the former probably some form of hamartoma, the latter an abnormal vascular response to trauma. Haemangiomas such as the bright red Campbell de Morgan spots are extremely common and rarely get confused with anything more sinister. However in later life many people develop vascular papules or nodules that can mimic melanoma. If you can confidently remove the blood by pressure (and often the lesion will collapse and shrink temporarily in volume after you do this) you do not need to worry further. If not, you need advice. One variety referred to as a venous lake, is commonly seen on the lips, is easily compressible and is often confused with melanotic macules of the lips (which are not compressible).
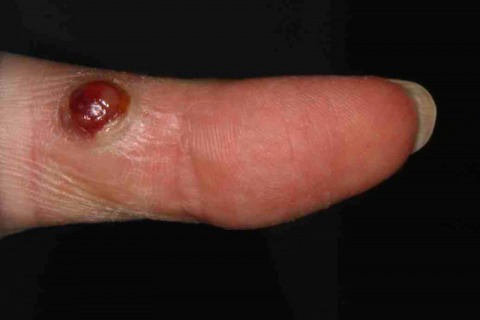
Pyogenic granulomas are best viewed as a vascular proliferation in response to wounding, in which the vascular granulation tissue continues to grow inappropriately. They can occur in patients of any age, and at any body site but are most common on the fingers in the young. They vary in appearance from a bleeding red raw liver like piece of meat, to, with time, a more organised nodule that may be confused with other types of angiomas. They can mimic amelanotic melanomas or pigmented melanomas, and it is not too uncommon for a presumed pyogenic granuloma to be curetted, only for the pathologist to report the specimen as a melanoma. Pyogenic granulomas occurring in childhood are more confidently diagnosed. The history of trauma is not always apparent.
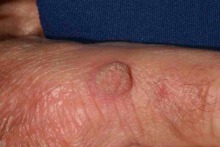
Viral warts
These are the common warts of childhood secondary to human papillomavirus infection (HPV). New warts may develop in older persons and can be confused with AKs, seborrhoeic keratoses or even SCCs. Patients who are immunosuppressed are at an increased risk of NMSC and have a much higher prevalence of viral warts. Clinical assessment can be difficult in these patients, and diagnostic suspicion is warranted because an SCC may be misdiagnosed as a benign viral wart.
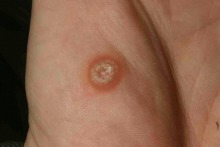
It is not always possible to be certain of the diagnosis of a simple viral wart without
pathology. The lesion on the left is straightforward, but the viral wart on the right could have
been a seborrhoeic keratoses or even a squamous cell carcinoma.
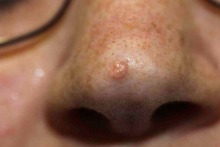
Sebaceous hyperplasia
These are clusters of enlarged sebaceous glands most common on the face. They vary in size between 2-6mm. They have a characteristic translucent and yellow colour and an umbilicated or rosette like shape around a central follicular orifice. They are easily confused with small BCCs by the overconfident. They are often multiple.
Dermatofibromas
These are firm nodules up to 1cm or more across that appear attached to the epidermis (you cannot pinch the epidermis separately from them, and the skin dimples when you pinch them). They may be skin coloured often show increased melanin pigmentation or annular rings of melanin pigmentation. They are most common on the arms and legs. Histologically they show a proliferation of fibroblasts in the dermis and some believe they are a late response to insect bites rather then a neoplasm. A big clinical clue is that they are much firmer than many other nodules, and that they feel bigger than they look. They are usually misdiagnosed as melanocytic nevi.
Skin tags (acrochordons)
These are focal overgrowths of epidermis and dermis. Usually multiple and common in flexural areas especially in the obese. They may have histological features of seborrhoeic keratoses or melanocytic nevi.
- What is the differences between a Spitz nevus and a blue nevus?
- Are seborrhoeic keratoses rich in sebaceous glands?
- What happens if you pinch a dermatofibroma?
- What site is particularly common for pyogenic granulomas?
- How could you tell the difference between a venous lake and a melanotic macule of the lip?
- Do clinical atypical nevi show dysplasia?
- Name two risk factors for freckles
- At what age are melanocytic nevi most prevalent?